The Software & Information Industry Association (SIIA) announced its finalists for the 68th Jesse H. Neal Awards — the ...
Coronavirus (COVID-19)
This page contains medical information for clinicians on the 2019 Novel Coronavirus (COVID-19, also called 2019-nCoV and now clinically SARS‐CoV‐2). This section includes articles on medical imaging of the virus for radiologists, new technologies being deployed to fight the virus and clinical information from various sources. Here are direct links for medical professionals to COVID-19 resources from the U.S. Food and Drug Administration (FDA), Centers for Disease Control (CDC) and the World Health Organization (WHO). Daily world-wide statistics on the coronavirus outbreak are available from the WHO Situations Reports. Centers for Medicare and Medicaid Services (CMS) frequently asked questions and answers (FAQs) for healthcare providers regarding Medicare payment for laboratory tests and other services related to the COVID-19
Imaging Technology News (ITN) has been named a finalist from the American Society of Business Publication Editors (ASBPE ...
March 7, 2022 — The "Global CT Equipment Procedure Volumes and Reimbursement Growth Opportunities" report has been added ...
Members of the enterprise imaging technology community are facing significant changes in the market, due to the COVID-19 ...
Here is what you and your colleagues found to be most interesting in the field of medical imaging during the month of ...
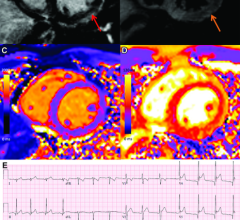
February 17, 2022 — While cardiac imaging shows that COVID-19 vaccine–associated myocarditis has a similar pattern as ...
February 16, 2022 — The COVID-19 pandemic upended many aspects of daily life, particularly in the first months and year ...
The COVID-19 pandemic accelerated a change that was already occurring in imaging-heavy practices across the country — ...
February 15, 2022 — Vaccine-associated myocarditis shows a similar injury pattern on cardiac MRI compared to other ...
February 14, 2022 — Cancer patients undergoing active treatment were more likely to believe misinformation related to ...
February 8, 2022 — There should be no delay in screening mammograms after COVID-19 vaccination due to a swelling in the ...
The coronavirus pandemic has changed the way radiologists read images and today facilities struggle to define a “new ...
Here is a list of the Top 10 most read pieces of content on ITNonline.com from the month of January 2022. This is based ...
February 2, 2022 — Urgent and immediate action must be taken to ensure more effective and equitable implementation of ...
Marc Succi, M.D., an emergency radiologist at MGH and executive director of the MESH Incubator, an in-house innovation ...
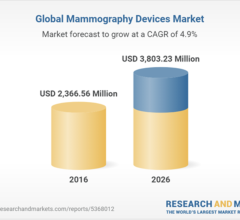
January 31, 2022 — The Global Mammography Devices Market stood at USD 2744.07 million in 2020 and is expected to grow at ...
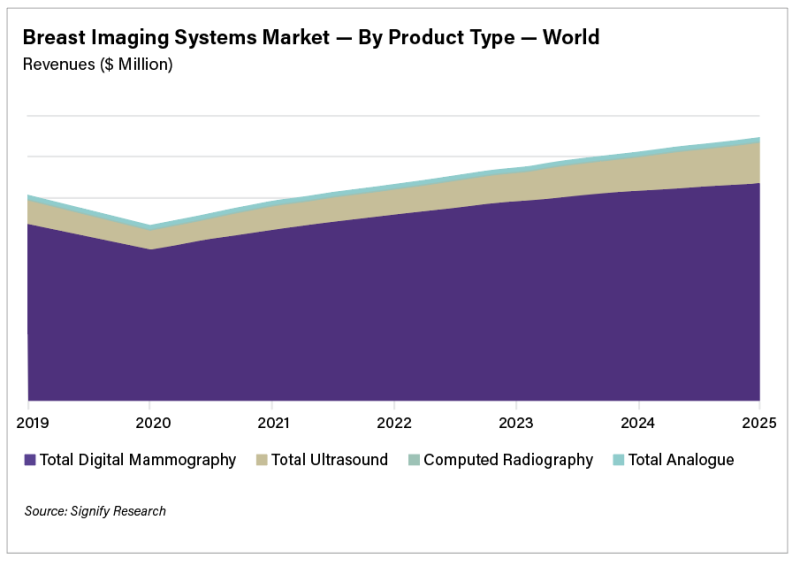
Since the advent of ultrasound scanning in the 1950s, the global movement to develop and expand its diagnostic features ...
The rising global incidence rates of breast cancer, coupled with the severe backlog of women requiring breast cancer ...
January 20, 2022 — Leading health tech firm Qure.ai has gained 510(k) clearance from the Food and Drug Administration ...
The Great Resignation has impacted every industry, including ours. While this movement will be studied for years to come ...
A 26-year-old man with history of diabetes and hypertension presented with 7 days of fever, chills, nausea, intractable ...
January 18, 2022 — In a statement released today from the Association for Medical Imaging Management (AHRA), the ...
January 17, 2022 — The COVID-19 pandemic has fundamentally changed the health care delivery landscape and shifted the ...


 March 10, 2022
March 10, 2022