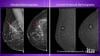
Interview with Gerald Kolb, JD, president of The Breast Group in Bend, Ore. Kolb spoke at the 2016 AHRA meeting in Nashville about the challenges of multimodality breast screening, the need for more personalized screening programs and the impact of recent screening recommendations. Read about the lastest advances in breast imaging.
Recent Videos View all 676 items
Radiology departments have many different needs and face a wide variety of challenges that can impact their departments, staff and patients.
Bayer Radiology’s Customer Engagement Team works with its customers to find the right solutions to meet their specific needs. The Team is made up of engineering, manufacturing and clinical experts who can provide creative solutions to the most complex challenges.
In this video, Thom Kinst and Barbara Ruhland discuss how Bayer Radiology’s Customer Engagement Team is dedicated to helping customers be successful today and also be prepared for the next frontier of challenges in radiology.
Bayer Radiology’s Barbara Ruhland and Thom Kinst discuss how radiology departments can address the many different challenges and market disruptions they are currently facing and some of the innovative solutions that Bayer can offer them to meet these challenges — including the Medrad Centargo CT Injection System, a multi-patient injector that drives workflow efficiency as well as new products that are in the pipeline.
Postpandemic staffing shortages and increased volumes require radiologists to do more with less, exacerbating burnout. Join Kyle Henson, senior director of imaging at Solis Mammography, for a discussion about the most impactful, practical, cost-effective ways technology can be used to minimize downtimes, help radiologists work more efficiently, and create a dynamic infrastructure to enable organizations to pivot quickly during uncertain times. This webinar discusses how radiologists can save time and minimize downtime.
Learning Objectives:
- Strategies to minimize downtime and optimize reading time.
- The promise and reality of artificial intelligence and where to deploy it for the most significant impact.
- Critical imaging-platform improvements for better performance, flexibility, and overall savings.
Speaker Profile:

Kyle Henson — Senior Director of Imaging, Solis Mammography
Kyle Henson is the senior director of imaging at Solis Mammography. After serving our country as an officer in the U.S. Army, Henson entered into healthcare IT. His 20-year career has included everything from the payer space to PACS vendor, imaging consultant, international speaker, hospitals, and diagnostic imaging centers. He has delivered cloud imaging solutions to all facilities in a 85+ hospital system.
Company Profile:
Change Healthcare is a leading healthcare technology company, focused on insights, innovation, and accelerating the transformation of the U.S. healthcare system through the power of the Change Healthcare platform. We provide data and analytics-driven solutions to improve clinical, financial, administrative, and patient engagement outcomes in the U.S. healthcare system.
Find actionable insights to achieve sustainability and savings in radiology in this newest of ITN’s “One on One” video series with Reed A. Omary, MD, MS, Vanderbilt University Medical Center (Nashville, TN). Tune in to "Promoting the Planet's Health: Sustainability in Radiology," to hear from a recognized leader about impactful, cost-saving initiatives radiologists, associations, healthcare systems and vendors can take, and why action is imperative.
Omary, the Carol D. and Henry P. Pendergrass Professor in the VUMC Department of Radiology, is a distinguished radiologist whose commitment to driving healthcare sustainability initiatives has gained both attention and momentum. After serving as Chair of the Department of Radiology and Radiology Sciences from 2012-2023, in June, 2023, Omary stepped away from his role as Chair to pursue a sabbatical focused on climate change and sustainable healthcare. He is author of The Green Leap, a blog about making healthcare sustainable, and founder of the Greenwell Project, a sustainable healthcare non-profit. He has presented a Plenary Lecture at the Radiological Society of North America (RSNA) Annual Scientific Sessions and American College of Radiology (ACR) meetings on the topic, and continues to connect with healthcare systems, vendors and colleagues to advance the issue.
Related content:
PHILIPS MARKS MILESTONE DURING HELIUM-FREE MRI INSTALLATION IN PUERTO RICO
RSNA 2022 PLENARY SPEAKER OMARY URGES RADIOLOGISTS TO SUPPORT PATIENTS, COMMUNITIES AND THE PLANET
RSNA 2022 PANEL DISCUSSIONS FORECAST RADIOLOGY IN 2027, AND HIGHLIGHT WHY MENTORS MATTER
Sponsored Videos View all 184 items
Radiology departments have many different needs and face a wide variety of challenges that can impact their departments, staff and patients.
Bayer Radiology’s Customer Engagement Team works with its customers to find the right solutions to meet their specific needs. The Team is made up of engineering, manufacturing and clinical experts who can provide creative solutions to the most complex challenges.
In this video, Thom Kinst and Barbara Ruhland discuss how Bayer Radiology’s Customer Engagement Team is dedicated to helping customers be successful today and also be prepared for the next frontier of challenges in radiology.
Bayer Radiology’s Barbara Ruhland and Thom Kinst discuss how radiology departments can address the many different challenges and market disruptions they are currently facing and some of the innovative solutions that Bayer can offer them to meet these challenges — including the Medrad Centargo CT Injection System, a multi-patient injector that drives workflow efficiency as well as new products that are in the pipeline.
Clinicians and referring physicians need fast, secure access to both patient data and their diagnostic or viewing tool set. But the cost barriers and the complexity of owning and maintaining healthcare information systems can compromise the quality of care.
To address this, Philips has partnered with AWS to develop Philips HealthSuite Imaging — a new radiology cloud service that provides on-demand access to advanced medical imaging software.
ITN recently visited with Madhuri Sebastian and Matthieu Ferrant to learn more about this service.
Agfa Radiology Solutions is committed to enhancing clinical outcomes and operational efficiency, underscoring its innovative edge in the dynamically evolving healthcare landscape.
AT RSNA23, ITN met with Karol Wesolowski, Global Commercial Excellence Leader, Agfa Radiology Solutions, and Jeroen Spruyt, Head of BU DR, VP Product Supply and Operations, Agfa Radiology Solutions, to learn more about how the company is transforming radiology practices.
Find more RSNA23 conference coverage here
Related content:
VIDEO: Talking Trends with Agfa — What’s On Tap for RSNA 2023
Technology Reports View all 12 items
This is an overview of trends and technologies in radiology artificial intelligence (AI) applications in 2021. Views were shared by 11 radiologists using AI and industry leaders, which include:
• Randy Hicks, M.D., MBA, radiologist and CEO of Reginal Medical Imaging (RMI), and an iCAD Profound AI user.
• Prof. Dr. Thomas Frauenfelder, University of Zurich, Institute for Diagnostic and Interventional Radiology, and Riverain AI user.
• Amy Patel, M.D., medical director of Liberty Hospital Women’s Imaging, assistant professor of radiology at UMKC, and user of Kios AI for breast ultrasound.
• Sham Sokka, Ph.D., vice president and head of innovation, precision diagnosis, Philips Healthcare.
• Ivo Dreisser, Siemens Healthineers, global marketing manager for the AI Rad Companion.
• Bill Lacey, vice president of medical informatics, Fujifilm Medical Systems USA.
• Karley Yoder, vice president and general manager, artificial intelligence, GE Healthcare.
• Georges Espada, head of Agfa Healthcare digital and computed radiography business unit.
• Pooja Rao, head of research and development and co-founder of Qure.ai.
• Jill Hamman, world-wide marketing manager at Carestream Health.
• Sebastian Nickel, Siemens Healthineers, global product manager for the AI Pathway Companion.
There has been a change in attitudes about AI on the expo floor at the Radiological Society of North America (RSNA) over the last two years. AI conversations were originally 101 level and discussed how AI technology could be trained to sort photos of dogs and cats. However, in 2020, with numerous FDA approvals for various AI applications, the conversations at RSNA, and industry wide, have shifted to that of accepting the validity of AI. Radiologists now want to discuss how a specific AI algorithm is going to help them save time, make more accurate diagnoses and make them more efficient.
With a higher level of maturity in AI and the technology seeing wider adoption, radiologists using it say AI gives them additional confidence in their diagnoses, and can even help readers who may not be deep experts in the exam type they are being asked to read.
With a myriad of new AI apps gaining regulatory approval from scores of imaging vendors, the biggest challenge for getting this technology into hospitals is an easy to integrate format. This has led to several vendors creating AI app stores. These allow AI apps to integrate easily into radiology workflows because the apps are already integrated as third-party software into a larger radiology vendors' IT platform.
There are now hundreds of AI applications that do a wide variety of analysis, from data analytics, image reconstruction, disease and anatomy identification, automating measurements and advanced visualization. The AI applications can be divided into 2 basic types — AI to improve workflow, and AI for clinical decision support, such as diagnostic aids.
On the workflow side, several vendors are leveraging AI to pull together all of a patients' information, prior exams and reports in one location and to digest the information so it is easier for the radiologist to consume. Often the AI pulls only data and priors that relate to a specific question being asked, based on the imaging protocol used for the exam. One example of this is the Siemens Healthineers AI Clinical Pathway and Siemens AI integrations with PACS to automate measurements and advanced visualization.
AI is also helping simplify complex tasks and help reduce the reading time on involved exams. One example of this is in 3-D breast tomosythesis with hundreds of images, which is rapidly replacing 2-D mammography, which only produces 4 images. Another example is automated image reconstruction algorithms to significantly reduce manual work. AI also is now being integrated directly into several vendors' imaging systems to speed workflow and improve image quality.
Vendors say AI is here to stay. They explain the future of AI will be automation to help improve image quality, simplify manual processes, improved diagnostic quality, new ways to analyze data, and workflow aids that operate in the background as part of a growing number of software solutions.
Several vendors at RSNA 2020 noted that AI's biggest impact in the coming years will be its ability to augment and speed the workflow for the small number of radiologists compared to the quickly growing elder patient populations worldwide. There also are applications in rural and developing countries were there are very low numbers of physicians or specialists.
Related AI in Medical Imaging Content:
AI Outperforms Humans in Creating Cancer Treatments, But Do Doctors Trust It?
VIDEO: Artificial Intelligence For MRI Helps Overcome Backlog of Exams Due to COVID
How AI is Helping the Fight Against Breast Cancer
VIDEO: Use of Artificial Intelligence in Nuclear Imaging
3 High-impact AI Market Trends in Radiology at RSNA 2019
Photo Gallery of New Imaging Technologies at RSNA 2019
VIDEO: Editors Choice of the Most Innovative New Radiology Technology at RSNA 2019
Study Reveals New Comprehensive AI Chest X-ray Solution Improves Radiologist Accuracy
VIDEO: Real-world Use of AI to Detect Hemorrhagic Stroke
The Radiology AI Evolution at RSNA 2019
Eliminating Bias from Healthcare AI Critical to Improve Health Equity
VIDEO: FDA Cleared Artificial Intelligence for Immediate Results of Head CT Scans
Building the Future of AI Through Data
Integrating Artificial Intelligence in Treatment Planning
Selecting an AI Marketplace for Radiology: Key Considerations for Healthcare Providers
Artificial Intelligence Improves Accuracy of Breast Ultrasound Diagnoses
Artificial Intelligence Greatly Speeds Radiation Therapy Treatment Planning
WEBINAR: Building the Bridge - How Imaging AI is Delivering Clinical Value Across the Care Continuum
AI in Medical Imaging Market to Reach $1.5B by 2024
VIDEO: AI-Assisted Automatic Ejection Fraction for Point-of-Care Ultrasound
5 Trends in Enterprise Imaging and PACS Systems
VIDEO: Artificial Intelligence to Automate CT Calcium Scoring and Radiomics
Scale AI in Imaging Now for the Post-COVID Era
VIDEO: Integrating Artificial Intelligence Into Radiologists Workflow
Northwestern Medicine Introduces Artificial Intelligence to Improve Ultrasound Imaging
Find more artificial intelligence news and video
In Artificial Intelligence at RSNA 2019, ITN Contributing Editor Greg Freiherr offers an overview of artificial intelligence (AI) advances at the Radiological Society of North America (RSNA) 2019 annual meeting.
In Enterprise Imaging at RSNA 2019, ITN Contributing Editor Greg Freiherr offers an overview of enterprise imaging advances at the Radiological Society of North America (RSNA) 2019 annual meeting.
In Artificial Intelligence 2018: What Radiologists Need to Know About AI, ITN Contributing Editor Greg Freiherr offers an overview of artificial intelligence (AI) advances at the Radiological Society of North America (RSNA) 2018 annual meeting.
Related Artificial Intelligence Content
Technology Report: Artificial Intelligence 2017
VIDEO: RSNA Post-game Report on Artificial Intelligence
VIDEO: AI in Tumor Diagnostics, Treatment and Follow-up
VIDEO: Artificial Intelligence May Help Reduce Gadolinium Dose in MRI
Radiation Oncology View all 108 items
In the conclusion of this 3-part video series on recent advancements in diagnostic radiology, current editorial advisory board member Robert L. Bard, MD, PC, DABR, FASLMS, discusses other advancements in diagnostic radiology and what new technologies are in development that could help in the fight against cancer.
Watch VIDEO PART I: Using 3-D Doppler Imaging and Other Advancements in Diagnostic Radiology
Dr. Bard is internationally known and recognized as a leader in his field. He specializes in advanced 3-D Doppler imaging to detect cancers in numerous organs, including the breast, prostate, and other areas. His images are used to accurately guide biopsies, target therapy and provide focused follow-up after treatment. He is committed to improving non-invasive cancer testing and developing minimally invasive image guided technologies to prevent cancer spread.
Watch VIDEO PART 2: VIDEO: The Advantages of Using Power Doppler Sonography on the Prostate to Screen for Tumors
In the spring of 2020, the Ellis Island Honor Society officially recognized Dr. Bard for his life’s work in clinical and research contributions in diagnostic imaging detection of cancers, which he received in person during a May 2022 ceremony, the prestigious 35th Annual Ellis Island Medal of Honor. Dr. Bard is also an Editorial Advisory Board Member for Imaging Technology News.
Related content:
VIDEO: Using 3-D Doppler Imaging and Other Advancements in Diagnostic Radiology
VIDEO: The Advantages of Using Power Doppler Sonography on the Prostate to Screen for Tumors
One on One ... with Robert L. Bard, MD, PC, DABR, FASLMS
The Full Body Imaging Movement: A Strategic Upgrade of the MRI
Microcirculation and Electromagnetic Response to Inflammation
At RSNA23, Imaging Technology News (ITN) spoke with Bhvita Jani, principal analyst at Signify Research, about advancements and trends in medical imaging, including the development of coronary CTA, use of molecular imaging in theranostic applications, and remote acquisition support, as well as future outlooks and the evolution of medical imaging.
Related content:
VIDEO: Data Workflow and Orchestration in Medical Imaging
VIDEO: One on One with Curtis P. Langlotz, MD, PhD, RSNA President
Find more RSNA23 conference coverage here
In Part 2 of this 3-part video series on recent advancements in diagnostic radiology, current editorial advisory board member Robert L. Bard, MD, PC, DABR, FASLMS, talks with ITN on the advantages of using power Doppler Sonography as a non-invasive way to screen for prostate tumors with abnormal blood vessels.
Dr. Bard is internationally known and recognized as a leader in his field. He specializes in advanced 3-D Doppler imaging to detect cancers in numerous organs, including the breast, prostate, and other areas. His images are used to accurately guide biopsies, target therapy and provide focused follow-up after treatment. He is committed to improving non-invasive cancer testing and developing minimally invasive image guided technologies to prevent cancer spread.
In the spring of 2020, the Ellis Island Honor Society officially recognized Dr. Bard for his life’s work in clinical and research contributions in diagnostic imaging detection of cancers, which he received in person during a May 2022 ceremony, the prestigious 35th Annual Ellis Island Medal of Honor. Dr. Bard is also an Editorial Advisory Board Member for Imaging Technology News.
Related content:
VIDEO: Using 3-D Doppler Imaging and Other Advancements in Diagnostic Radiology
One on One ... with Robert L. Bard, MD, PC, DABR, FASLMS
The Full Body Imaging Movement: A Strategic Upgrade of the MRI
Microcirculation and Electromagnetic Response to Inflammation
Imaging advancements, including 3D Doppler imaging to detect cancers in numerous organs, are used to accurately guide biopsies, target therapy and provide focused follow-up after treatment. ITN spoke with current editorial advisory board member Robert L. Bard, MD, PC, DABR, FASLMS, to find out more about recent advancements in diagnostic radiology. This video is Part 1 of a 3-part video series.
Dr. Bard is internationally known and recognized as a leader in his field. He specializes in advanced 3-D Doppler imaging to detect cancers in numerous organs, including the breast, prostate, and other areas. His images are used to accurately guide biopsies, target therapy and provide focused follow-up after treatment. He is committed to improving non-invasive cancer testing and developing minimally invasive image guided technologies to prevent cancer spread.
In the spring of 2020, the Ellis Island Honor Society officially recognized Dr. Bard for his life’s work in clinical and research contributions in diagnostic imaging detection of cancers, which he received in person during a May 2022 ceremony, the prestigious 35th Annual Ellis Island Medal of Honor. Dr. Bard is also an Editorial Advisory Board Member for Imaging Technology News.
Related content:
One on One ... with Robert L. Bard, MD, PC, DABR, FASLMS
The Full Body Imaging Movement: A Strategic Upgrade of the MRI
Microcirculation and Electromagnetic Response to Inflammation
Radiology Imaging View all 155 items
Find actionable insights to achieve sustainability and savings in radiology in this newest of ITN’s “One on One” video series with Reed A. Omary, MD, MS, Vanderbilt University Medical Center (Nashville, TN). Tune in to "Promoting the Planet's Health: Sustainability in Radiology," to hear from a recognized leader about impactful, cost-saving initiatives radiologists, associations, healthcare systems and vendors can take, and why action is imperative.
Omary, the Carol D. and Henry P. Pendergrass Professor in the VUMC Department of Radiology, is a distinguished radiologist whose commitment to driving healthcare sustainability initiatives has gained both attention and momentum. After serving as Chair of the Department of Radiology and Radiology Sciences from 2012-2023, in June, 2023, Omary stepped away from his role as Chair to pursue a sabbatical focused on climate change and sustainable healthcare. He is author of The Green Leap, a blog about making healthcare sustainable, and founder of the Greenwell Project, a sustainable healthcare non-profit. He has presented a Plenary Lecture at the Radiological Society of North America (RSNA) Annual Scientific Sessions and American College of Radiology (ACR) meetings on the topic, and continues to connect with healthcare systems, vendors and colleagues to advance the issue.
Related content:
PHILIPS MARKS MILESTONE DURING HELIUM-FREE MRI INSTALLATION IN PUERTO RICO
RSNA 2022 PLENARY SPEAKER OMARY URGES RADIOLOGISTS TO SUPPORT PATIENTS, COMMUNITIES AND THE PLANET
RSNA 2022 PANEL DISCUSSIONS FORECAST RADIOLOGY IN 2027, AND HIGHLIGHT WHY MENTORS MATTER
Agfa Radiology Solutions is committed to enhancing clinical outcomes and operational efficiency, underscoring its innovative edge in the dynamically evolving healthcare landscape.
AT RSNA23, ITN met with Karol Wesolowski, Global Commercial Excellence Leader, Agfa Radiology Solutions, and Jeroen Spruyt, Head of BU DR, VP Product Supply and Operations, Agfa Radiology Solutions, to learn more about how the company is transforming radiology practices.
Find more RSNA23 conference coverage here
Related content:
VIDEO: Talking Trends with Agfa — What’s On Tap for RSNA 2023
At RSNA23, Imaging Technology News (ITN) spoke with Bhvita Jani, principal analyst at Signify Research, about advancements and trends in medical imaging, including the development of coronary CTA, use of molecular imaging in theranostic applications, and remote acquisition support, as well as future outlooks and the evolution of medical imaging.
Related content:
VIDEO: Data Workflow and Orchestration in Medical Imaging
VIDEO: One on One with Curtis P. Langlotz, MD, PhD, RSNA President
Find more RSNA23 conference coverage here
Updates on AI in Radiology, RSNA Programs and Stanford Initiatives
Listen and learn with ITN’s newest “One on One” video discussion with a leader in the field of artificial intelligence (AI). RSNA President Curtis P. Langlotz, MD, PhD, Stanford University, offers not-to-be-missed actionable insights into the application and benefits of artificial intelligence in medical imaging. He also shares highlights from RSNA 2023 and top priorities in the coming year, and summarizes the programs on which he and his Stanford University colleagues are focused.
Related content:
Find more RSNA23 conference coverage here
Molecular Imaging View all 19 items
At RSNA23, Imaging Technology News (ITN) spoke with Bhvita Jani, principal analyst at Signify Research, about advancements and trends in medical imaging, including the development of coronary CTA, use of molecular imaging in theranostic applications, and remote acquisition support, as well as future outlooks and the evolution of medical imaging.
Related content:
VIDEO: Data Workflow and Orchestration in Medical Imaging
VIDEO: One on One with Curtis P. Langlotz, MD, PhD, RSNA President
Find more RSNA23 conference coverage here
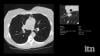
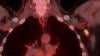
Yael Eshet, M.D., MSc, a diagnostic radiology specialist at Sheba Medical Center in Israel, was the lead author on a recent study that showed COVID-19 (SARS-CoV-2) vaccine adenopathy can persist more than 6 weeks. This swelling of lymph nodes is similar to what is seen cancer and infections and the new findings show it can last longer than 7-10 weeks. The current recommended time people should delay medical imaging is 6 weeks after receiving a COVID vaccine to avoid a misdiagnosis,[2] but this new study shows there is increased inflammation shown on PET-CT imaging for much longer.
These were the findings in the Radiology published study "Prevalence of Increased FDG PET/CT Axillary Lymph Node Uptake Beyond 6 Weeks after mRNA COVID-19 Vaccination."[1]
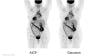
Researchers using fluorodeoxyglucose (FDG)-positron emission tomography (PET) have found increased FDG uptake in the lymph nodes of patients 7-10 weeks past their second mRNA-based Pfizer-BioNTech COVID-19 vaccination. This new information indicates a persistent immune response that could be mistaken on imaging exams for serious conditions like lymphoma over a much longer period of time.
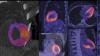
Recent recommendations for post-vaccine lymphadenopathy advise scheduling routine imaging, such as screening mammography, before, or at least 6 weeks after, the final vaccination dose to eliminate false positive results. However, this new research showed that avid axillary lymph node uptake was present beyond 6 weeks after the second vaccination in more than 29% of the patients in the study cohort.
The authors stated “This study shows that avid axillary lymph node uptake on FDG PET/CT can be detected in more than a quarter of our patient population even beyond 6 weeks after the second dose of the mRNA-based COVID-19 vaccination. Compared to a previous study showing normalization of FDG uptake within 40 days of receiving an inactivated H1N1 influenza vaccine, we found uptake persistence even at 70 days. Physicians should be aware of this potential pitfall.”
Some images in this video are from another Radiology study, which showed PET tracer uptake at the COVID vaccine injection site and other examples of axillary adenopathy.[3]
Related COVID Vaccine Axillary Adenapathy Content:
COVID-19 Vaccine Can Cause False Positive Cancer Diagnosis
Help Spread Awareness of Potential COVID-19 Vaccine Imaging Side-effects
VIDEO: COVID Vaccine May Cause Enlarged Lymph Nodes on Mammograms — Interview with Constance "Connie" Lehman, M.D.
COVID-19 Vaccination Axillary Adenopathy Detected During Breast Imaging
PHOTO GALLERY: How COVID-19 Appears on Medical Imaging
CMS Now Requires COVID-19 Vaccinations for Healthcare Workers by January 4
Find more radiology related COVID content
References:
This is an example of Canon's Advanced intelligent Clear-IQ Engine (AiCE) AI-driven image reconstruction software that is now being used to improve image quality on the Canon Celesteion Prime PET/CT nuclear imaging system. The deep learning is used to enhance the iterative reconstruction used to reduce noise and sharped high contrast resolution on positron emission tomography (PET) images from the digital PET detector used on the system.
This example is a whole-body FGD PET scan of a patient with a large BMI with lung cancer.
The Cartesion Prime PET/CT is the industry’s only air-cooled digital PET/CT, provides variable bed time (vBT) acquisition as a standard feature. This and the new FDA 510(k)-pending AiCE technology were highlighted at the 2020 Radiological Society of North America (RSNA) virtual meeting.
Ernest Garcia, Ph.D., MASNC, FAHA, endowed professor in cardiac imaging, director of nuclear cardiology R&D laboratory, Emory University, developer of the Emory Cardiac Tool Box used in nuclear imaging and past-president of the American Society of Nuclear Cardiology (ASNC), explains the use of artificial intelligence (AI) in cardiac imaging. He said there is a tsunami of new AI applications that are starting to flood the FDA for market approval, and there are several examples of AI already in use in radiology. He spoke on this topic in a keynote session at the 2020 ASNC meeting.
Related Artificial Intelligence in Cardiology Content:
VIDEO: Machine Learning for Diagnosis and Risk Prediction in Nuclear Cardiology — Interview with Piotr J. Slomka, Ph.D.,
Artificial Intelligence Applications in Cardiology
VIDEO: Artificial Intelligence May Improve Cath Lab Interventions — Interview with Nick West, M.D., Abbott CMO
How Artificial Intelligence Will Change Medical Imaging
VIDEO: Artificial Intelligence for Echocardiography at Mass General — Interview with Judy Hung, M.D.
VIDEO: ACC Efforts to Advance Evidence-based Implementation of AI in Cardiovascular Care — Interview with John Rumsfeld, M.D.
VIDEO: Overview of Artificial Intelligence and its Use in Cardiology — Interview with Anthony Chang, M.D.
Conference Coverage View all 311 items
Find actionable insights to achieve sustainability and savings in radiology in this newest of ITN’s “One on One” video series with Reed A. Omary, MD, MS, Vanderbilt University Medical Center (Nashville, TN). Tune in to "Promoting the Planet's Health: Sustainability in Radiology," to hear from a recognized leader about impactful, cost-saving initiatives radiologists, associations, healthcare systems and vendors can take, and why action is imperative.
Omary, the Carol D. and Henry P. Pendergrass Professor in the VUMC Department of Radiology, is a distinguished radiologist whose commitment to driving healthcare sustainability initiatives has gained both attention and momentum. After serving as Chair of the Department of Radiology and Radiology Sciences from 2012-2023, in June, 2023, Omary stepped away from his role as Chair to pursue a sabbatical focused on climate change and sustainable healthcare. He is author of The Green Leap, a blog about making healthcare sustainable, and founder of the Greenwell Project, a sustainable healthcare non-profit. He has presented a Plenary Lecture at the Radiological Society of North America (RSNA) Annual Scientific Sessions and American College of Radiology (ACR) meetings on the topic, and continues to connect with healthcare systems, vendors and colleagues to advance the issue.
Related content:
PHILIPS MARKS MILESTONE DURING HELIUM-FREE MRI INSTALLATION IN PUERTO RICO
RSNA 2022 PLENARY SPEAKER OMARY URGES RADIOLOGISTS TO SUPPORT PATIENTS, COMMUNITIES AND THE PLANET
RSNA 2022 PANEL DISCUSSIONS FORECAST RADIOLOGY IN 2027, AND HIGHLIGHT WHY MENTORS MATTER
Industry trade shows and conferences seem to be making their comeback in 2024. And the Healthcare Information and Management Systems Society (HIMSS) Global Conference and Exhibition seems particularly poised to deliver the best of the best when it comes to digital transformation in both the delivery of healthcare, but also the delivery of a quality experience for those in this demanding, rapidly evolving industry. This month in our ongoing One on One series with industry leaders, we are talking with Hal Wolf, FHIMSS, president and CEO of HIMSS. He offered insights on the society’s new partnership with Informa Markets, key topics being covered at HIMSS24, AI’s impact on the industry, and his thoughts on healthcare sustainability.
Find more HIMSS24 conference coverage here
A New Partnership for Growth
Last August, Informa Markets and HIMSS announced a landmark partnership to propel the growth and evolution of the HIMSS Global Health Conference and Exhibition, recognized as the most influential healthcare technology event of the year, and in North America. It draws 40,000 health professionals, tech leaders, providers and governmental organizations from across the globe. Informa Markets, the world’s largest exhibition organizer, took on management of the HIMSS Exhibition, while HIMSS continues to oversee developing expert content and programming.
Exciting New Features at HIMSS24
At HIMSS2024, with this new collaboration comes new features, including:
- A Digital Health Technology Theme Park, filled with innovations that revolve around AI, workforce and the business of healthcare;
- The Government Connections Plaza, featuring the latest rundown from Washington;
- A reimagined Interoperability Showcase for a deeper dive into the inner workings of healthcare;
- Hot topics will be featured on the exhibition Main Stage; and
- A Hosted Buyer Program, facilitating focused meetings between providers and trusted companies in healthcare technology.
Related content:
Find more HIMSS24 conference coverage here
VIDEO: Using Maturity Models to Measure Digital Health
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
Don't miss ITN's latest "One on One" video interview with AAWR Past President and American College of Radiology (ACR) RAN and RADPAC Chair, Amy K. Patel, MD, discussing advocacy initiatives and innovations in artificial intelligence (AI) for breast imaging.
Dr. Patel is a breast imaging trailblazer and radiology advocacy leader. In this video, learn how radiologists can support key initiatives, ways AI is improving patient care, and more.
Related content:
Technology Report: Artificial Intelligence in Radiology 2021
VIDEO: Integrating Artificial Intelligence Into Radiologists Workflow
Tune in to ITN’s latest “One on One” video series with Michael Butkus, PhD, for insights into proton therapy advancements. Butkus is the co-medical director and head of proton physics at the Dwoskin Proton Center at the Sylvester Comprehensive Cancer Center, part of the University of Miami/UHealth Medical System. A board member of the National Association of Proton Therapy (NAPT), Butkus spoke with ITN’s managing editor to discuss how physicists, physicians and vendors are collaborating to expand availability of proton therapy and improve the health of patients being treated.
Related proton therapy content:
Targeting Cancer, Tracking Collaboration: A Progress Report on Proton Therapy
VIDEO: First FLASH Proton Therapy Trial Completed in Humans
Information Technology View all 192 items
Industry trade shows and conferences seem to be making their comeback in 2024. And the Healthcare Information and Management Systems Society (HIMSS) Global Conference and Exhibition seems particularly poised to deliver the best of the best when it comes to digital transformation in both the delivery of healthcare, but also the delivery of a quality experience for those in this demanding, rapidly evolving industry. This month in our ongoing One on One series with industry leaders, we are talking with Hal Wolf, FHIMSS, president and CEO of HIMSS. He offered insights on the society’s new partnership with Informa Markets, key topics being covered at HIMSS24, AI’s impact on the industry, and his thoughts on healthcare sustainability.
Find more HIMSS24 conference coverage here
A New Partnership for Growth
Last August, Informa Markets and HIMSS announced a landmark partnership to propel the growth and evolution of the HIMSS Global Health Conference and Exhibition, recognized as the most influential healthcare technology event of the year, and in North America. It draws 40,000 health professionals, tech leaders, providers and governmental organizations from across the globe. Informa Markets, the world’s largest exhibition organizer, took on management of the HIMSS Exhibition, while HIMSS continues to oversee developing expert content and programming.
Exciting New Features at HIMSS24
At HIMSS2024, with this new collaboration comes new features, including:
- A Digital Health Technology Theme Park, filled with innovations that revolve around AI, workforce and the business of healthcare;
- The Government Connections Plaza, featuring the latest rundown from Washington;
- A reimagined Interoperability Showcase for a deeper dive into the inner workings of healthcare;
- Hot topics will be featured on the exhibition Main Stage; and
- A Hosted Buyer Program, facilitating focused meetings between providers and trusted companies in healthcare technology.
Related content:
Find more HIMSS24 conference coverage here
VIDEO: Using Maturity Models to Measure Digital Health
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
Clinicians and referring physicians need fast, secure access to both patient data and their diagnostic or viewing tool set. But the cost barriers and the complexity of owning and maintaining healthcare information systems can compromise the quality of care.
To address this, Philips has partnered with AWS to develop Philips HealthSuite Imaging — a new radiology cloud service that provides on-demand access to advanced medical imaging software.
ITN recently visited with Madhuri Sebastian and Matthieu Ferrant to learn more about this service.
A discussion on processing, and then understanding, how to implement data workflow and orchestration in medical imaging with Jef Williams, managing partner, Paragon Health IT, and Imaging Technology News (ITN) editorial advisory board member.
Related content:
VIDEO: One on One with Curtis P. Langlotz, MD, PhD, RSNA President
Find more RSNA23 conference coverage here
Fujifilm recently expanded its enterprise imaging portfolio with Synapse Pathology, the company’s newly acquired and branded digital pathology PACS solution.
Synapse Pathology is an open, vendor-agnostic, end-to-end solution designed for medical facilities that handle large volumes of pathology images and data across multiple locations.
Imaging Technology News recently met with Fujifilm’s Bill Lacy and Mark Lloyd, and Chuck Barkey at West Virginia University Medicine to learn more about this new addition to the Synapse Enterprise Imaging portfolio.
Related content:
Rural Hospital Raises the Bar with Comprehensive State-of-the-art Imaging Systems
Fujifilm’s Synapse Pathology Wins 2023 MedTech Breakthrough Award
Develop, Partner, Acquire or Avoid: Where is Investment for Digital Pathology Headed?
Women's Health View all 79 items
Don't miss ITN's latest "One on One" video interview with AAWR Past President and American College of Radiology (ACR) RAN and RADPAC Chair, Amy K. Patel, MD, discussing advocacy initiatives and innovations in artificial intelligence (AI) for breast imaging.
Dr. Patel is a breast imaging trailblazer and radiology advocacy leader. In this video, learn how radiologists can support key initiatives, ways AI is improving patient care, and more.
Related content:
Technology Report: Artificial Intelligence in Radiology 2021
VIDEO: Integrating Artificial Intelligence Into Radiologists Workflow
In addition to women with dense breasts, there are also other women for whom mammographic screening is not really enough, which is why research needs to continue in this field. Dr. Wendie Berg, a leading breast cancer specialist, talks with ITN about new research and advancements in breast imaging technology.
Dr. Berg, MD, PhD, FACR, FSBI, is Professor of Radiology at the University of Pittsburgh School of Medicine and Magee-Womens Hospital of UPMC, specializing in breast imaging. She is also the Chief Scientific Advisor to DenseBreast-info.org. A renowned expert, she writes and co-edits one of the leading textbooks on the topic, Diagnostic Imaging: Breast, currently in its third edition, and has co-authored over 120 peer-reviewed research publications.
Related Breast Density Content:
VIDEO: FDA Update on the US National Density Reporting Standard - A Discussion on the Final Rule
One on One … with Wendie Berg, MD, PhD, FACR, FSBI
Task Force Issues New Draft Recommendation Statement on Screening for Breast Cancer
Creating Patient Equity: A Breast Density Legislative Update
AI Provides Accurate Breast Density Classification
VIDEO: The Impact of Breast Density Technology and Legislation
VIDEO: Personalized Breast Screening and Breast Density
VIDEO: Breast Cancer Awareness - Highlights of the NCoBC 2016 Conference
Fake News: Having Dense Breast Tissue is No Big Deal
The Manic World of Social Media and Breast Cancer: Gratitude and Grief
Related Breast Imaging Content:
Single vs. Multiple Architectural Distortion on Digital Breast Tomosynthesis
Today's Mammography Advancements
Digital Breast Tomosynthesis Spot Compression Clarifies Ambiguous Findings
AI DBT Impact on Mammography Post-breast Therapy
ImageCare Centers Unveils PINK Better Mammo Service Featuring Profound AI
Radiologist Fatigue, Experience Affect Breast Imaging Call Backs
Fewer Breast Cancer Cases Between Screening Rounds with 3-D Mammography
Study Finds Racial Disparities in Access to New Mammography Technology
It has long been said that a national reporting standard is needed in order to ensure all American women receive at least the same basic information regarding breast density, and a spotlight put on the importance of routine breast imaging. Dr. Wendie Berg, a leading breast cancer specialist, shares with ITN what is being done in the fight against breast cancer and the importance of this standardization in reporting for women.
Dr. Berg, MD, PhD, FACR, FSBI, is Professor of Radiology at the University of Pittsburgh School of Medicine and Magee-Womens Hospital of UPMC, specializing in breast imaging. She is also the Chief Scientific Advisor to DenseBreast-info.org. A renowned expert, she writes and co-edits one of the leading textbooks on the topic, Diagnostic Imaging: Breast, currently in its third edition, and has co-authored over 120 peer-reviewed research publications.
Related Breast Density Content:
VIDEO: Research and Advancements in Breast Imaging Technology
One on One … with Wendie Berg, MD, PhD, FACR, FSBI
Task Force Issues New Draft Recommendation Statement on Screening for Breast Cancer
Creating Patient Equity: A Breast Density Legislative Update
AI Provides Accurate Breast Density Classification
VIDEO: The Impact of Breast Density Technology and Legislation
VIDEO: Personalized Breast Screening and Breast Density
VIDEO: Breast Cancer Awareness - Highlights of the NCoBC 2016 Conference
Fake News: Having Dense Breast Tissue is No Big Deal
The Manic World of Social Media and Breast Cancer: Gratitude and Grief
Related Breast Imaging Content:
Single vs. Multiple Architectural Distortion on Digital Breast Tomosynthesis
Today's Mammography Advancements
Digital Breast Tomosynthesis Spot Compression Clarifies Ambiguous Findings
AI DBT Impact on Mammography Post-breast Therapy
ImageCare Centers Unveils PINK Better Mammo Service Featuring Profound AI
Radiologist Fatigue, Experience Affect Breast Imaging Call Backs
Fewer Breast Cancer Cases Between Screening Rounds with 3-D Mammography
Study Finds Racial Disparities in Access to New Mammography Technology
Dr. Frank A. Vicini, MD, FACR, FASTRO, FABS, who is a radiation oncologist with GenesisCare, discussed his findings from a phase III trial presented at ASTRO22 that evaluated new and improved techniques to treat patients with breast cancer. Here he shares some of his findings with Imaging Technology News (ITN).
Related Conference Coverage:
Photo Gallery of Technologies Showcased at ASTRO 2022
ASTRO 2022 Shines Spotlight on “Cancer Breakthroughs” with AAPM, ASCO Research
“Cancer Breakthroughs” Session at ASTRO2022 Unveils Key Findings from ASCO, AAPM
Looking Ahead to ASTRO: Keynotes, Awards and Scientific Session Updates