February 9, 2024 — Multiple sclerosis (MS) is a neurological disease that usually leads to permanent disabilities. It ...
Radiology Imaging
The radiology imaging channel includes technology news related to computed tomography (CT), digital radiography (DR / X-ray), ultrasound, magnetic resonance imaging (MRI), radiographic fluoroscopy (R/F), mammography, angiography, 3-D printing, contrast media injectors, molecular imaging, neurological imaging, pediatric imaging and radiation dose management.
At RSNA23, Imaging Technology News (ITN) spoke with Bhvita Jani, principal analyst at Signify Research, about ...
February 6, 2024 — PIUR IMAGING, a European provider of independent tomographic 3D ultrasound solutions, announced the ...
SPONSORED CONTENT — Fujifilm’s latest CT technology brings exceptional image quality to a compact and user- and patient ...
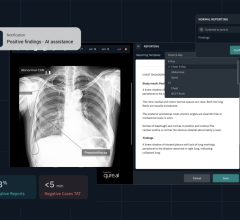
February 6, 2024 — Medical imaging AI innovator, Qure.ai, has received breakthrough device designation from the Food and ...
February 6, 2024 — An update to the CT Colonography Reporting and Data System (C-RADS) has been published Jan. 30 in the ...
February 6, 2024 — The Society of Nuclear Medicine and Molecular Imaging (SNMMI) held its 2024 SNMMI Mid-Winter Meeting ...
Agfa Radiology Solutions is committed to enhancing clinical outcomes and operational efficiency, underscoring its ...
February 2, 2024 — FUJIFILM Sonosite Inc., a leader in point-of-care ultrasound (POCUS) solutions, announced the launch ...
February 1, 2024 — Banyan Software, a leading acquirer and permanent home for great software businesses, announces the ...
It's a new year, and as another month comes to a close, ITN takes a look at the Top 10 most-read pieces of content from ...
Agfa Radiology Solutions delivers diagnostic imaging solutions that set the standard in productivity, safety, clinical ...
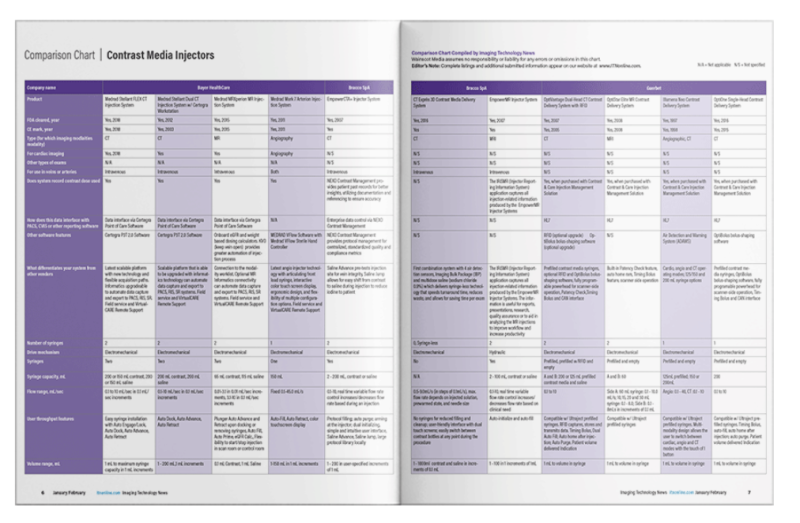
Did you know that Imaging Technology News (ITN) maintains more than 40 comparison charts of product specifications from ...
This gallery includes photos of the wide range of medical imaging technologies, scientific sessions, educational courses ...
January 25, 2024 — Esaote Group, a leading Italian innovator in medical imaging, today unveiled its new brand identity ...
In June, the Philips Radiology Experience Tour hit the road to provide healthcare professionals with an opportunity to ...
January 24, 2024 — Whole Body MRI, a private clinic committed to delivering accurate and comprehensive diagnostic ...
January 24, 2024 — A study by the Neiman Health Policy Institute found that, by 2021, only 1.1% of radiologists’ ...
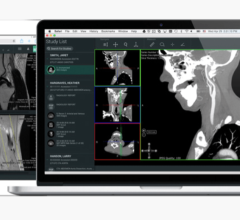
January 23, 2024 — Siemens Healthineers announces the Food and Drug Administration (FDA) clearance of syngo Virtual ...
Updates on AI in Radiology, RSNA Programs and Stanford Initiatives Listen and learn with ITN’s newest “One on One” video ...
January 18, 2024 — Abbott announced that the U.S. Food and Drug Administration (FDA) has approved expanded MRI labeling ...
January 17, 2024 — Clarius Mobile Health, a global leader in wireless ultrasound solutions, has received CE Mark for its ...
January 17, 2024 — The Radiological Society of North America (RSNA) is launching a new artificial intelligence (AI) ...
According to research conducted by Polaris Market Research, the global positron emission tomography (PET)/computed ...

 February 09, 2024
February 09, 2024