July 25, 2025 — Data in recent staffing surveys from the American Society of Radiologic Technologists show that vacancy rates for all medical imaging disciplines are above the rates reported in 2020, according to the 2025 ASRT Radiologic Sciences Staffing and Workplace Survey.
Coronavirus (COVID-19)
This page contains medical information for clinicians on the 2019 Novel Coronavirus (COVID-19, also called 2019-nCoV and now clinically SARS‐CoV‐2). This section includes articles on medical imaging of the virus for radiologists, new technologies being deployed to fight the virus and clinical information from various sources. Here are direct links for medical professionals to COVID-19 resources from the U.S. Food and Drug Administration (FDA), Centers for Disease Control (CDC) and the World Health Organization (WHO). Daily world-wide statistics on the coronavirus outbreak are available from the WHO Situations Reports. Centers for Medicare and Medicaid Services (CMS) frequently asked questions and answers (FAQs) for healthcare providers regarding Medicare payment for laboratory tests and other services related to the COVID-19
July 25, 2025 — Data in recent staffing surveys from the American Society of Radiologic Technologists show that vacancy ...
Postpandemic staffing shortages and increased volumes require radiologists to do more with less, exacerbating burnout ...
June 11, 2024 — A new study led by researchers at Emory AI.Health, published in the Journal of Computers in Medicine and ...
Members of the enterprise imaging technology community are facing significant changes in the market, due to the COVID-19 ...
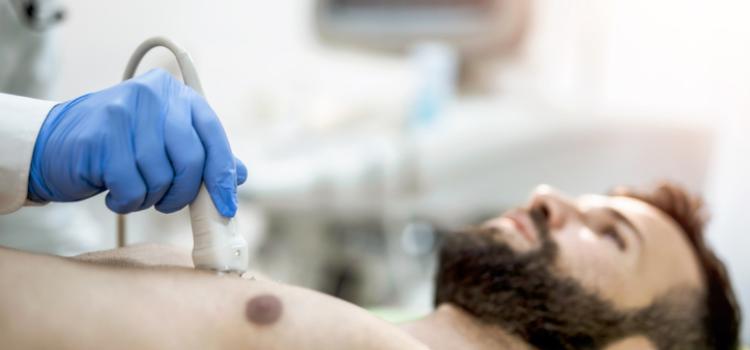
March 21, 2024 — Artificial intelligence can spot COVID-19 in lung ultrasound images much like facial recognition ...
March 20, 2024 — SARS-CoV-2, the virus that causes COVID-19, can damage the heart even without directly infecting the ...
November 22, 2023 — People with long COVID exhibit patterns of changes in the brain that are different from fully ...
The COVID-19 pandemic accelerated a change that was already occurring in imaging-heavy practices across the country — ...
November 20, 2023 — Using an image-guided minimally invasive procedure, researchers may be able to restore the sense of ...
September 21, 2023 — Declines in cardiovascular procedure volumes observed early in the COVID-19 pandemic greatly ...
September 18, 2023 — The Society of Nuclear Medicine and Molecular Imaging (SNMMI), as a professional society ...
The coronavirus pandemic has changed the way radiologists read images and today facilities struggle to define a “new ...
August 18, 2023 — Artificial intelligence (AI) is capturing the public imagination as the pace of innovation accelerates ...
Healthcare is constantly evolving, finding new ways to innovate and advance digital tools and technology. With this ...
July 3, 2023 — According to an accepted manuscript published in ARRS’ own American Journal of Roentgenology (AJR) ...
June 14, 2023 — A University of Waterloo engineer’s MRI invention reveals better than many existing imaging technologies ...
May 17, 2023 — According to an accepted manuscript published in ARRS’ own American Journal of Roentgenology (AJR), SARS ...
May 9, 2023 — The American College of Radiology (ACR) Economics and Health Policy Department has selected Ezequiel Silva ...
March 13, 2023 — According to an accepted manuscript published in ARRS’ American Journal of Roentgenology (AJR) ...
March 13, 2023 — The American College of Radiology (ACR) and the American College of Emergency Physicians (ACEP) ...
March 10, 2023 — Researchers found evidence of heart muscle inflammation in a small number of patients with acute ...
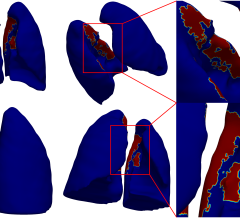
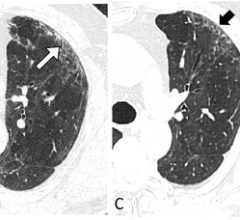
February 15, 2023 — Chest CT revealed persistent lung abnormalities in patients two years after COVID-19, according to a ...
February 8, 2023 — New data published in the Journal of Clinical Oncology further quantify the vast lingering impact of ...





 July 25, 2025
July 25, 2025