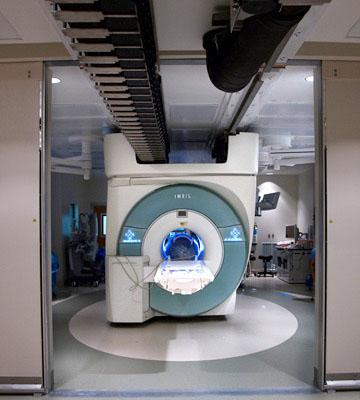
The VISIUS Surgical Theatre at Le Bonheur Hospital in Memphis, Tenn., installed in January 2011, features an intraoperative MRI that moves between operating and diagnostic rooms on ceiling rails. A study at the hospital is crediting the iMRI with reducing resurgery rates. (CNW Group/IMRIS Inc.)
June 26, 2013 -- IMRIS Inc. reported that Le Bonheur Children's Hospital in Memphis, Tenn., is crediting intraoperative MRI (iMRI) within the VISIUS Surgical Theatre with reducing returns to the operating room for residual tumor removal by 84 percent over 2 years.
The VISIUS Surgical Theatre at Le Bonheur provides neurosurgeons with on-demand access to real-time structural brain images before, during or after a procedure without moving patients from the surgical table as the iMRI moves between rooms using ceiling rails. The multifunctional neurosurgical environment, installed in 2011, also allows for surgery in one room and diagnostic scanning in another room, in addition to intraoperative imaging.
"iMRI is an invaluable tool for me. In most pediatric brain tumors the goal is to maximally resect the entire tumor," said Paul Klimo, chief of the division of pediatric neurosurgery at Le Bonheur and University of Tennessee Health Science Center. "This is a huge step in achieving this objective. For certain tumors, we have been able to improve our precision and get to them easier. We are now able to leave the OR with the knowledge of whether a tumor was completely resected or not. If not, then it is almost always because the residual tumor cannot be safely resected. Almost all of my tumor operations are done using it. I've also used it to demonstrate complete resection of arteriovenous malformation (AVM) and in tumor biopsies."
In 2012, 47 percent of Le Bonheur's brain tumor surgeries were performed using VISIUS iMRI - and none of those surgeries required returns to the OR for residual tumor. In addition, the iMRI also eliminates the need, in many cases, for additional sedation that would be needed for post-operative MRI, or additional surgeries for residual tumor.
Ranked among the top 25 children's neuroscience programs by the US News & World Report in 2012, Frederick Boop, M.D., chairman of the department of neurosurgery and co-director of Le Bonheur's Neuroscience Institute, said the hospital has an on-going quality improvement effort to improve this ranking, overall reputation and patient outcomes. The hospital's reputation growth has brought an increase in patients locally but most notably outside the region, Boop said. During the last few years, he said, survival rates for various tumors, in some cases, far exceed typical rates.
"Our protocol of using iMRI for certain procedures is safer than previous workflow of imaging only pre- and post-operation," said Boop. "Previously when using ordinary MRI with these patients, we were nervous about anesthesia, lines and other issues of moving the patient," he said. "The iMRI has allowed us to get a more complete removal of these tumors more often than before without bringing the patient back for another operation."
IMRIS CEO David Graves said these results reinforce the value of iMRI in the VISIUS Surgical Theatre. "This shows that having immediate access to the iMRI without moving or changing the position of the patient to see and remove the entire tumor limits the chance, costs and other issues related to returning a patient to surgery," he said.


 May 22, 2026
May 22, 2026 









