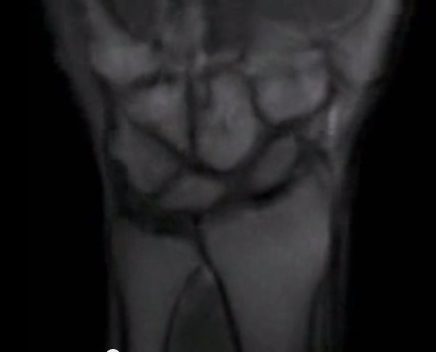
January 6, 2014 — University of California, Davis radiologists, medical physicists and orthopaedic surgeons have found a way to create "movies" of the wrist in motion using a series of brief
magnetic resonance imaging (MRI) scans. Called "Active MRI," the technique could be useful in diagnosing subtle changes in physiology that indicate the onset of conditions such as wrist instability.
The outcome of the team's first test of the new technique is published online in the journal PLOS ONE, titled “Real-Time Magnetic Resonance Imaging (MRI) During Active Wrist Motion — Initial Observations.”
"These fast images are like a live-action movie," said Robert Boutin, professor of radiology, UC Davis, and lead author of the study. "The movie can be slowed, stopped or even reversed as needed. Now patients can reproduce the motion that's bothering them while they're inside the scanner, and physicians can assess how the wrist is actually working. After all, some patients only have pain or other symptoms with movement."
Wrist instability, explained Abhijit Chaudhari, Ph.D., assistant professor of radiology, UC Davis, and senior author, occurs when carpal bones become misaligned and affect joint function, often as a result of trauma that injures the ligaments between wrist bones. It causes abnormal mobility and chronic pain that can lead to osteoarthritis, a major socioeconomic burden to patients and healthcare systems. Good outcomes in managing the condition are more likely with early diagnosis, when less-invasive treatments are possible.
Methods such as dynamic computed tomography (CT) and fluoroscopy can image the moving wrist, but these approaches involve radiation and do not show soft tissue such as ligaments — a major part of the wrist's intricate architecture — as well as MRI scans.
"MRI scans provide detailed anatomical information of wrist structures without using ionizing radiation, but they cannot help diagnose problems with bone or tendon position that are best seen when the wrist is moving," said Chaudhari. "Active MRI provides a detailed and 'real time' view of the kinesiology of the wrist in action using a widely available and safe technology."
The researchers overcame a number of hurdles in adapting MRI capabilities to providing moving images. A complete MRI exam usually takes 30 to 45 minutes, with each image set requiring at least three minutes — not nearly fast enough to make a video. The team developed a new MRI protocol that takes one image every 0.5 seconds, delivering a series of images in 30 seconds.
Another barrier was the presence of imaging errors called banding artifacts. Movement of the bones in the wrist area can interfere with the scanner's magnetic field, creating signal drop-offs. The resulting dark bands can obscure the moving wrist. The team overcame this problem with dielectric pads, which stabilize the magnetic field and shift artifacts away from the area of interest and to the side, allowing doctors to clearly see the wrist bones.
For the current study, Active MRI was tested on 15 wrists of 10 subjects with no symptoms of wrist problems. The participants' wrists were imaged as they performed motions such as clenching the fist, rotating the wrist and waving the hand side-to-side. Each exam lasted 10 minutes.
"It's quite phenomenal that we can look inside the body while it's in action using MRI," said Boutin. "Routine MRI provides exquisite details, but only if the body is completely motionless in one particular position. But bodies are made to move. We think Active MRI will be a valuable tool in augmenting traditional, static MRI tests."
"Our next step is to validate the technology by using it on patients with symptoms of wrist instability," said Chaudhari. "We also want to use Active MRI to study sex distinctions in musculoskeletal conditions, including why women tend to be more susceptible to hand osteoarthritis and carpal tunnel syndrome."
Additional authors were Michael Buonocore, M.D., Ph.D., Igor Immerman, M.D., Zachary Ashwell, Gerald Sonico and Robert Szabo, M.D., all from UC Davis. The National Institutes of Health (NIH), UC Davis Imaging Research Center and UC Davis Department of Radiology funded the research.