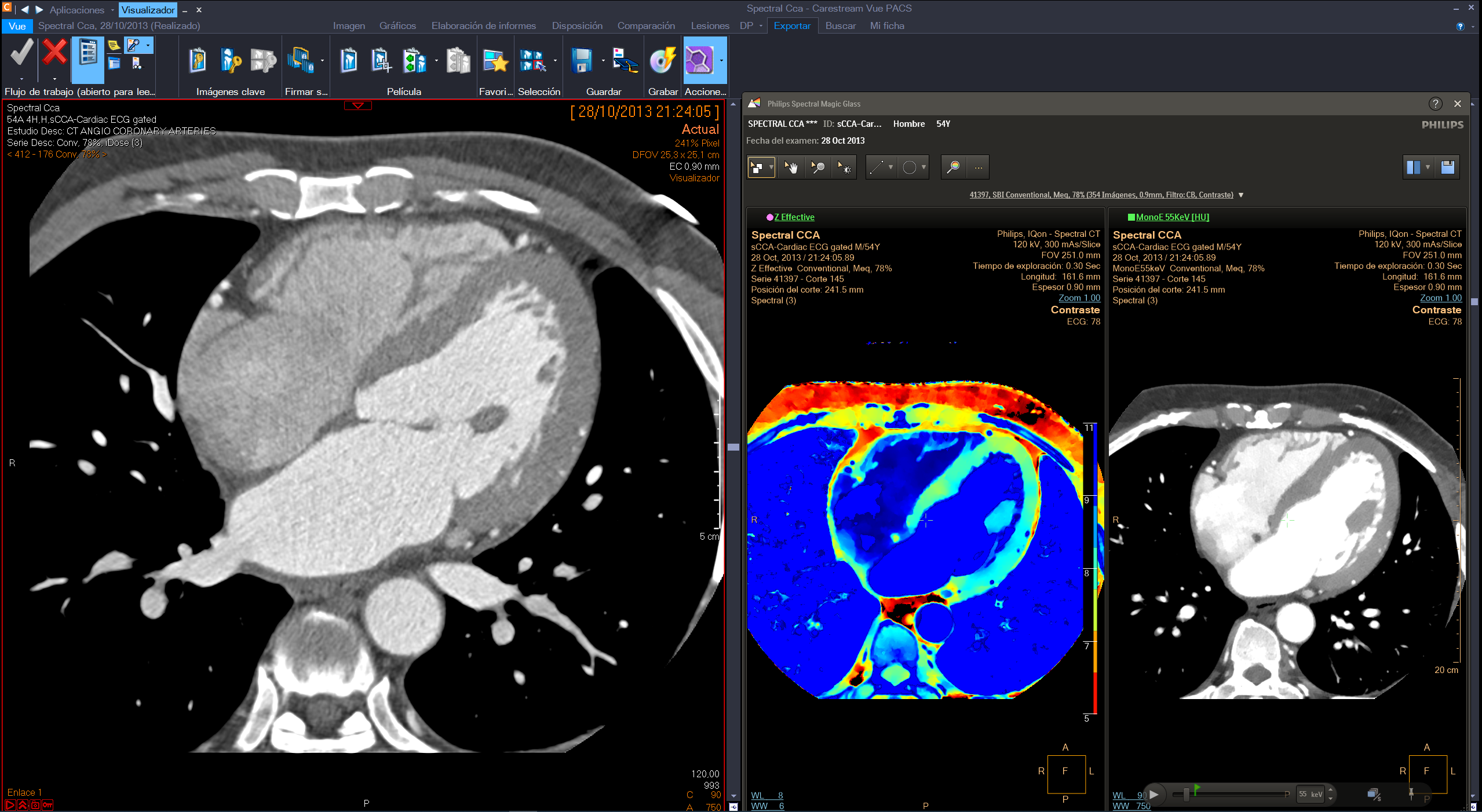
Philips integrated the IntelliSpace Portal advanced applications with the Philips diagnostic viewer (from Carestream) creating a combined radiology diagnostic workspace.
Radiology enterprise imaging platforms and picture archiving and communication systems (PACS) have recently evolved in several ways to help improve workflows. To name a few, streamlined integration of data from various departments into the electronic medical record (EMR) to share images, and the addition of artificial intelligence to increase efficiencies.
The evolution of PACS has gone from the integration of separate radiology information systems (RIS) and PACS into one system. This evolution over the past decade has been a trend at large hospitals and healthcare systems from siloed PACS to enterprise imaging systems, enabling a few image-heavy departments, or all departments across the enterprise, to integrate their data and images into one central, vendor neutral location. This makes integration of patient data from numerous sources easier to integrate into the over-arching EMR systems.
Many vendors today are touting enterprise imaging. These systems will likely become the way of the future to enable additional integration of digital health records in one location. However, there is still a robust standalone PACS market for smaller hospitals and clinics.
Here are several key takeaways from the Radiological Society of North America’s (RSNA) 2020 annual meeting. Many of these points are not new, they are just a continuation of the evolution of this technology.
1. Radiology Workflow Orchestration
The buzzword “workflow orchestration” is being used by some vendors to describe their systems’ ability to use smart workflows to optimize radiology reading lists.
Carestream’s artificial intelligence (AI)-driven workflow orchestrator was the key IT asset desired by Philips Healthcare when it bought Carestream’s IT division in 2019. By RSNA 2020, Philips had incorporated that technology into its systems. Sectra also touted workflow orchestration at RSNA as being a key to improving radiology workflow.
Orchestration creates order on reading lists where specific exams will be routed to the most qualified radiologist, and it eliminates radiologists cherry-picking the exams they want to review by having the system limit their selections to what actually needs to be read. These systems further prioritize reads and the position on studies in the list based on STAT reads, exam protocol type, and on how long they have been available and are approaching the deadline for reads based on service level agreements (SLAs).
Orchestration can manage distributed workflows so the workload is shared equitably between radiologists and different sites. The systems also can monitor, manage and analyze radiology workloads to help identify bottlenecks, issues with some types of exams, and offer analytics on the radiologists, technologists, exam protocols, facilities and the ability to meet SLA parameters.
2. AI Integration into PACS and Enterprise Imaging Platforms
AI has by far been the biggest and most exciting trend in radiology IT systems over the past few years. The discussion at RSNA 2020 has moved away from explaining how AI works, to a general acceptance. If an AI application has regulatory clearance, the main question is how will it help radiologists or hospitals improve their workflow and patient care.
Most of the AI algorithms are being integrated into the backend of PACS or enterprise imaging systems as workflow aids that operate unnoticed. Algorithms developed by Agfa, Philips and Siemens can identify the imaging protocol used and automatically pull in prior exams and patient history that are relevant to the organ or section of the body being imaged.
The Philips diagnostic workspace anticipates the radiologist’s next move to speed workflow. In the case of serial computed tomography (CT) scans of cancer patients to track tumor size during treatments, the system can automatically call up prior exams for comparisons. It also automates finding the exact same view the radiologist has chosen, and standardizes and automates the tumor quantification processes to show if the tumor is shrinking or getting larger.
Siemens Healthineers has developed two AI-supported platforms. AI-Rad Companion helps reduce basic repetitive tasks and can increase diagnostic precision when interpreting medical images. It provides automatic post-processing of image datasets through AI-powered algorithms. The automation of routine workflows in areas of high case volumes helps the radiologist gain back more time to focus on more critical or involved exams.
Siemens’ AI-Pathway Companion optimizes personalized patient care by using AI-guided care pathways. The intelligent decision support system can offer suggestions for facilitating diagnosis and therapeutic decisions along disease-specific pathways. The suggested courses of action are based on evidence-based guidelines. This can be particularly helpful for multidisciplinary tumor boards. The patient’s “pathway” through the health system is illustrated with a timeline showing where a patient is at on the pathway, and links to prior exams and reports.
Another aspect of AI is diagnostic support. AI algorithms can work in the background to automatically identify regions of interest on images, including FDA-cleared applications to identify pneumothorax, improper placement of endotracheal tubes, if a patient has a stroke and whether it is ischemic or hemorrhagic, the presence of tumors, or to red flag incidental findings that are outside the main area of the exam’s protocol.
Many PACS/enterprise imaging vendors are working on their own AI apps and are partnering with third-party AI vendors to offer a wide variety of AI solutions.
3. Radiology Workflow Automation
AI is also being baked into systems to automatically identify anatomy, key image views for reads, set-up of specific radiologists’ hanging protocols, and to automatically make key measurements. AI is also being used to autofill sections of radiology reports with measurements or common paragraphs of text based on findings of what the AI sees or measures in the images. All of these measures help speed workflow and often act as a second set of eyes for the radiologist. The radiologist still maintains control in being able to override and edit anything the artificial intelligence has added.
4. Image Remote Views Help Radiologists Collaborate
Remote viewing systems are increasing in popularity, but their importance has been further propelled by the COVID-19 pandemic. Many radiologists have worked remote when possible, and efforts were made at most hospitals to limit contact between staff. Remote image sharing/viewing systems allow radiologists to send images to referring physicians or to collaborate with peers.
A recent movement in radiology platforms is to allow live, remote collaboration. This can allow discussion on what a surgeon needs from the radiologist while preparing for a procedure, with other radiologists for odd image findings, or for multidisciplinary care team meetings. Some remote viewing systems also enable sharing links to radiologists or doctors outside the hospital, so they can take a quick look at imaging on mobile devices.
An example of this is the Visage 7 Live Connect platform, where radiologists can immediately and securely collaborate and share images with referrers directly from Visage 7 during interpretation workflow. The radiologist sends a secure link and session code to all intended recipients for real-time viewing from any web browser. It does not require recipient users to have any installed software or account.
5. Web-based Radiology Systems
Over the past few years, most PACS and all enterprise imaging systems have migrated to cloud-based solutions. This enables any web-enabled computer to become a PACS workstation, which greatly simplifies user access. Rather than needing to cable connect dedicated PACS workstations across a hospital or enterprise, house and maintain massive servers and require all updates to be done manually on each computer, all users need is internet connection.
This outsourced IT architecture enables software updates to be done in the cloud, rather than individual computers. Data storage is now often accomplished using remote cloud servers. This allows hospitals to get out of the business of maintaining large server rooms.
The technology also allows easier integration of remote viewing systems and the ability to access information and images on mobile devices.
Related Enterprise Imaging Content:
Radiology Technology Trends to Watch in 2020
PACS and the Road to Reconstruction
The First Step in Building an Enterprise Initiative
BLOG: Artificial Intelligence May Help Enterprise Imaging
BLOG: How AI Might Boost Efficiency and Effectiveness
BLOG: How AI Could Make Radiologists’ Jobs Less Stressful
BLOG: How Burnout Puts Radiology at Risk
Centricity Universal Viewer: Embrace the Power of One Intelligent Diagnostic Viewer


 May 14, 2026
May 14, 2026 









