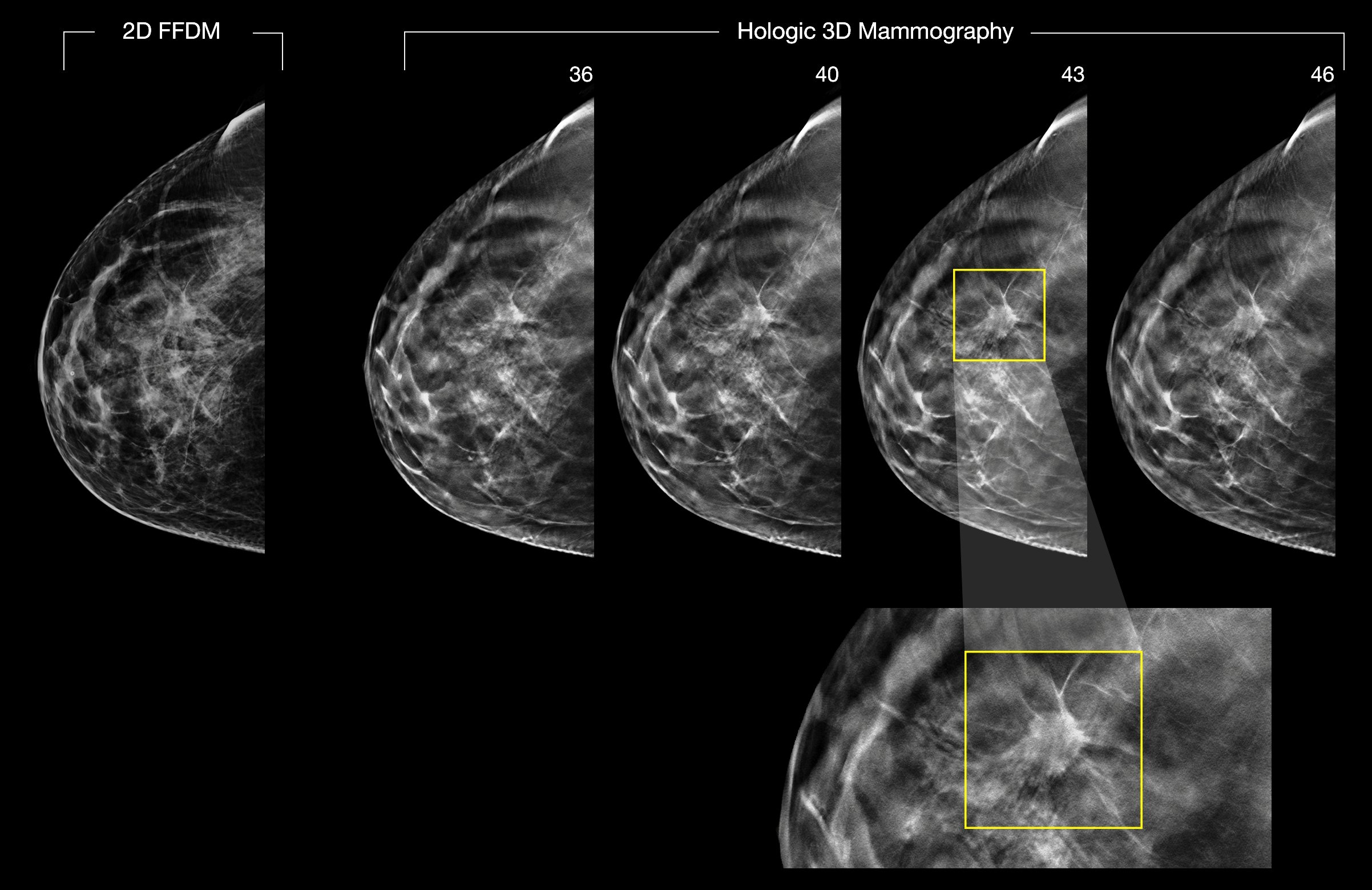
Since the widespread adoption of digital imaging and PACS, referring physicians seldom visit radiology reading rooms, substantially reducing a major source of feedback for radiologists. (Shown are 2-D and 3-D digital breast images.) A software module to be described April 5 at the SBI/ACR Breast Imaging Symposium has been providing that feedback for radiologists interpreting breast images at the University of Pittsburgh Medical Center. Image courtesy of Hologic
The use pattern of a picture archiving and communication system (PACS) software module demonstrates that radiologists want to know the outcome of cases recommended for recall or biopsy, according to Jules Sumkin, D.O., chairman of the Department of Radiology at the University of Pittsburgh Medical Center (UPMC) in Pennsylvania. Enthusiasm for the software was so high that it has been modified to deliver feedback for cases outside breast imaging.
Sumkin will describe performance of the “proof of concept” module at the Society for Breast Imaging (SBI)/American College of Radiology (ACR) Breast Imaging Symposium on April 5 in a 1:30-2:30 pm scientific session during a talk titled “Individualized automated continuous feedback of breast imaging interpretations and outcomes for improved performance.”
Engineers at UPMC built the software into the radiology department’s PACS. As initially configured in early 2017, the module tells radiologists the results of recommended recalls and biopsies. Its effect, if any, on recall rate or the positive predictive value of biopsies could not be measured, Sumkin noted. Nor was doing so the original intent. The module was designed and installed to fill a void created by the adoption of digital imaging and PACS.
“Since everything is electronic, we don’t have colleagues coming into the reading room, telling us about what happened to our cases,” he said. “Basically we stopped learning.”
The PACS module solves that problem, Sumkin said, by telling breast imagers what has become of patient recalls and subsequent biopsies.
The software automatically creates a work list of patient recalls, noting whether results have been entered into the PACS. The involved radiologists are messaged upon signing into the PACS if results from their recommended recalls and biopsies are available.
A work list of 20 cases is maintained by the software for each radiologist. The most recent cases are added to the top. Cases reviewed by the radiologist are dropped automatically. If the list expands to more than 20, the oldest cases are dropped automatically.
Patient Volume Led Initially To Breast Imaging
The concept was proved in breast imaging because of the high volume of studies, particularly ones that involve screening mammograms, said Sumkin, who himself interprets many mammograms.
The UPMC radiology chairman will present two years of data at the SBI symposium. Beginning in February 2017, 3427 cases were logged by the software; 79 percent were reviewed by radiologists, he said. “You can look at the diagnostic. You can look at the biopsy. You can look at the rad correlation with the pathology. And then the software acknowledges (that the radiologists have looked at the case),” Sumkin said. “That is the way we tracked that they actually used the software.”
The 19 radiologists who interpret breast images at UPMC were each given a 10-minute training course on using the software. Only two reviewed fewer than half the cases made available to them. Radiologists were neither enticed nor pressured to use the system, Sumkin said.
“We wanted to find out if, after we showed them how to use the tool, whether they would use it,” he said.
The software has since been modified for more extensive use throughout the radiology department, Sumkin said. UPMC radiologists can now request that the software “follow up their suggestions,” for example, that they be notified about results from a chest computed tomography (CT) scan after one was ordered following a chest radiograph.
“Now they’ll know,” he said.
Greg Freiherr is a contributing editor to Imaging Technology News (ITN). Over the past three decades, Freiherr has served as business and technology editor for publications in medical imaging, as well as consulted for vendors, professional organizations, academia, and financial institutions
Related content:
VIDEO: What is New in Breast Imaging Technology
.



 May 22, 2026
May 22, 2026 









