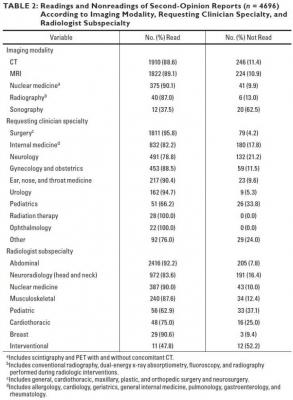
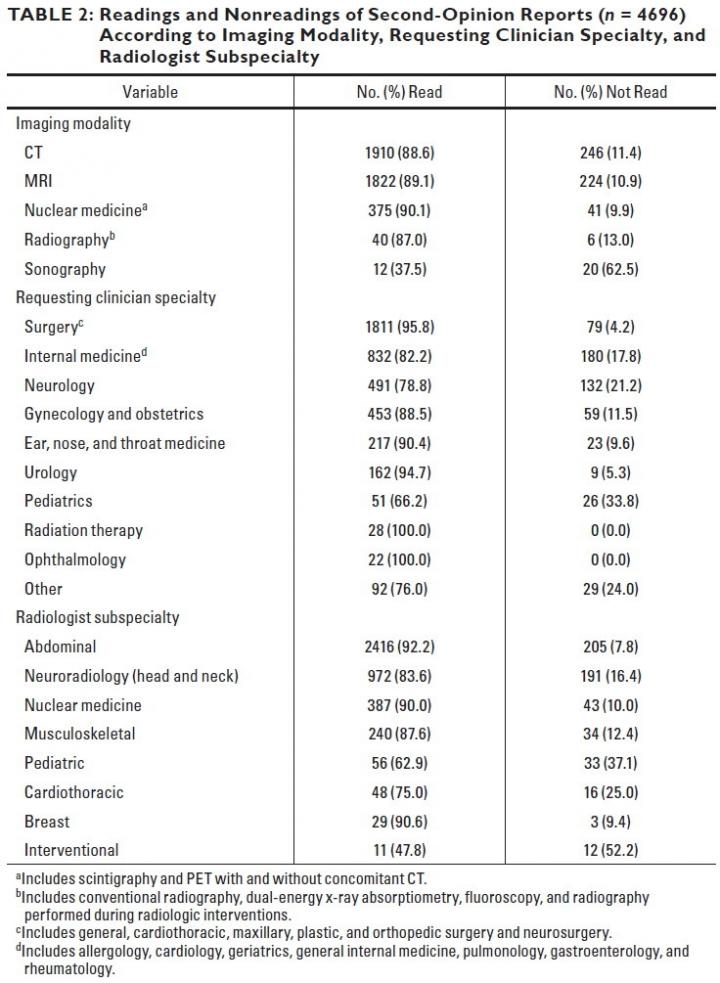
a) Includes scintigraphy and PET with and without concomitant CT. b) Includes conventional radiography, dual-energy x-ray absorptiometry, fluoroscopy, and radiography performed during radiologic interventions. c) Includes general, cardiothoracic, maxillary, plastic, and orthopedic surgery and neurosurgery. d) Includes allergology, cardiology, geriatrics, general internal medicine, pulmonology, gastroenterology, and rheumatology. Image courtesy of American Roentgen Ray Society (ARRS), American Journal of Roentgenology (AJR)
August 14, 2020 — According to ARRS' American Journal of Roentgenology (AJR), clinicians do not read a considerable proportion of second-opinion radiology reports — "a situation that can be regarded as an appreciable but potentially reversible waste of health care resources," the authors of this AJR "Health Care Policy and Quality" article concluded.
Conducted by three radiologists from University Medical Center Groningen in The Netherlands, this retrospective study included 4,696 consecutive second-opinion reports of external imaging examinations authorized by subspecialty radiologists at a tertiary care institution between January 1 and December 31, 2018.
Of the 4,696 second-opinion reports, 537 were not read by a clinician, corresponding to a frequency of 11.4% (95% CI, 10.6-12.3%).
The imaging modality with the highest rate of not being read was sonography (20/32 [62.5%]), the requesting specialty with the highest rate was pediatrics (26/77 [33.8%]), and the radiologic subspecialty with the highest rate was interventional radiology (12/23 [52.2%]).
On multivariate logistic regression analysis, first author Sabine A. Heinz found that the following variables remained significantly and independently associated with the second-opinion report not being read:
- inpatient status (odds ratio [OR], 163.26; p < 0.001),
- sonography as the imaging modality (OR, 5.07; p = 0.014),
- surgery (OR, 0.18; p < 0.001) or neurology (OR, 2.82; p < 0.001) as the specialty of the requesting clinician,
- interventional radiology as the subspecialty of the radiologist who authorized the second-opinion report (OR, 3.52; p = 0.047).
Noting that the National Healthcare Authority of The Netherlands allows up to €100 ($118) to be charged for each second-opinion reading, and that a typical second-opinion reading takes approximately 15 minutes, Heinz and colleagues calculated that the 537 unread second-opinion reports could cost as much as €53,700 ($63,427), as well as approximately 134.25 hours of radiologist interpretation time.
"Although these numbers appear modest, they pertain to a single institution during a 1-year time period," Heinz et al. wrote, adding that cumulative nationwide figures would raise these totals, "possibly substantially," and that the number of unread second-opinion reports will likely increase, "given the projected rise in future second-opinion requests."
Furthermore, since opening the report in the electronic patient file system does not necessarily mean that the clinician actually read said report, Heinz and team contend that the rate of reports not being read (11.4%) is likely an underestimation.
Ultimately, "if subspecialty radiologists and clinicians take proven determinants into account," the authors of this AJR article maintained, "the amount of second-opinion readings with limited additional clinical value may be reduced."
For more information: www.arrs.org


 May 27, 2026
May 27, 2026 









