Invented in 1896 by Enrico Salvioni, the fluoroscope remains a flagship technology of modern medicine. The live video X-ray image it provides can guide a catheter safely through a living patient’s circulatory system, delivering a therapeutic action precisely where needed. As an interventional cardiologist, I’d be blind without my fluoroscope, and the life-saving procedures it permits would be impossible.
Unfortunately, the machine’s great power comes from the X-ray beam it uses to penetrate and image the human body’s interior. The very high frequency, short wavelength electromagnetic radiation generated in its X-ray tube is a well-known danger to living beings, and must be very carefully controlled. Most of us who work with radiation in medical applications believe we are controlling it, but that may stem more from complacency than from facts.
Within the last decade, studies have revealed that interventional cardiology and cardiac electrophysiology staff experience increased rates of cancer, skin lesions, cataracts and orthopedic illnesses as compared with their unexposed colleagues, even though they had adhered to international and federal radiation dose limits. These maladies increased with the amount of time spent conducting interventions.
While the diagnostic and treatment benefits of radiologic medicine are far too valuable to give up, we deny its downside at our peril: an increased risk of debilitating and potentially lethal health effects for the doctors, nurses, technicians and other staff who work in the catheterization lab daily and absorb small amounts of scatter radiation repeatedly over the course of their careers.
This risk is compounded by the trend toward higher-power machines to produce sharper images. It’s the Catch-22 of a life in the catheterization lab: the better fluoroscopes get at helping our patients, the more they seem to hurt our healthcare team.
While most healthcare providers know about the dangers of direct radiation and take steps to avoid exposure, the threat of scatter radiation is less commonly understood. But over time, it can be just as dangerous. To help them grasp the concept, I tell my students to think of a high-tech heist movie, where the treasure to be stolen is protected behind a wall of crisscrossing laser beams: when you break one beam the alarm sounds. It’s much the same with scatter radiation in the cath lab, except that the beams are invisible and harmful, and no alarm sounds when we move through them.
That’s why it’s a good idea, from time to time, to refresh our understanding of the risks and dangers of scatter radiation during fluoroscopic interventions, along with the best practices and new technologies that are making it easier to stay safer in the cath lab. With these in place, we no longer have to choose between improving our patient’s health and protecting our own.
Risks and Dangers
Over more than a century using radiation in medical applications, we’ve learned a lot about what it can do, for better and worse. Unseen but for the damage it leaves behind, ionizing radiation is dangerous both acutely in higher doses and cumulatively in lower doses over time, as happens with scatter radiation in the catheterization lab.
The damage it can wreak on the human body takes one or more of the following forms:
•Direct effects. These injuries result from acute overexposure to a directed radiation beam or proximity to a radioactive substance such as uranium, and can include all levels of burns to the skin and underlying tissue, radiation sickness, and death. Modern medical equipment is designed to prevent such massive overdoses.
•Stochastic effects. Like an insidious poison, low doses of radiation repeated over time can increase one’s risk of acquiring naturally occurring cancers. This is because radiation damages the genetic code deep within cell nuclei, increasing the chance that mistakes in the repair process could lead to a cancer-causing mutation to be incorrectly inserted into one’s DNA. Stochastic effects for cath lab staff also include cataracts and cognitive problems.
•Genetic effects. Damage to a chromosome that is repaired with an incorrect sequence can cause serious genetic mayhem, and it can be passed on to subsequent generations.
•Embryo and fetus effects. A developing child is particularly vulnerable to radiation’s dose-dependent effects, which can include death or congenital abnormalities that appear at birth or later in life.
For fluoroscope users like me, no list of radiation’s dangers would be complete without mentioning the pain, fatigue and occasionally debilitating effects caused by wearing heavy garments, an antiquated but still technically effective way to protect staff. In fact, I’ve known cath lab colleagues who were forced to retire from the field due to long-term damage caused by these cumbersome devices. With 12 years of training required for each interventional cardiologist, losing them to back pain seems a terrible waste of resources. Thankfully, lighter, lead-free alternatives are proliferating along with non-apparel methods to protect the whole room, and these will form the core of an effective 21st century fix for the problem.
Solutions
The solution to radiation exposure is radiation protection, and when it comes to policies that can best protect cath lab staff from scatter radiation, the guiding principle must be ALARA, the acronym for “as low as reasonably achievable.” It means in all instances one’s mindset should be to use the minimum amount of radiation to get the job done and produce the least exposure. This is especially important when it comes to personal protective equipment, as forgetting to don it before entering the danger zone can lead to real trouble. A protective gear checklist to review when suiting up can help, as well as maintaining an environment where staff are encouraged to continually check each other’s safety status.
Time, distance, shielding and dose monitoring are the time-tested pillars of radiation protection in medical settings. Combined with an ALARA mindset, they imply the following directives:
•Time. Minimize your time operating the fluoroscope or being in the room while it’s on.
•Distance. Maximize your distance from the radiation source. Two steps away from the table cuts your exposure by half.
•Shielding. Put as much shielding as possible between you and the radiation source.
•Monitoring. Wear a personal dosimeter to monitor and gauge your exposure.
Ultimately, all cath lab staff should be fully educated on scatter radiation’s dangers and the policies, practices, and technologies in use to defeat it.
Fluoroscope Settings
Fluoroscopic image quality can suffer from insufficient power, usually because the image is too noisy or cluttered for a low dose scan. High dose settings (sometimes called detail mode) can improve image quality by boosting contrast, but this sends more radiation to the patient and more scatter into the room. In practice most of the time, the low power setting produces an excellent though slightly less sharp image, with no practical reduction in diagnostic value.
The following habits can also minimize overexposure due to machine settings:
•Higher magnification and frame rates increase radiation overall, so use lower settings for these features unless a higher one is necessary.
•Use the “fluoro save” feature to save the last image and reduce the need for more imaging.
•Place lead drapes under the patient table, avoiding obstructions to C-arm travel.
•Put the X-ray source under the patient table as far away as possible to reduce scatter radiation by directing it through the table and patient before it reaches staff, and place the X-ray detector as close to the patent as possible to produce the sharpest image.
•Use tubing extensions to maintain a two-step distance from the table during imaging.
•Avoid using the fluoroscope if a non-radiological imaging device can do the job; ultrasound, magnetic resonance imaging (MRI), optical coherence tomography (OCT), intravascular ultrasound (IVUS) or transesophageal echo (TEE) might be a safer alternative.
Other factors that can affect radiation scatter include larger patients. Modern fluoroscopes with automatic brightness control (ABC) will increase their power to penetrate patients with thicker or denser than average bodies. In these cases, the fluoroscopist should check if the ABC can be turned off and still produce an acceptable image.
Technology to the Rescue
A technological fix is always tempting, but we must remember that scatter radiation is a problem that sprang from a previous technological fix — the use of X-rays to image the inner body. Every device designed to solve this problem will likely have positive and negative aspects that warrant careful consideration, and you may have to change the way you practice to reap all the benefits they promise.
Anyone who has worn leaden shielding garments for this type of work will be quick to suggest lightening the load, and modern medical science is answering the call with lead-free alternatives that dramatically reduce weight without sacrificing shielding power. Removing toxic lead from shielding also prevents it from finding its way into our environment, which is another win for healthcare.
Companies such as RadPad and Vitalcare Products produce a range of lead-free pads, table skirts, drapes, and other innovative shield types that are sterilizable and disposable. They are a simple and less expensive way to put shielding where needed, they keep the ALARA principle alive, and they serve as a helpful adjunct to more complicated, high-tech systems.
The Zero-gravity drape wrap from TIDI Products is one such step up in technical complexity. It offers security, light weight and ease of movement through a suspended lead-acrylic head shield that protects the operator from overexposure while working with the fluoroscope. Its chief advantage is in reducing strain on the back, neck, shoulder, hips, knees and ankles.
Of course, the holy grail of cath lab radiation protection will be a system that protects everyone in the room, and early attempts at such systems have begun to appear.
For example, Egg Medical’s EggNest cath lab table reduces overall scatter by up to 91%, and Rampart’s IC M1 123 independently adjustable acrylic shielding panels give it multiple vascular access points and may block enough X-ray scatter that lead aprons are not required.
Radiaction Medical’s approach to full room protection relies on intuitive controls and an ingenious design to reduce scatter radiation by up to 90%, with up to a 97% reduction to the operator’s head, face and neck. The device doesn’t impede access to the patient, and data indicate it may eliminate the need for up to 75% of protective lead apparel. It attaches unobtrusively to the fluoroscope’s C-arm and deploys robotically on command, extending shielding panels that conform to the patient’s body and to the rotational angle of the C-arm. Afterward, the Radiaction device retracts quickly, minimizing its small footprint even further.
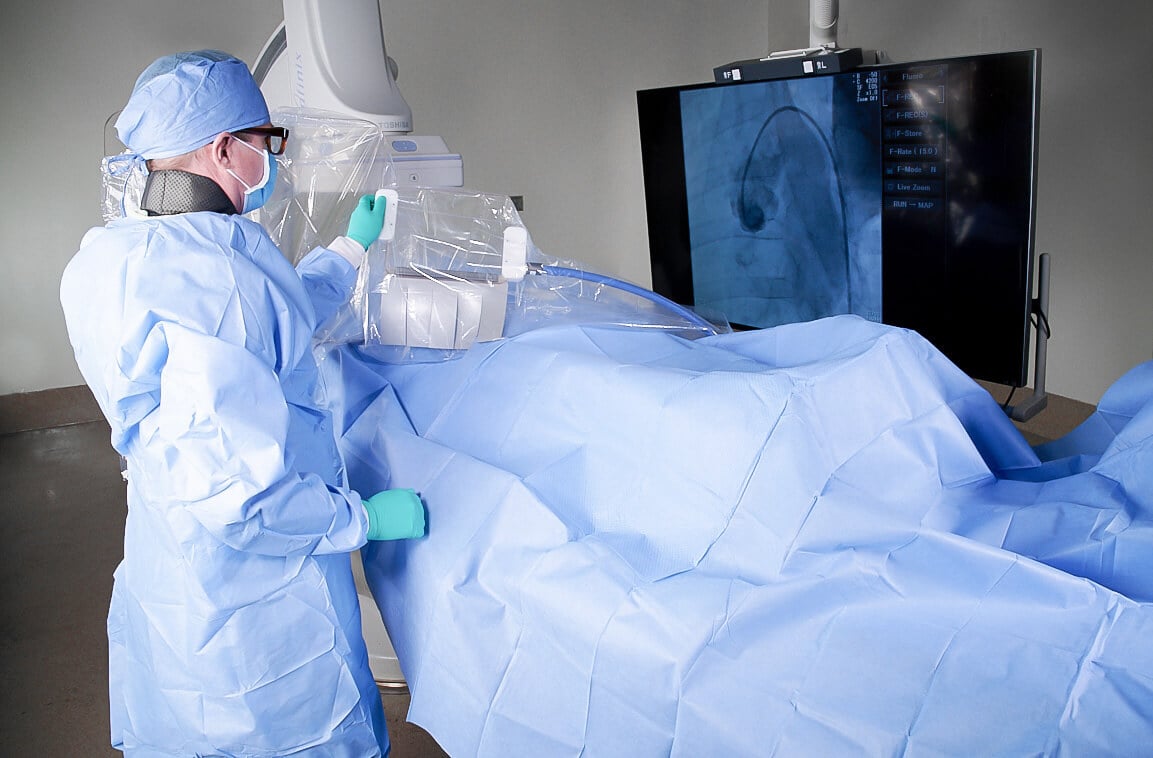
The EggNest radiation protection system reduces radiation exposure without compromising workflow. Image courtesy of Egg Medical.
Moving Forward
Safer fluoroscopic interventions are both possible and necessary, but addressing the dangers of scatter radiation in interventional suites requires a commitment from all involved, from staff who must religiously follow safety protocols to administrators who must provide appropriate, effective tools to ensure our workplace safety. Fortunately for all of us, awareness is spreading, technology is progressing, and a bright future of long, healthy careers in radiologic medicine is well within our grasp.

Mohammad Sahebjalal, MD, is an Interventional Consultant Cardiologist at Musgrove Park Hospital. He was appointed in 2017 making him, at the time, one of the youngest interventional consultants in the UK.
Related Radiation Scatter Content:
Market for MRI-based Radiotherapy Could Soon Widen
Carestream Introduces SmartGrid Software to Reduce Effects of Scatter Radiation
Scatter Radiation from Mammography Presents No Cancer Risk


 May 19, 2026
May 19, 2026 









