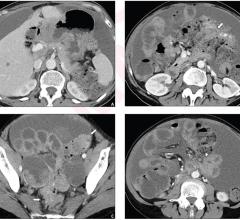
Contributing Editor Greg Freiherr offers an overview of computed tomography (CT) advances at the Radiological Society of North America (RSNA) 2015. The video includes Freiherr during his booth tours with some of the key vendors who were featuring new technology.
Technology Report:
Computed Tomography (CT)
Related Content
News | Artificial Intelligence
September 20, 2023 — Medical imaging artificial intelligence (AI) company Annalise.ai has announced that the results…
Sponsored Content | Case Study | Radiology Imaging | By Tim Hodson
In June, the Philips Radiology Experience Tour hit the road to provide healthcare professionals with an opportunity to…
News | Computed Tomography (CT)
September 19, 2023 — An advanced CT test can identify individuals with stable angina at a reduced risk of three-year…
Sponsored Content
Feature | Information Technology
AT A GLANCE Organization: Expert Radiology Management Services, LLC Specialty: Subspecialty teleradiology — neuro and ...
News | FDA
September 13, 2023 — Annalise.ai, a leader in AI-powered medical imaging solutions, announced the receipt of 510(k)…
September 8, 2023 — A simple, noninvasive contrast enhanced ultrasound (CEUS) scan is an ideal tool for resolving…
Feature | PET Imaging
According to a new report from Transparency Market Research (TMR), PET radiotracers are expected to rise at a CAGR of 8…
Sponsored Content
Sponsored Content
Videos | Radiology Business
Radiology departments have many different needs and face a wide variety of challenges that can impact their departments ...
News | Radiology Imaging
August 24, 2023 — Medical imaging via X-rays, CT scans, MRIs and ultrasounds provide health-care professionals with…
News | Radiology Business
August 17, 2023 — SSM Health and Siemens Healthineers have announced a new 10-year strategic partnership agreement…
News | Contrast Media
August 17, 2023 — University of Missouri School of Medicine neurologist Adnan Qureshi, MD recently led a study that…
Sponsored Content
Feature | Breast Imaging
Despite decades of progress in breast imaging, one challenge continues to test even the most skilled radiologists ...
Sponsored Content | Videos | Radiology Imaging
This summer, the Philips Radiology Experience Tour has been bringing Philips imaging modalities directly to the…
News | Computed Tomography (CT)
August 14, 2023 — Precision Imaging Centers has added Fujifilm Healthcare Americas Corporation’s Scenaria View low-dose…
August 14, 2023 — GigXR, Inc, whose immersive learning platform delivers a catalog of complementary XR applications for…
Sponsored Content
Sponsored Content
Videos | Radiology Business
Bayer Radiology’s Barbara Ruhland and Thom Kinst discuss how radiology departments can address the many different ...
News | Artificial Intelligence
August 9, 2023 — Annalise.ai, one of the global leaders of AI decision-support solutions, announced that their Annalise…
News | Artificial Intelligence
August 7, 2023 — AI tools that quickly and accurately create detailed narrative reports of a patient’s CT scan or X-ray…
News | Artificial Intelligence
August 7, 2023 — GigXR, Inc, whose immersive learning platform delivers a catalog of complementary XR applications for…
Sponsored Content | Case Study | Enterprise Imaging
The healthcare industry faces many different types of obstacles in today’s challenging marketplace.
Staff shortages,…
News | Computed Tomography (CT)
July 31, 2023 — The American College of Radiology (ACR) has issued a statement regarding ACP colorectal cancer…
News | AHRA
July 24, 2023 — The Association for Medical Imaging Management (AHRA) announced that GE Healthcare won the 2023…
News | Computed Tomography (CT)
July 13, 2023 — New computed tomography (CT) technology allows for a comprehensive, simultaneous evaluation of lung…
News | Computed Tomography (CT)
July 13, 2023 — According to an accepted manuscript published in the American Journal of Roentgenology (AJR), a…
© Copyright Wainscot Media. All Rights Reserved.
Subscribe Now

 September 20, 2023
September 20, 2023