Find actionable insights to achieve sustainability and savings in radiology in this newest of ITN’s “One on One” video series with Reed A. Omary, MD, MS, Vanderbilt University Medical Center (Nashville, TN). Tune in to "Promoting the Planet's Health: Sustainability in Radiology," to hear from a recognized leader about impactful, cost-saving initiatives radiologists, associations, healthcare systems and vendors can take, and why action is imperative.
Omary, the Carol D. and Henry P. Pendergrass Professor in the VUMC Department of Radiology, is a distinguished radiologist whose commitment to driving healthcare sustainability initiatives has gained both attention and momentum. After serving as Chair of the Department of Radiology and Radiology Sciences from 2012-2023, in June, 2023, Omary stepped away from his role as Chair to pursue a sabbatical focused on climate change and sustainable healthcare. He is author of The Green Leap, a blog about making healthcare sustainable, and founder of the Greenwell Project, a sustainable healthcare non-profit. He has presented a Plenary Lecture at the Radiological Society of North America (RSNA) Annual Scientific Sessions and American College of Radiology (ACR) meetings on the topic, and continues to connect with healthcare systems, vendors and colleagues to advance the issue.
Related content:
PHILIPS MARKS MILESTONE DURING HELIUM-FREE MRI INSTALLATION IN PUERTO RICO
RSNA 2022 PLENARY SPEAKER OMARY URGES RADIOLOGISTS TO SUPPORT PATIENTS, COMMUNITIES AND THE PLANET
RSNA 2022 PANEL DISCUSSIONS FORECAST RADIOLOGY IN 2027, AND HIGHLIGHT WHY MENTORS MATTER































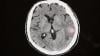
 The software also offers a second set of eyes for more difficult to detect cases. Quickly determining is a stroke is ischemic or hemorrhagic is critical to the path of treatment. If caught early enough, TPA can be injected into patients to clear clots causing an ischemic stroke, but can cause massive brain damage or death if injected into a patient with a brain bleed. At advanced neuro-interventional centers, quickly determining the type of stroke is needed to know if they need to revascularize a patient or manage a hemorrhage.
The software also offers a second set of eyes for more difficult to detect cases. Quickly determining is a stroke is ischemic or hemorrhagic is critical to the path of treatment. If caught early enough, TPA can be injected into patients to clear clots causing an ischemic stroke, but can cause massive brain damage or death if injected into a patient with a brain bleed. At advanced neuro-interventional centers, quickly determining the type of stroke is needed to know if they need to revascularize a patient or manage a hemorrhage. 