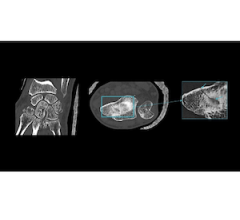
GE Healthcare showcases Senographe Pristina Serena featuring its add-on-biopsy kit at the Breast Imaging Symposium. Photo by Greg Freiherr
Productivity and its enabler — efficiency — guided the display of products at the April Society of Breast Imaging (SBI)/American College of Radiology (ACR) 2019 Breast Imaging Symposium. But if the undercurrent of productivity is to take hold, the patient must benefit in the coming marketplace of value-based medicine.
Products shown on the exhibit floor indicated what different vendors perceive as opportunities. GE Healthcare demonstrated the flexibility achieved with its Senographe Pristina 3-D mammography system, ranging from screening to diagnosis; Siemens Healthineers focused on the advantages possible with the use of wide-angle digital breast tomosynthesis. Fujifilm Medical Systems USA showcased new software that uses data obtained during tomosynthesis; Konica Minolta Healthcare Americas focused on software to improve communications among care providers; and Barco Healthcare showed a high-performance monitor with the luminescence to be used in X-ray mammography but flexible enough to be used across all modalities.
Different approaches were showcased for identifying tissue to be surgically excised following the diagnosis of breast cancer. Developers of medical artificial intelligence (AI) described how their smart algorithms might improve care, with several describing near-term objectives; others long-term, including risk stratification; some both.
Commercial efforts to develop AI in women’s health have tended to focus on building smart algorithms that accelerate currently accepted medical practices, boosting efficiency and effectiveness. Profound AI from iCAD exemplifies how the current development of AI can affect breast imaging. This software, which was cleared by the U.S. Food and Drug Administration (FDA) in late 2018, helps physicians interpret digital breast tomosynthesis images. Its use aligns well with the goals of value-based medicine, which emphasizes increased efficiency and effectiveness while offering patient benefits such as reduced false positive rates and improved patient recall rates.
Vendors at the symposium also exhibited other kinds of AI-based software. These included an algorithm being developed by Lunit to analyze 2-D mammograms and one by a different company, Koios, that does the same for sonograms.
Seoul-based Lunit is developing AI for applications in mammography, both 2-D and tomo, as well as in computed tomography (CT) of the chest and coronaries. The 2-D mammography software, now in review for FDA clearance and the CE mark from the European Union, detects breast cancer lesions with up to 97 percent accuracy in full field digital mammograms (FFDM), according to the company. Lunit Insight for Mammography was described on the SBI exhibit floor as a “diagnostic support tool” focused primarily on screening mammography.
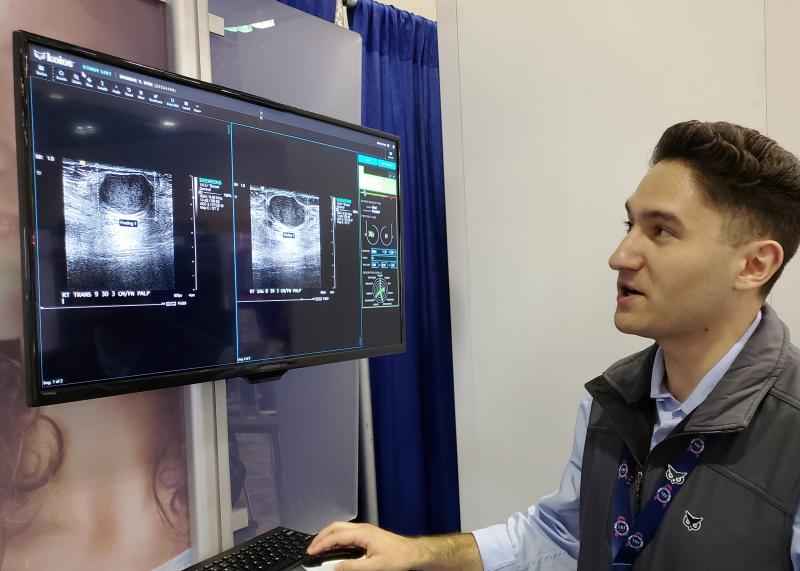
Koios framed its software as a “diagnostic assistant.” The software is designed to provide decision support for physicians and technologists using breast ultrasound. A version compatible with major picture archiving and communication systems (PACS) has cleared the FDA and is available commercially. Another is being tailored for use onboard GE Healthcare’s Logiq E10 high-performance ultrasound scanner.
Why Risk Stratification Is Important
Smart algorithms in the future may have an even greater impact, helping women who are considering breast cancer screening factor in a myriad of risks, including family history and breast density, versus today’s reliance on a single risk factor, age. Such risk stratification might be accomplished without imaging, according to Michael Klein, iCAD executive chairman and CEO, starting with women completing questionnaires that would characterize risk factors. The answers, processed using an AI algorithm, might spot high-risk women on the basis of cited risk factors. Doing so “may encourage more women to get a mammogram,” Klein said.
Today age is the determinant most often cited in guidelines that address screening mammography. At least one recommends that screening begin at age 50; others advise much younger starts, one as early as age 40 (the American Cancer Society Guidelines for the Early Detection of Cancer).
“But there are women in their 50s who are at lower risk than someone in their 40s,” said Diana Miglioretti, Ph.D., a biostatistics professor at the University of California, Davis. “Using a risk-based approach would actually identify more women with potential benefit from screening than using just age.”
AI might be used as a means for achieving risk stratification. Building on its exclusive partnership with researchers at The Karolinska Institutet in Stockholm, Sweden, iCAD may develop an AI algorithm that uses risk categories to suggest which women might benefit from additional or more frequent screening. Physicians would be part of the evaluation, Klein emphasized: “We can be descriptive and use predictive analytics, but we can’t be prescriptive. Only the physician can be prescriptive.”
Using AI To Stratify Risk
GE may also leverage risk stratification, potentially using its propriety AI platform, Edison, which was unveiled at RSNA 2018. The Edison platform is intended to support the application of AI tools to virtually any modality. Already it has been applied to digital X-ray in GE’s development of the Critical Care Suite, comprised of AI algorithms that could assist physicians in their diagnosis of abnormalities affecting critically ill patients.
Edison might be applied to mammography, according to Agnes Berzsenyi, president and CEO of GE Healthcare Women’s Health, who described Edison as not only having the capacity to host different AI applications, but that “the Edison platform benefits developers.”
The company has long worked with iCAD in the development of software compatible with GE mammography equipment. In 2007, for example, iCAD and GE officially announced an agreement to customize a version of iCAD’s SecondLook Digital for GE Healthcare’s Senographe and Seno Advantage systems. SecondLook Digital was described at the time as potentially helping radiologists distinguish cancers from other anomalies in the breast. The partnership between the two companies is continuing.
How Productivity And Efficiency Go Hand-in-Hand
Productivity was a central point of conversation on the symposium exhibit floor. “We can be more productive and not lose anything (of diagnostic value),” said Pam Cumming, senior director of product marketing for women’s health at Siemens Healthineers USA, about use of the company’s wide-angle tomosynthesis technology for screening.
Ernie Liu, Siemens product marketing specialist for women’s health, described the potential gains in both productivity and accuracy that might come from using this technology. Its use, Liu said, can translate into faster interpretations and more confident diagnoses.
“They (physicians) see much more clearly — without dense tissue overlapping,” Liu said.
Radiologists care about productivity, as demonstrated by their interest in knowing how well they have done. Research done by Jules Sumkin, D.O., chairman of the Department of Radiology at the University of Pittsburgh Medical Center (UPMC) in Pennsylvania, indicates that radiologists want to know the outcome of cases recommended for recall or biopsy.
On April 5, in a talk titled “Individualized automated continuous feedback of breast imaging interpretations and outcomes for improved performance,” Sumkin described the use of a PACS module at the UPMC that tells breast imagers what has become of patient recalls and subsequent biopsies. Only two of the 19 radiologists who interpret breast images at UPMC reviewed fewer than half the cases made available to them. In total, 79 percent of the 3,427 cases logged by the software over a two-year period were reviewed by radiologists.
Just as productivity appears to be a key consideration for radiologists, so was it on the minds of visitors to the GE Heathcare booth, where the Senographe Pristina Serena was center stage. This system is a variant of the Senographe Pristina 3-D mammography system, distinguished by an add-on biopsy kit.
Biopsies are performed while the breast is compressed. “We want radiologists to have confidence that they in fact did (sample the suspicious area of the breast),” said Kathleen Schindler, GE Healthcare global clinical mammography product leader. “So all the features of making the patient comfortable and very easy to position on Pristina apply exactly to the biopsy.”
Additionally, the commercially available system allows biopsies from the side of the breast, which allows samples to be extracted regardless of breast size, Berzsenyi noted. “This (also) is not only helping to give more working space but the patient can look away, which can also reduce anxiety,” she said.
The entire exam, including biopsy, can be done within 15 minutes, according to Berzsenyi.
Options for the Aspire Cristalle from Fujifilm Medical Systems USA were focused on productivity. S-View, which synthesizes a 2-D image from data obtained during digital breast tomosynthesis, was shown along with a reconstruction process, called iterative super-resolution reconstruction (ISR).
“ISR helps reduce noise (and enhances detail),” said Susan Crennan, Fujifilm product manager for women’s health, who noted that the reconstruction process is used in the company’s S-View. These gains do not compromise the speed of image acquisition, she said.
The third option that FujiFilm showcased, an option called Tomosynthesis Spot, uses tomo data to precisely visualize a specific area of concern. This capability, according to Crennan, exactly fits into physician workflow.
How Communication Affects Productivity
Konica Minolta Healthcare Americas highlighted features of its Exa Mammo, a PACS designed for breast imaging centers. Two features — namely, Exa Chat and Exa Peer Review (both of which the company expects to make available later this year) — were developed to help improve communications among providers. Emily Lafella, director of women’s healthcare enterprise imaging HCIT at Konica Minolta Healthcare Americas, highlighted two core features of Exa Mammo — its zero-footprint viewer and server-side rendering.
“We are doing everything we can to provide everyone in the breast imaging facility access to everything they need,” Lafella said, “whether that be a screening mammogram; or maybe they’re coming back for a biopsy; or maybe they have (a patient who has) been diagnosed with cancer.”
Seeing pathologies clearly — and quickly — is the underpinning of Barco Healthcare’s Coronis Uniti, whose display has a 33.6-inch diagonal and resolution of 4,200 by 2,800. The size and luminance of the monitor, showcased at the symposium, help differentiate it from competitors, according to Albert Xthona, strategic product manager of the Barco Healthcare Division.
“It lets you see the smallest detail quickly,” Xthona said. “The high luminance combined with the high resolution definitely (provides) high image quality.”
Because of this, the monitor is routinely sold for a variety of radiological purposes, he said, echoing the theme of productivity heard elsewhere on the symposium exhibit floor. “It (Coronis Uniti) is enabling people to do more work in the same amount of time.”
The Benefits Of Wire-free Localizers
Wires have traditionally been placed prior to lumpectomy to mark cancerous tissues in the breast. Wire-free localizers, however, provide alternatives that could make hospitals and care providers more productive, while benefiting patients.
Cianna Medical featured the implant of a tiny radar reflector in place of a wire. Leica Biosystems’ Mammotome showcased a magnetic seed for implantation, as well as a magnetic liquid injectable that accumulates in the sentinel lymph node, which surgeons may remove from patients undergoing mastectomy. The Mammotome tracer is approved by the FDA for use specifically in patients undergoing mastectomy for breast cancer.
Because wires, which protrude from the breast, can keep patients from going home, patients traditionally have had the wires implanted the morning of surgery. This has forced radiologists to implant the wires the same day as lumpectomies and surgeons to schedule procedures after implantation. Any delays can potentially cause problems for the surgeons as well as in the use of operating rooms.
“So not only is (wire-free localization) better for the patient, it is more efficient,” said Mike Numamoto, vice president of marketing for Cianna Medical, which makes the Savi Scout Radar Localization system.
Cianna’s Scout allows physicians to localize the implanted reflector to within 1 mm, according to Numamoto. The radar signal, fired by a handheld wand, is reflected by the implant. It is then processed and displayed by the Scout console
to indicate the distance between the wand and
the reflector.
Rather than relying on an external source transmission, a Mammotome probe detects magnetic fields emanating from its implanted Magseed markers or injected Magtrace Liquid. Magseed is used to localize breast tissue that the surgeon intends to remove; the liquid tracer is designed to help find the sentinel lymph node to which the breast cancer may have metastasized.
“If you want to see if the cancer has spread to the lymph node (and) you don’t know which lymph node to check, you have to map it,” Hafemeister said. “This is a radioactive-free option.”
Although, in the end, productivity is just one variable of the value-medicine equation, the variables of this equation are inextricably linked. Productivity depends on efficiency.
Yet both affect the patient, as the shadow of patient benefit falls on all of healthcare.
Greg Freiherr is a contributing editor to Imaging Technology News (ITN). Over the past three decades, Freiherr has served as business and technology editor for publications in medical imaging, as well as consulted for vendors, professional organizations, academia and financial institutions.
Related content:
VIDEO: Age, Interval and Other Considerations for Breast Screening
BOOK: Breast Cancer Screening: Making Sense of Complex and Evolving Evidence
Risk Stratification for Screening Mammography: Benefits and Harms
VIDEO: A Discussion on Proposed FDA Rules for Mammography Reporting
FDA Proposes New Rules for Mammography Reporting and Quality Improvement





 May 12, 2026
May 12, 2026