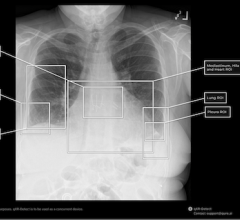
Figure 2: Pulmonary CT angiography of a 68 year old male. The CT scan was obtained 10 days after the onset of COVID-19 symptoms and on the day the patient was transferred to the intensive care unit. Axial CT images (lung windows) (a,b) show peripheral ground-glass opacities (arrow) associated with areas of consolidation in dependent portions of the lung (arrowheads). Interlobular reticulations, bronchiectasis (black arrow) and lung architectural distortion are present. Involvement of the lung volume was estimated to be between 25% and 50%. Coronal CT reformations (mediastinum windows) (c,d) show bilateral lobar and segmental pulmonary embolism (black arrows). Courtesy of RSNA
April 23, 2020 — A special report published in the journal Radiology outlines prevention, diagnosis and treatment of complications stemming from blood clots in patients with COVID-19. The journal also published two research letters and a case study on this topic.
Clinicians worldwide face this new severe infectious lung disease with no proven therapies. Based on recent reports that demonstrated a strong association between elevated D-dimer levels and poor prognosis, concerns have risen about thrombotic complications in patients with COVID-19.
The National Institute for Public Health of the Netherlands asked a group of radiology and vascular medicine experts to provide guidance for the imaging workup and treatment of these important complications. Their report summarizes evidence for thromboembolic disease and potential diagnostic and preventive actions that can be taken.
“Worldwide, COVID-19 is being treated as a primary pulmonary disease,” said Edwin J.R. van Beek, M.D., Ph.D., director at Edinburgh Imaging, Queens Medical Research Institute, at the University of Edinburgh, U.K. “From the analysis of all available current medical, laboratory and imaging data on COVID-19, it became clear that symptoms and diagnostic tests could not be explained by impaired pulmonary ventilation alone.”
Recent observations suggest that respiratory failure in COVID-19 is not driven by the development of the acute respiratory distress syndrome alone, but that microvascular thrombotic processes may play a role. This may have important consequences for the diagnostic and therapeutic management of these patients. There is a strong association between D-dimer levels, disease progression and chest CT features suggesting venous thrombosis. In addition, various studies in patients with COVID-19 have shown a very strong association between increased D-dimer levels and severe disease/poor prognosis.
The report authors stress that careful attention needs to be paid to the initial diagnosis and treatment of the prothrombotic and thrombotic state that can occur in a substantial percentage of COVID-19 patients.
“Imaging and pathological investigations confirmed the COVID-19 syndrome is a thrombo-inflammatory process that initially affects lung perfusion, but consecutively affects all organs of the body,” Professor van Beek said. “This highly thrombotic syndrome leads to macro-thrombosis and embolism. Therefore, strict thrombosis prophylaxis, close laboratory and appropriate imaging monitoring with early anti-coagulant therapy in case of suspected venous thromboembolism are indicated.”
Recommendations for diagnostic and therapeutic management, which vary based on patient symptoms and risk profiles, include prophylactic-dose heparin, chest CT, CT pulmonary angiography and routine D-dimer testing.
Findings have also emerged linking COVID-19 more specifically with pulmonary embolism. A research letter from Hôpitaux Universitaires de Strasbourg published today in Radiology reported that of 106 pulmonary CT angiograms performed for COVID-19 patients over a one-month period in a tertiary care center in France, 32 patients (30%) had acute pulmonary embolus (PE). This rate of PE is much higher than usually encountered in critically ill patients without COVID-19 infection (1.3%,) or in emergency department patients (3 to 10%). In the study, a D-dimer threshold of 2660 μg/L detected all patients with PE on chest CT.
A second research letter published today described a study from Centre Hospitalier Universitaire de Besancon in France pointed to high proportion (23%) of COVID-19 patients with contrast CT had PE. PE was diagnosed at mean of 12 days from symptom onset. Patients with PE were more likely require care in the critical care unit and to require mechanical ventilation.
Lastly, a case report from Cooper University Hospital in Camden, New Jersey, describes multiple areas of pulmonary and arterial thrombosis in an 84-year-old man with COVID-19.
“COVID-19 is more than a lung infection,” Professor van Beek said. “It affects the vasculature of the lungs and other organs and has a high thrombosis risk with acute life-threatening events that require adequate treatment with anticoagulants based on laboratory monitoring with appropriate imaging tests as required.”
For more information: www.rsna.org
Related Coronavirus Content:
VIDEO: Imaging COVID-19 With Point-of-Care Ultrasound (POCUS)
The Cardiac Implications of Novel Coronavirus
CT Provides Best Diagnosis for Novel Coronavirus (COVID-19)
Radiology Lessons for Coronavirus From the SARS and MERS Epidemics
Deployment of Health IT in China’s Fight Against the COVID-19 Epidemic
Emerging Technologies Proving Value in Chinese Coronavirus Fight
Radiologists Describe Coronavirus CT Imaging Features
Coronavirus Update from the FDA
CT Imaging of the 2019 Novel Coronavirus (2019-nCoV) Pneumonia
CT Imaging Features of 2019 Novel Coronavirus (2019-nCoV)
Chest CT Findings of Patients Infected With Novel Coronavirus 2019-nCoV Pneumonia
Find more related clinical content Coronavirus (COVID-19)
ACC COVID-19 recommendations for the cardiovascular care team
VIDEO: What Cardiologists Need to Know about COVID-19 — Interview with Thomas Maddox, M.D.
The Cardiac Implications of Novel Coronavirus
ESC Council on Hypertension Says ACE-I and ARBs Do Not Increase COVID-19 Mortality


 May 08, 2026
May 08, 2026