November 20, 2008 - With the most recent release of data from the National Oncologic PET Registry (NOPR), researchers may have reached the moment of critical mass by confirming the effectiveness of positron emission tomography (PET) in the monitoring of tumor activity across a wide range of cancers.
“During the first year of the study, we verified that PET finds more areas of active cancer than other imaging tools and leads, in some cases, to earlier initiation of subsequent treatment,” said Bruce E. Hillner, M.D., professor of medicine at Virginia Commonwealth University in Richmond, Va., and lead author of the article. “We noted that PET has a clinically significant impact on cancer management, resulting in a change in treatment in more than one out of three cases—or 36 percent of the time.”
In the article, published in the December issue of The Journal of Nuclear Medicine, researchers reported results by cancer type for the first two years of data collected from nearly 41,000 PET studies conducted at more than 1,300 cancer centers nationwide. Analysis was restricted to the use of PET for staging, restaging or detection of suspected recurrences in patients with pathologically proven cancers.
Study data released in March 2008 showed a striking consistency of the impact of PET on referring physicians’ intended management plans. At that time, NOPR researchers felt that the significance of the evidence was such that they formally asked the Centers for Medicare and Medicaid Services (CMS) to reconsider the current National Coverage Determination on oncologic use of PET.
“As a result of the data, the follow-up question for the second year was: Does the impact of PET vary between cancers?” explained Hillner. “We found that it did not vary significantly, and that changes in treatment plans for rare cancers—such as stomach cancer—clustered around the same one-third mark as the more common cancers. As a result, we believe that coverage for PET in the staging, restaging and detection of recurrence of cancer should be handled the same across the board.”
According to the researchers, a substantial body of national and international literature now exists showing that PET is a highly effective technique for imaging cancer.
“From the data, we concluded that, although the effectiveness of PET may differ somewhat between individual cancers, it's in the same ballpark,” said Barry A. Siegel, M.D., professor of radiology at Mallinckrodt Institute of Radiology in St. Louis, Mo., and one of the co-authors of the article. “This result was a little unexpected, but leads us to believe that a continual parsing of PET’s usefulness, cancer by cancer and indication by indication, for purposes of reimbursement does not make clinical sense.”
The NOPR was launched in 2006 in response to a proposal from CMS to expand coverage for PET to include cancers and indications not presently eligible for reimbursement, including cancers of the ovary, uterus, prostate, pancreas, stomach, kidney and bladder.
“The NOPR has been a collaborative process with CMS,” said Siegel. “The purpose of our partnership has been to get the best data into the public domain for decision-making. We are hopeful that a decade-long process leading to an understanding of the usefulness of PET in cancer management is finally completed.”
A draft decision by CMS is expected on Jan. 10, 2009. Following a 30-day comment period, the final National Coverage Determination will be made April 9.
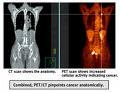
PET imaging, also called PET scanning, is a procedure that images the function of cells to show differences between healthy tissue and diseased tissue. It is used to evaluate various neurological and cardiac disorders as well as for diagnosing, staging and monitoring the treatment of many different cancers.
Coauthors of “Relationship of Cancer Type and the Impact of PET and PET/CT on Intended Patient Management: Findings of the National Oncologic PET Registry” include Bruce E. Hillner, department of internal medicine and Massey Cancer Center, Virginia Commonwealth University, Richmond, Va.; Barry A. Siegel, division of nuclear medicine, Mallinckrodt Institute of Radiology and Siteman Cancer Center, School of Medicine, Washington University, St. Louis, Mo.; Anthony F. Shields, Karmanos Cancer Institute, Wayne State University, Detroit, Mich.; Dawei Liu, Ilana F. Gareen and Ed Hunt, Center for Statistical Sciences, Brown University, Providence, R.I.; and R. Edward Coleman, department of radiology, School of Medicine, Duke University, Durham, N.C.
For more information: www.snm.org


 May 27, 2026
May 27, 2026