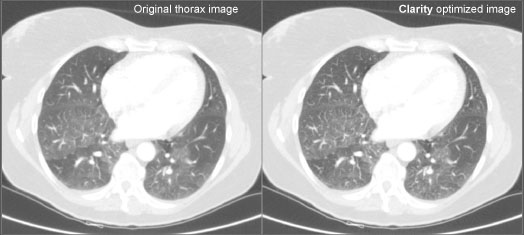
A comparison of the original and Clarity-enhanced CT image from Philips Brilliance 64, showing a 3 mm contrast-enhanced thorax slice at 133 mAs, 120 KVP.
In an effort to lower the radiation doses patients receive from CT scans, Unilabs Röntgen Majorstuen in Oslo, Norway, installed dose-lowering enhancement software on a trial basis between May and November 2008. In selected cases of thoracic CT, the hospital was able to reduce up to 70 percent of the dose as compared to full-dose examinations.
The facility used the Clarity CT Solution software made by Saphenia. The system was connected to the facility’s Philips Brilliance 64 CT and Siemens PACS. Data acquired from the scanner were reconstructed on the scanner before post-processing on the Clarity server. From there DICOM images were transferred to the PACS and Philips workstation. In addition, unprocessed raw data was transferred to the workstation for comparison and secondary reconstruction purposes.
Unilabs chose only to implement the system for low-dose noncontrast thoracic CT examinations during the trial period. Indications for referral included dyspnea, chest pain, possible pneumonia, suspected interstitial lung disease, and skeletal abnormalities or possible finding on a chest X-ray.
There were 35 patients examined under these criteria. Most underwent noncontrast, low-dose CT from the jugulum to the diaphragm at 120 kV, 80 mA. In the last 16 patients the dose was further reduced by lowering mA by an average of 20 percent, some as low as 30 mA. In addition the radiologists included a control group of 10 patients who, for various reasons, had to undergo a full-dose CT of the chest. The images were reconstructed in 3/2 before transfer to the Clarity server.
The series of images were examined by one of the three staff radiologists and reported as any other CT scan. Image quality and clinical value were also evaluated.
The mean radiation dose in the 35 low-dose patients was 2.41 mSv. The mean dose in the 10 full-dose patients was 5.29 mSv, while the national average dose in Norway is 10 mSv (1). Use of the software contributed to a 53.3 percent and 74.1 percent reduction respectively. If only the last 16 patients were considered, the average dose was 1.55 mSv. This translates into an 84 percent reduction from average dose for Norway and a 70 percent reduction from Unilabs’ average full-dose scans. Image quality and diagnostic value was considered good or very good by all reporting radiologists.
For more information: www.claritysolutions.org, www.unilabs.no


 May 19, 2026
May 19, 2026 









