March 29, 2023 — In a partnership which aims to provide faster and safer medical imaging across Australia and New ...
PET Imaging
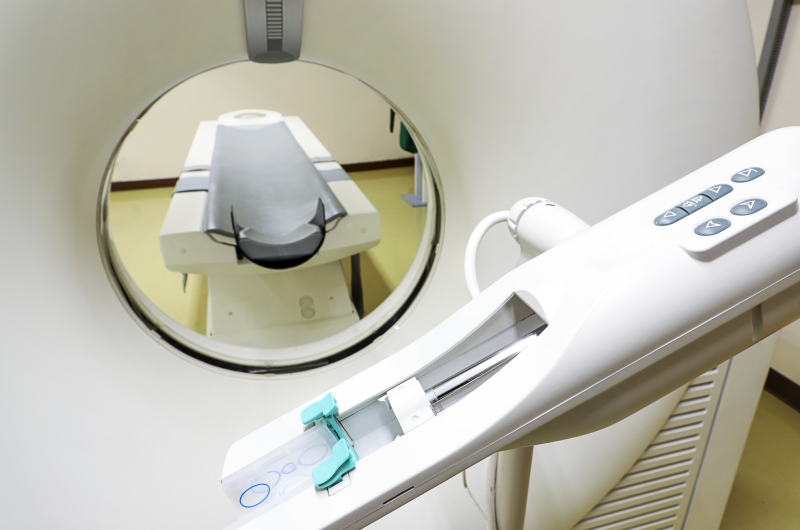
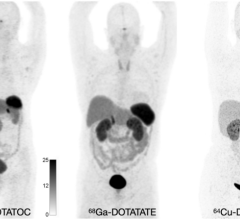
Positron emission tomography (PET) is a nuclear imaging technology (also referred to as molecular imaging) that enables visualization of metabolic processes in the body. The basics of PET imaging is that the technique detects pairs of gamma rays emitted indirectly by a positron-emitting radionuclide (also called radiopharmaceuticals, radionuclides or radiotracer). The tracer is injected into a vein on a biologically active molecule, usually a sugar that is used for cellular energy. PET systems have sensitive detector panels to capture gamma ray emissions from inside the body and use software to plot to triangulate the source of the emissions, creating 3-D computed tomography images of the tracer concentrations within the body.
March 23, 2023 — Nuclidium announced that the Neuroendocrine Tumors Research Foundation (NETRF) has selected the company ...
March 21, 2023 — Positron Corporation, a molecular imaging device company that offers PET imaging systems and clinical ...
Digital technology is opening remarkable opportunities for clinical positron emission tomography (PET) about which ...
March 10, 2023 — Researchers found evidence of heart muscle inflammation in a small number of patients with acute ...
February 23, 2023 — The Society of Nuclear Medicine and Molecular Imaging (SNMMI) and the European Association of ...
February 9, 2023 — Blue Earth Diagnostics, a Bracco company and recognized leader in the development and ...
Precision can have an enormous impact on patients. From diagnosis to patient monitoring (see “How Digital PET/CT Can ...
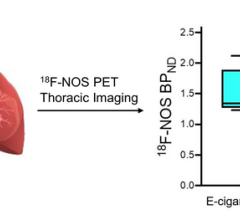
January 31, 2023 — Electronic cigarette (e-cigarette) users have greater lung inflammation than cigarette smokers and ...
December 14, 2022 — CytoSite Bio, a company developing precision imaging products that determine patient response to ...
December 2, 2022 — Blue Earth Diagnostics, a Bracco company and recognized leader in the development and ...
PET is getting ready to venture outside oncology, cardiology and mainstream neurology. High on the list of new clinical ...
December 1, 2022 — A new method for determining whether patients with heart disease need coronary stents or bypass ...
November 2, 2022 — Blue Earth Diagnostics, a Bracco company and recognized leader in the development and ...
According to a recent study from market research firm Graphical Research, the global imaging agents market size is set ...
Analog is approximate. Digital is specific. Therein lies the fundamental difference between digital PET and its analog ...
October 25, 2022 — Blue Earth Diagnostics, a Bracco company and recognized leader in the development and ...
October 24, 2022 — RefleXion Medical, a therapeutic oncology company pioneering biology-guided radiotherapy* (BgRT) as a ...
October 20, 2022 — A new highly selective PET imaging agent can detect the presence of overexpressed monoamine oxidase-B ...
October 19, 2022 — Blue Earth Diagnostics, a Bracco company and recognized leader in the development and ...
September 28, 2022 — Blue Earth Diagnostics, a Bracco company and recognized leader in the development and ...
September 28, 2022 — Xoran Technologies is engaged in a ground-breaking research project to develop a PET/CT scanner for ...
September 13, 2022 — For over 40 years the vision of Shared Medical Services (SMS) has been to provide innovative ...
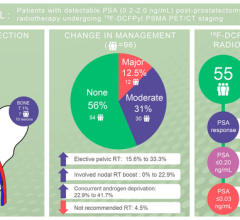
September 8, 2022 — In prostate cancer patients experiencing recurrence following a radical prostatectomy, imaging with ...


 March 29, 2023
March 29, 2023 





![data showed that CytoSite’s Granzyme B (GzmB) PET imaging using [68Ga-NOTA]-hGZP (CSB-111) was feasible and safe in human subjects. These data come from a Phase I trial assessing the safety and feasibility of GzmB PET imaging in subjects with melanoma and non-small cell lung cancer (NSCLC) receiving KEYTRUDA (pembrolizumab).](/sites/default/files/styles/feed_medium/public/Cytosite.png?itok=ZBUOmEkJ)