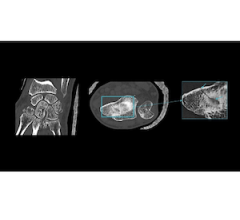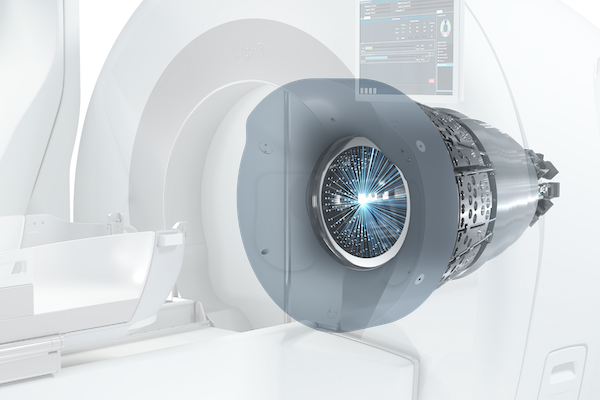
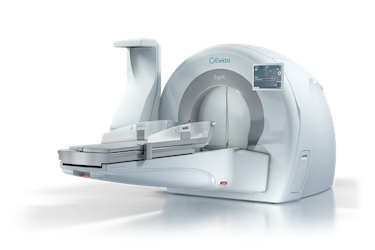
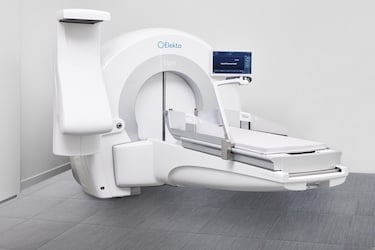
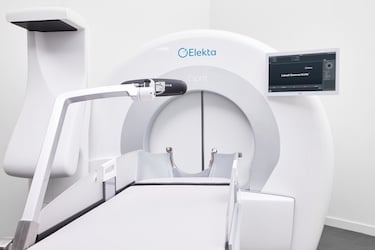
The Elekta Gamma Knife Esprit delivers 192 simultaneous radiation beams, providing a steep dose gradient and accuracy to spare healthy brain tissue. (Photo: Elekta)
Once considered an adjunct brain cancer therapy and a last-resort treatment, noninvasive radiosurgery has evolved dramatically over the past two decades. Today, it is a first-line option for multiple indications, from brain metastases and trigeminal neuralgia to vascular anomalies and select behavioral health conditions.
“Advances in MR imaging and planning, backed a growing body of clinical evidence, make the latest Gamma Knife [the Leksell Gamma Knife Esprit] more predictable, safer, and more effective,” says neuroradiologist Tanvir Rizvi, MD, with UVA Health. “We can now reliably target lesions with millimeter accuracy, which translates into better clinical outcomes. Radiology has been one of the keys to this evolution.”
Expanding the Radiologist's Role
Radiologists play an essential role in Gamma Knife radiosurgery, working as part of a multidisciplinary team that may include neurosurgery, radiation oncology, medical physicists, and nuclear medicine specialists.
“Now, the radiologist is much more involved in the sophisticated imaging we use,” says neurosurgeon Jason Sheehan, MD, director of the UVA Gamma Knife Center. Those imaging modalities, Dr. Sheehan says, include the traditional MRI and CT used in Gamma Knife, along with PET imaging, functional MRI, and MR-based fiber tracking.
Dr. Rizvi defined five key phases of radiologist involvement:
- pre-treatment planning with MRI and CT
- target delineation
- image fusion
- treatment collaboration with neurosurgeons and physicists
- follow-up imaging to assess response.
Planning More Precise Treatments
Newer-generation Gamma Knife systems, Dr. Rizvi says, include MRI with higher spatial resolution, improved signal-to-noise ratio, and better distortion correction. “We can also use 3D isotropic sequences so we are more precise in giving the radiation, with less damage to normal tissues,” he says.
Treatment planning also incorporates functional MRI and tractography to help reduce cognitive decline and neurological deficits that can occur with radiation. “Structural imaging clearly defines the vital structures like hippocampi, brainstem, optic nerves and deep gray nuclei, the areas we need to preserve,” Dr. Rizvi says.
Embedding AI Into Workflows
AI is advancing radiosurgery treatments in several ways. AI contouring and segmentation are making procedures more efficient. “We can perform MRI sequences faster using AI,” Dr. Rizvi says. “We can also assess treatment response based upon the AI to differentiate between recurrence and radiation injury.”
In addition, Dr. Sheehan and another UVA colleague, Adam Tashman, PhD, associate professor of data science, are conducting grant-funded research into using large language models to predict stereotactic radiosurgical dosing regimens for patients with brain metastases.1
“What might be the best dose and fractionation scheme for a tumor in one patient may be slightly different in another,” Dr. Sheehan says. “We are able to use our AI model to better predict what would be appropriate treatment parameters for radiosurgery.”
Redefining Outcome Measures
Advances in radiosurgery are shifting the endpoints beyond traditional metrics, such as progression-free survival and overall survival, and toward quality-of-life and patient-reported measures.
“There are several papers published in Neuropoint Alliance [a national radiosurgery registry] showing that quality of life in patients treated with brain metastases who undergo radiosurgery is remarkably well preserved, and in some aspects, it actually improves after Gamma Knife radiosurgery,” Dr. Sheehan says.
Gamma Knife can also be used in more intricate procedures, thanks in part to higher image quality and complexity. “Previously, physicians used to refrain from giving radiation near the eloquent cortex, which controls speech,” Dr. Rizvi says. “Now, because of the precise definition, you can target those lesions without causing damage or impairing language and motor functions.”
Expanding to New Indications
Looking ahead, Drs. Sheehan and Rizvi see practical use of radiosurgery in psychiatric disorders, with groups like the International Stereotactic Radiosurgery Society already establishing guidelines for the use of Gamma Knife in treating conditions such as obsessive-compulsive disorder (OCD).2
“The ability to integrate fiber tracking and functional MRI into Gamma Knife opens up a whole new horizon for us, not just for tumors and vascular malformations, but potentially for functional disorders, including OCD, pain disorders, and potentially even depression.”3
References
- Levy I, Gorecki T, Castro B, et al. Machine Learning-Driven Prediction of Gamma Knife Treatment Parameters and Outcomes. AI in Precision Oncology. 2026;2(6):231-240. doi:10.1177/2993091X251392898
- Maroufi SF, Fallahi MS, Kotecha R, et al. Stereotactic Radiosurgery Capsulotomy for Intractable Severe Obsessive-Compulsive Disorder: A Systematic Review, Meta-Analysis, and International Stereotactic Radiosurgery Society Practice Guidelines. Neurosurgery. Published online Nov. 11, 2025. doi:10.1227/neu.0000000000003842
- Sheehan J, Trifiletti D, Keole S. Unlocking the Power of Connectomes for Image-Guided Cranial Interventions. Int J Radiat Oncol Biol Phys. 2024;119(4):1133-1136. doi:10.1016/j.ijrobp.2023.12.053


 May 04, 2026
May 04, 2026