January 15, 2016 — A regional anesthesia technique called thoracic paravertebral nerve block (TPVB) is highly effective in controlling pain after breast cancer surgery, but concern about potential complications may limit its use. A new study provides evidence that using ultrasound to guide the nerve blocking procedure lowers the risk of complications, reports a study in Anesthesia & Analgesia.
In particular, ultrasound-guided nerve blocking avoids potentially serious complications related to inadvertent puncture of the tissue lining the lungs (pleura), according to the report by Peter Stefanovich, M.D., and colleagues at Massachusetts General Hospital.
The researchers analyzed their experience with this nerve blocking in 856 women undergoing mastectomy from 2010 through 2013. In this procedure, a small amount of local anesthetic is injected around the thoracic nerve roots where they emerge from the spinal cord. This numbs the entire area of the chest, on one or both sides (if the nerves on both sides of the spinal cord are injected).
This regional nerve block provides excellent control of pain after breast cancer surgery. That's especially important because pain in the immediate postoperative period is a major risk factor for the development of chronic pain in women who have undergone mastectomy.
However, this nerve blocking isn't performed as often as it might be because of patient safety concerns—especially the risk of puncturing the pleura due to incorrect needle placement. This can lead to a serious complication called pneumothorax, where air enters the chest cavity, potentially causing collapse of the lung.
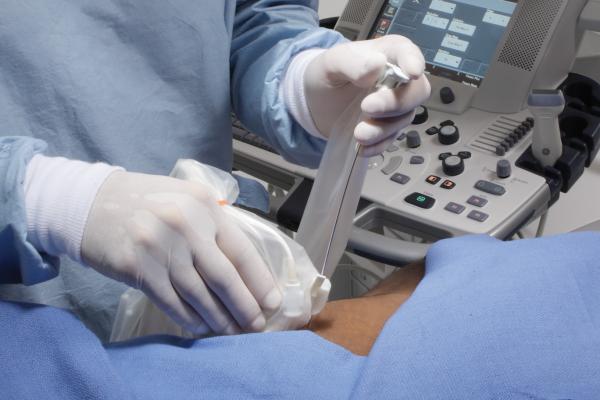
Stefanovich and colleagues analyzed their experience with ultrasound guidance to make this nerve blocking safer. Using ultrasound, the anesthesiologists performing nerve blocking were able to visualize the exact location of the thoracic spinal nerve roots. Ultrasound was used in addition to the conventional approach, using anatomical landmarks to guide the injection.
Following this procedure, anesthesiologists were able to confirm correct needle placement before injecting the local anesthetic. In the experience of more than 14,000 thoracic spinal nerve injections, there were no pleural punctures and no cases of pneumothorax.
Major complications related to this nerve blocking placement developed in six patients—a rate of 0.7 percent. Four patients had drops in blood pressure and heart rate, while two had suspected toxic effects of the local anesthetic used for the procedure.
Previous reports have suggested that performing this nerve block under ultrasound guidance might make the procedure safer. The new study is the first to provide evidence that ultrasound-guided nerve blocking lowers the risks of pleural puncture and pneumothorax.
"Avoidance of these complications may be a consequence of improved safety using real-time visualization and imaging of the pleura with ultrasound," Stefanovich and coauthors write. They hope their experience will encourage other hospitals to offer this highly effective regional anesthesia technique—potentially reducing the common and difficult-to-treat problem of chronic pain after mastectomy.
"Thoracic paravertebral nerve block is a technique that many consider to be high risk," commented Steven L. Shafer, M.D., of Stanford University, editor-in-chief of Anesthesia & Analgesia. "This study provides convincing evidence that, with ultrasound guidance and in experienced hands, TPVB is not a high-risk procedure."
For more information: www.iars.org


 May 27, 2026
May 27, 2026 









