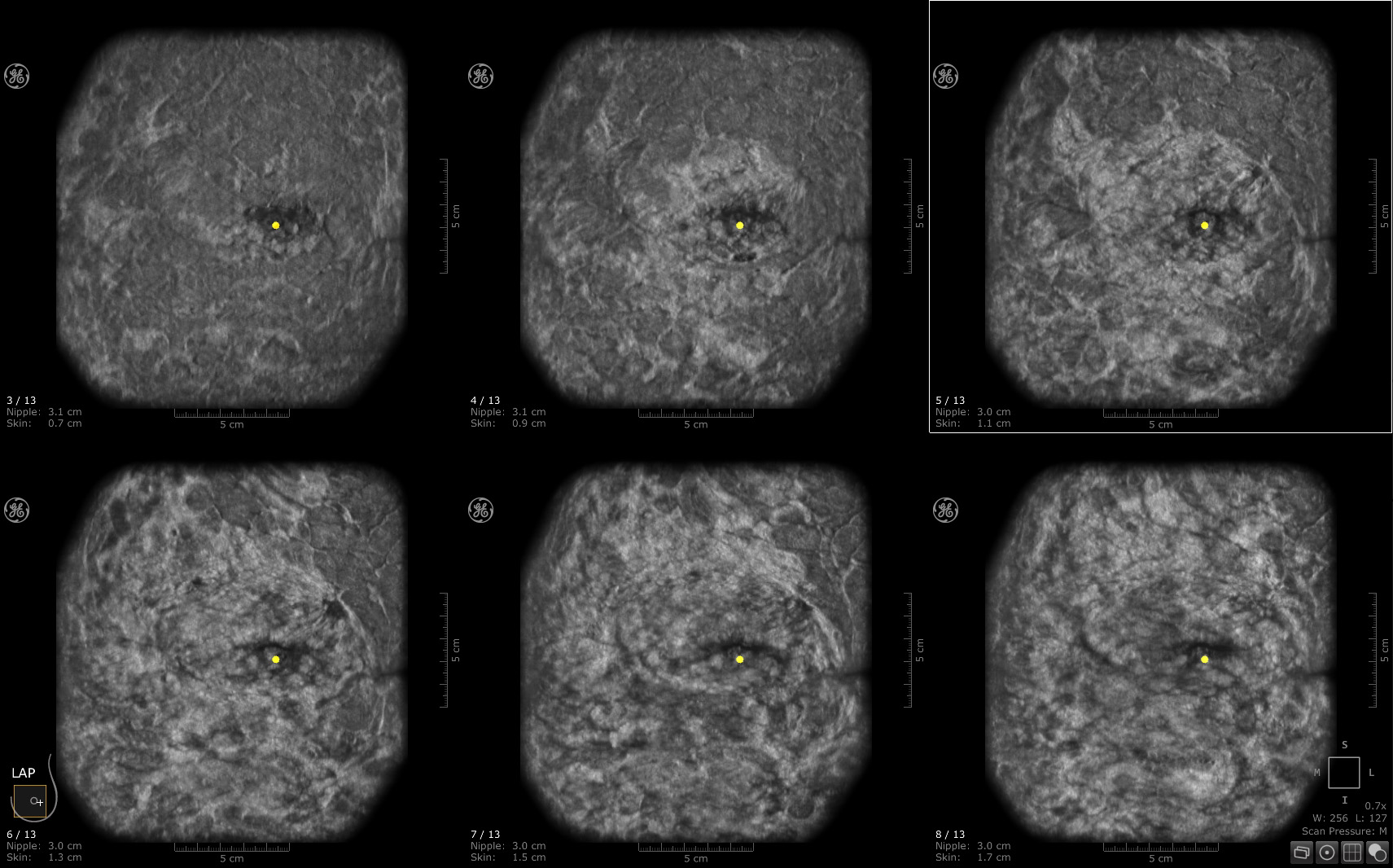
In a detailed overview held during the Radiological Society of North America’s (RSNA) 2021 annual meeting, promising results from an Institutional Review Board (IRB)-approved study were presented by Georgia Giakoumis Spear, MD. She serves as chief of the department of breast imaging with NorthShore University HealthSystem, and is an associate professor of radiology at the University of Chicago Pritzker School of Medicine.
NorthShore University HealthSystem includes four hospital-based full-service comprehensive breast centers and five satellite imaging centers. A teaching affiliate at the University of Chicago, it has 14 board certified radiologists specializing in breast imaging. The high-risk breast clinic, part of the Kellogg Comprehensive Cancer Center, provides 95,000 screening mammograms yearly, and physicians perform all diagnostic ultrasounds.
In the session, Spear, who uses the GE Invenia ABUS 2.0 system, shared the benefits of adding whole breast automated ultrasound (ABUS) screening to clinical practice, enhancing cancer detection in dense breast tissue. Featuring case-based review, the presentation included strategies for successful implementation and interpretation.
QView Medical and GE Healthcare announced, in November 2021, that QView’s QVCAD software can be launched on GE Healthcare’s Invenia ABUS 2.0, the first FDA-approved ultrasound supplemental breast screening technology specifically designed for detecting cancer in dense breast tissue.
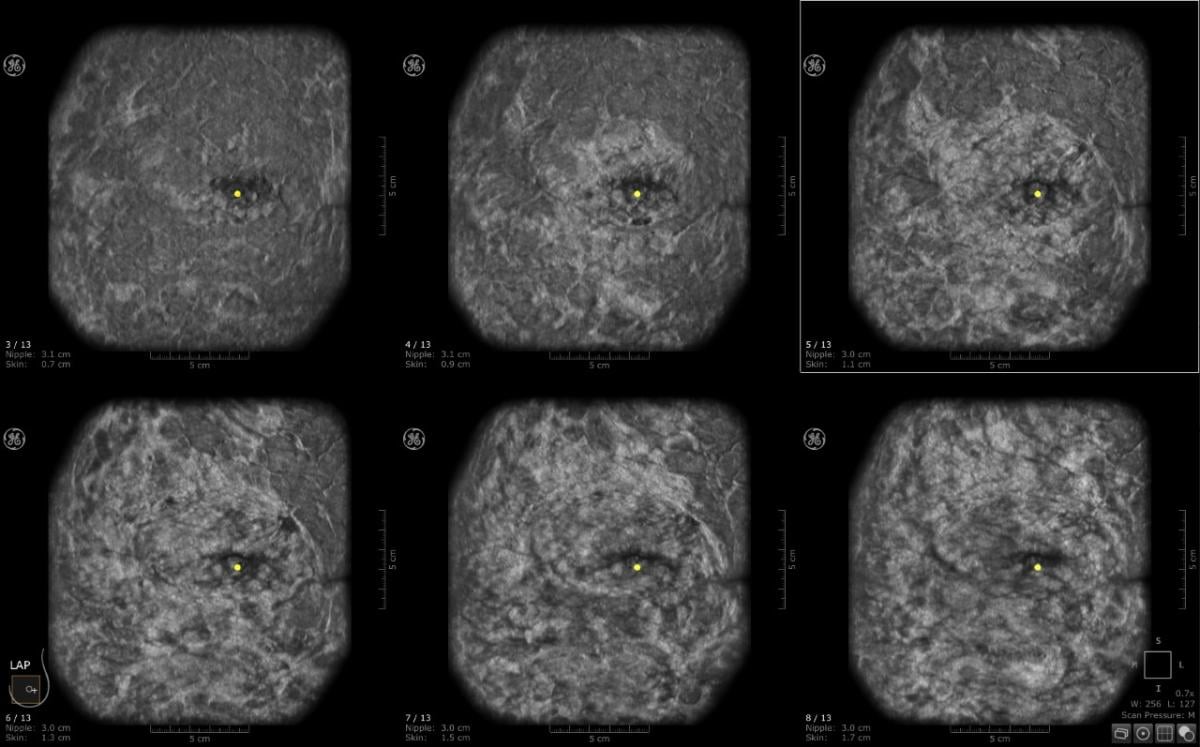
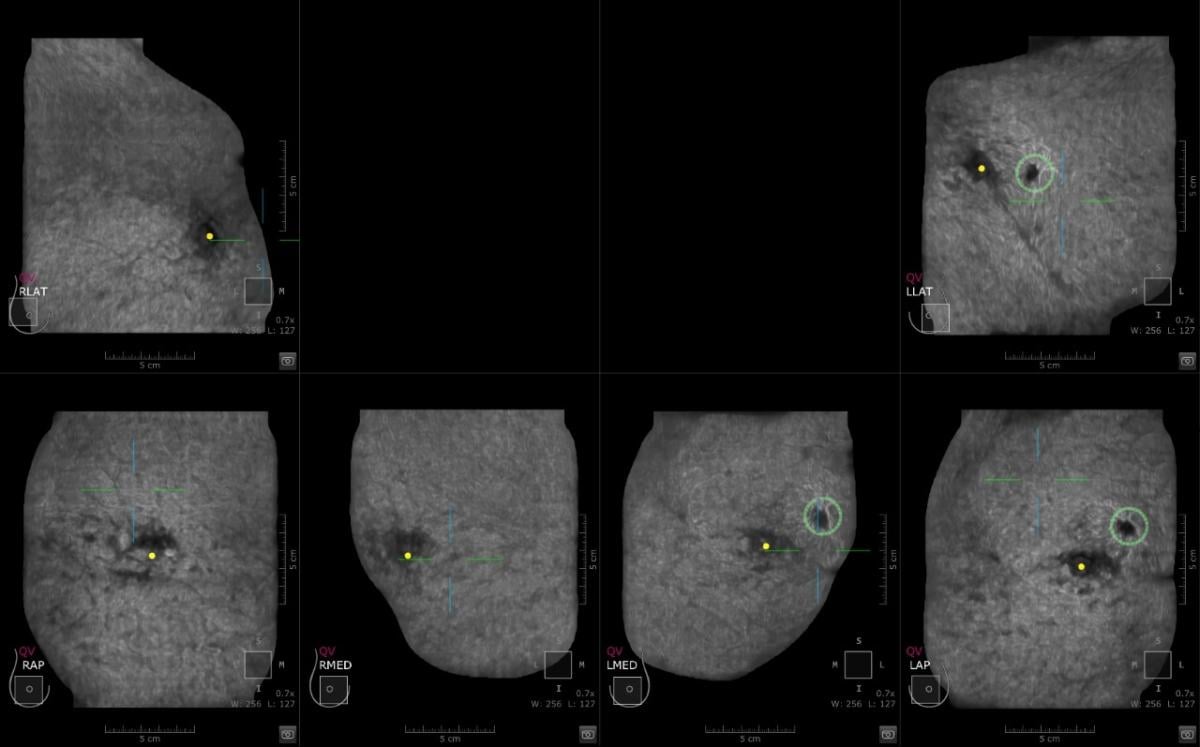
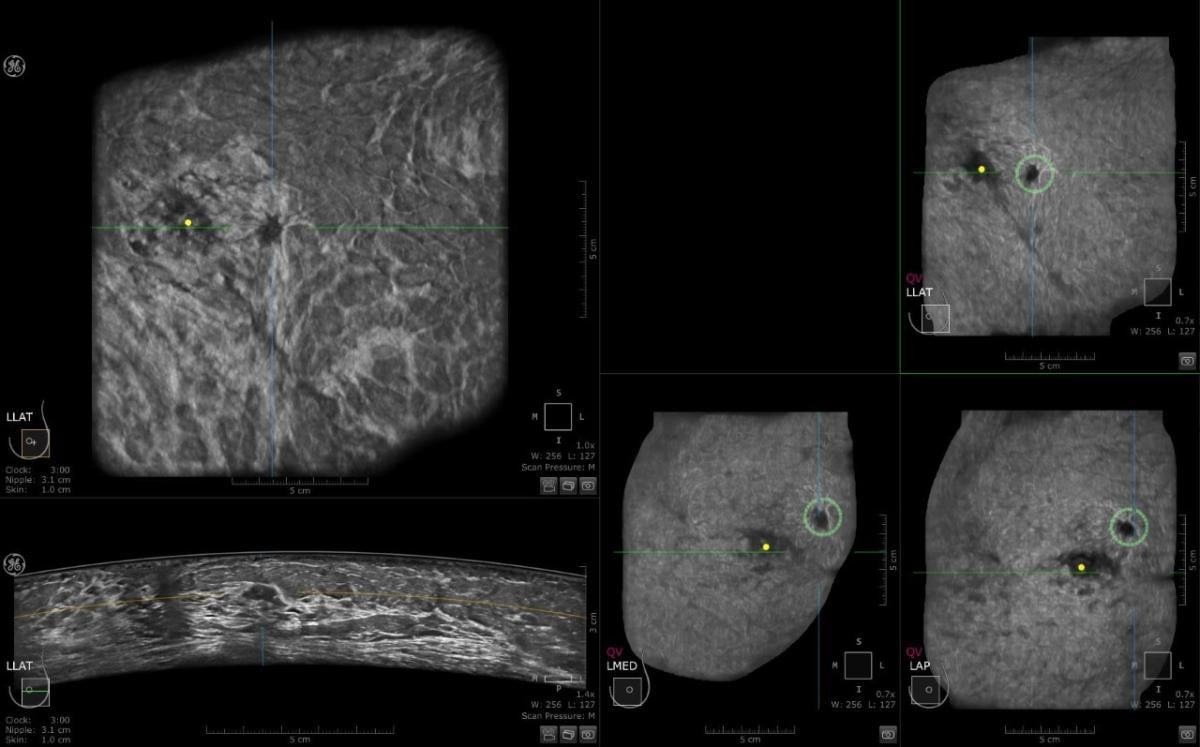
This is a case where CAD detected an abnormality in the left breast and the margins are irregular. Multiview display. QView CAD detection integrated in the ABUS. Bilateral breast ABUS display with the pink indicator indicating that QView CAD is processed. Image courtesy of Georgia Giakoumis Spear, MD
ABUS: Why and How We Use It
In providing an overview of ABUS, its uses and benefits, and the clinical study, Spear offered reasons why ABUS is a valuable solution for central screening with breast tissue. She noted that breast density limits the ability to detect breast cancer, which can impact a woman’s risk 4-6 fold. She applauded progress with mandatory breast density legislation, noting that, as of 2021, a total of 38 states and DC are following legislation, and 8 have supplemental screening reimbursement legislation, reflective of an Increased demand for supplemental screening.
“The onus is on us to find those cancers,” stated Spear. Speaking to the effectiveness of the new technology available, she added, “You can’t help but make believers of these advances (in reference to QView’s CAD technology), because we are finding things that we’d not seen before.”
In an overview of the NorthShore University HealthSystem Retrospective IRB-approved Study, she noted that this was a study of the first 500 patients who underwent ABUS for supplemental screening. Results included 6 small, invasive, node-negative, clinically significant breast cancers detected (CDR 12/1,000); a low call back rate of <10%, and a 55% high positive biopsy rate. She noted that this was a 3-year prospective clinical trial, recently completed, compiling of data ongoing. The high CDR and low recall rates were attributed to four factors:
• Facility with ultrasound in the practice;
• incidence vs. prevalence screens;
• image quality optimization; and
• interpretation strategies.
Referrals came from their own radiologists and technicians; the high-risk breast clinic; breast surgery department; and referring physicians.
Eligibility criteria was as follows:
•Patients with BI-RADS density
categories C&D;
•difficult clinical examination; and
•current mammogram (within 9 months).
At NorthShore University HealthSystem, Spear and her colleagues work with the QView CAD application, which can be accessed through the Invenia ABUS 2.0 Viewer software from GE Healthcare. Spear shared detailed and promising outcomes she has experienced in the implementation process, noting that computer assistance detected abnormalities that may not have been caught initially. AI allows for analysis of hundreds of images and presents them in a single page via the QView CAS Navigator Image (3D map).
When AI was integrated into the reading workflow, in a review of 2,000 images with the QView CAD system, the results included a 33% reading time improvement, and a 93% sensitivity with 0.1 FPR per volume.
“You cannot help but make believers of people by showing these results,” she noted, adding, “This will help us improve both efficiency and success, offering wonderful specificity and sensitivity for new and experienced users.” She said this will help the radiologist look at three mammograms and add supplemental modality with thousands of images. Her experiences have led her to be a firm believer in the value of ABUS systems as an important element in busy practices, and is aware that having “distortions and lesions pop” is a benefit to radiologists and patients.
Clinical Implementation of ABUS
Spear addressed the practical benefits to radiology teams and summarized how the implementation process evolved for their team.
“There are many advantages on the horizon, especially given our increasingly busy practices, which often have us viewing 150-200 exams/day,” said Spear.
“Optimal input necessary for optimal output,” she added, reinforcing that “Image quality optimization was the key factor in successful interpretation.” Spear addressed the success factors for ABUS implementation include a team approach, communication, focusing on education, training, knowledge of displays, and strategies for interpretation. Here, then, an abridged summary of her presentation:
“We looked into automated ultrasound technology as we noticed the prevalence of dense breast tissue. In November 2015, we started performing this with two ABUS units, and now have 9 total, as we have found it to be both a physician satisfier and a patient satisfier. As an ultrasound facility, we wanted to learn why detection was high and call back rate was low.
“When we implemented automated ultrasound, we identified the patients who would most benefit … the goal was to reduce false positives and look for the cancer that they may have missed with just mammography.
“It was determined that the mammogram and automated breast ultrasound should both be done on the same day,” said Spear, who offered multiple benefits in doing so:
•Target areas of subtle mammographic question, focusing on same area in >2,000 ultrasound images.
•Combined assessment may minimize false positives on both studies and may increase combined accuracy of both exams.
•Eliminate need for callback from mammogram (i.e. new mammographic mass may be explained by cyst on same day ABUS).
Spear shared the top issues radiology teams need to consider with a new modality to establish success:
•Understanding physician staffing
• Technologist proficiency
• IT integration is crucial (large storage capacity is essential)
•Scheduling appropriate times and throughput in dept
•Coordination of interpretation
•Training with standardized protocols in small groups
“We are interpreting with the intention to find more cancers, which will help them be more successful,” said Spear. “Handheld and automated have major differences, whereby automation allows viewing of the coronal plane, which is critical for success.”
Spear listed some advantages of automated ultrasound over handheld ultrasound:
•Reproducibility and consistency
•Easy to perform, does not require physician time to perform
•Consistent image acquisition time
•Reduces expected delays, allows streamlined workflow
•Physician time for interpretations decreases with experience
•Post processing advantages
•Coronal views helpful in detecting architectural distortion
•Sharper images
•Large area of coverage
ABUS Scanning and the Benefits of the Unique Coronal Plane
Spear discussed that this acts as a roadmap for evaluation of the breast and allows for anatomic consistency. It also shows a breast’s radial anatomic arrangement, and the wide footprint allows for longer area of breast tissue coverage with one scanning motion. Extended field of view allows for evaluation of multiple findings and larger area of tissue surrounding a lesion, and offers enhanced visualization of architectural distortion and multiple masses. She stated that it was a different than routine HHUS imaging — the coronal plane allows for anatomic depiction of whole breast from skin to chest wall.
She addressed specific components radiologists need to look for with the coronal plane. Her recommendations include: Alterations in the tissue: dark/black holes; Identify masses, architectural distortion, spiculation — lesion analysis; look at surrounding tissue (echogenicity, desmoplastic reaction); and spiculation/retraction similar to that seen on 2D and DBT mammography. She also noted the multi-slice coronal view being used more regularly in her practice, as they continue looking at anatomy and identifying abnormalities.
Is there a role for AI in successful implementation? She believes there is. Spear contends that AI tools can assist radiologists in multiple ways, from increased productivity, to allowing radiologists to focus on potential areas of interest quicker. She added that AI can impact one’s accuracy potentially as AI algorithms have high sensitivity.
“Relying on AI is a good thing to do to balance the quality of interpretation and cancer detection,” noted Spear.
She identified four primary benefits of AI in discussing its role in successful implementation. AI tools assist the radiologist first and foremost, she noted. It increases productivity by allowing a view of the entire case at-a-glance; third, users are drawn to focus attention on potential areas of interest, which leads to increased confidence; and lastly, accuracy, as AI algorithms detect and mark easy-to-miss lesions and oversights with high sensitivity.
“We are always asking what we can do to improve efficiency and success,” said Spear, reporting that “The specificity is wonderful, and new users and experienced users can both benefit.” Noting how increased volumes of screenings lead to reader fatigue, she reinforced the benefit that this helps radiologists hone in on abnormalities, and provide a confidence boost on imaging so radiologists can readily work through images for better outcomes.
“Our experience with automated ultrasound drove our understanding of strategies for success,” said Spear in her closing comments.
She outlined that AUS implementation strategies rely on workflow planning/IT, integration/scheduling, and an emphasis on small group training. AUS interpretation strategies rely upon high quality imaging, optimizing software utilization, understanding AUS technology and particularly understanding the role of the coronal plane, and reduction of false positives. “As we see it, AI is a crucial part of the future of our practices,” stated Spear.
“With such busy practices, we understand that any implementation of any modality will have initial uphill challenges, but it is always about adding value as you move through. In general, as physicians and radiologists we get comfortable in our environment, so change can be hard. We picked four people at the start and had successful results. After we reiterated interpretation strategies, we were finding things we had not before seen. Three-dimensional was an advantage, and we already knew that. It is a matter of human nature, but one must be persistent. It was important to start slow, and to have a physician to champion the program. QView CAD is a recent addition to the practice, and now that it is integrated with ABUS workstations, we are working to disseminate it across the board.”
Recounting an experience that impacted her, she shared one instance where she had worked with one woman from the start of her diagnosis. Noting how rare it is to get feedback, she recalled that after treatment and recovery, the patient came to her practice and gave her a clock, to thank Spear for giving her back the gift of her time.
“This helps propel you to find new and better ways of doing things and improving
the status quo,” concluded Spear.
Related ABUS content:
Driving the Adoption of ABUS With AI Technology
QView Medical Showcases QVCAD for ABUS Exams at RSNA 2018
Artificial Intelligence Helps Detect Breast Cancer and Saves Time
FDA Proposes New Rules for Mammography Reporting and Quality Improvement


 May 22, 2026
May 22, 2026 









