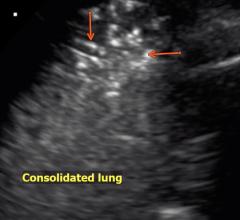
An example of COVID-19 (SARS-CoV-2) pneumonia lung consolidation on ultrasound. Related COVID ultrasound video clips ...
Coronavirus (COVID-19)
This page contains medical information for clinicians on the 2019 Novel Coronavirus (COVID-19, also called 2019-nCoV and now clinically SARS‐CoV‐2). This section includes articles on medical imaging of the virus for radiologists, new technologies being deployed to fight the virus and clinical information from various sources. Here are direct links for medical professionals to COVID-19 resources from the U.S. Food and Drug Administration (FDA), Centers for Disease Control (CDC) and the World Health Organization (WHO). Daily world-wide statistics on the coronavirus outbreak are available from the WHO Situations Reports. Centers for Medicare and Medicaid Services (CMS) frequently asked questions and answers (FAQs) for healthcare providers regarding Medicare payment for laboratory tests and other services related to the COVID-19
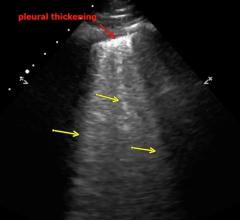
An example of lung pleural thickening formation caused by COVID-19 (SARS-CoV-2). Related COVID ultrasound video clips ...
October 20, 2021 — On behalf of the nation's radiation oncologists and the more than one million people with cancer they ...
Members of the enterprise imaging technology community are facing significant changes in the market, due to the COVID-19 ...
October 20, 2021 — New research in the October 2021 issue of JNCCN—Journal of the National Comprehensive Cancer Network ...
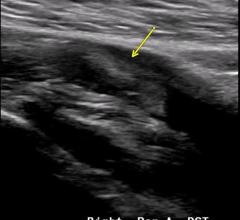
An example of popliteal artery thrombosis formation caused by COVID-19 (SARS-CoV-2). Coronavirus often caused thrombus ...
September 28, 2021 — The global radiotherapy devices market is expected to grow from $5.44 billion in 2020 to $5.848 ...
The COVID-19 pandemic accelerated a change that was already occurring in imaging-heavy practices across the country — ...
September 27, 2021 — GE Healthcare unveiled Revolution Ascend with Effortless Workflow, offering clinicians a collection ...
A year after COVID-19 turned the world upside down, the American Society of Nuclear Cardiology (ASNC) asked members how ...
The breast ultrasound market is seeing growth, driven largely by the proliferation of recent legislation aimed at ...
The coronavirus pandemic has changed the way radiologists read images and today facilities struggle to define a “new ...
According to a new report produced by Grand View Research, the global magnetic resonance imaging (MRI) market size was ...
September 13, 2021 — At the opening press conference of the ESMO Congress 2021, President Solange Peters announced that ...
September 13, 2021 — The Radiological Society of North America (RSNA) today announced highlights of the Technical ...
September 9, 2021 — According to ARRS’ American Journal of Roentgenology (AJR), immediately reading screening mammograms ...
The in-person 2021 Healthcare Information Management Systems Society (HIMSS) meeting planned for Aug. 9-13 appeared to ...
September 3, 2021 — Researchers at Case Western Reserve University have developed an online tool to help medical staff ...
Several radiology IT vendors at 2021 Healthcare Information Management Systems Society (HIMSS) conference demonstrated ...
August 24, 2021 — Telehealth came into its own during the COVID-19 pandemic, providing patients access to care in the ...
August 23, 2021 — The U.S. Food and Drug Administration (FDA) just granted full approval to the Pfizer/BioNTech COVID-19 ...
August 19, 2021 — In a new publication from Cardiovascular Innovations and Applications; DOI, Zhaowei Zhu, Jianjun Tang ...
August 12, 2021 — RSNA 2021 will require proof of COVID-19 vaccination from all in-person attendees and exhibitors at ...

 October 22, 2021
October 22, 2021