June 21, 2023 — Fresenius Kabi, a leading provider of injectable medicines, announced today it has launched the ...
Molecular Imaging
Nuclear imaging, also called molecular imaging, includes positron emission computed tomography (PET) and single photon emission computed tomography (SPECT) imaging. This section includes radiopharmaceuticals and tracers, PET-CT, SPECT-CT, and PET-MRI. Molecular imaging includes the field of nuclear medicine, which uses very small amounts of radioactive materials, or radiopharmaceuticals, to diagnose and treat disease.
June 19, 2023 — NorthStar Medical Technologies, LLC, a global innovator in the development, production and ...
June 15, 2023 — With immunotherapy emerging as one of the most important treatment options in oncology, GE HealthCare ...
Technological advancements in positron emission tomography/computed tomography (PET/CT) offer both clinicians and ...
June 14, 2023 — A University of Waterloo engineer’s MRI invention reveals better than many existing imaging technologies ...
May 25, 2023 — GE HealthCare, a leader in breast cancer care technology and diagnostics, has today announced that NCCN ...
May 16, 2023 — The American Society for Radiation Oncology (ASTRO) today expressed its strong support for President ...
Efficiency and effectiveness are inseparable in clinical medicine. Digital PET addresses them both. The key is the ...
May 16, 2023 — Bracco Imaging, an innovative world leader delivering end-to-end products and solutions through a ...
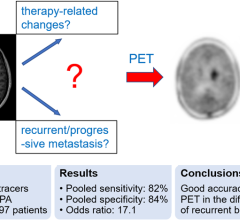
May 12, 2023 — A newly published meta-analysis indicates that amino acid PET can accurately differentiate recurrent or ...
May 1, 2023 — Prelude Corporation (PreludeDx), a leader in molecular diagnostics and precision medicine for early-stage ...
Introducing HYPERSCAN , Pencil Beam Scanning Delivery HYPERSCAN enables tumor volumes to be scanned in a matter of ...
April 24, 2023 — NorthStar Medical Radioisotopes, LLC, a global innovator in the development, production and ...
April 13, 2023 —NorthStar Medical Radioisotopes, LLC, a global innovator in the development, production and ...
April 5, 2023 — RaySearch Laboratories AB announced that the number of clinics in the world that have bought RayStation ...
April 3, 2023 — NorthStar Medical Radioisotopes, LLC, a global innovator in the development, production and ...
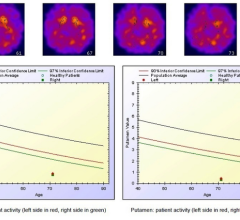
March 29, 2023 — A newly published literature review sheds light on how nuclear medicine brain imaging can help evaluate ...
March 29, 2023 — Ratio Therapeutics Inc., a pharmaceutical company that employs a suite of innovative technologies to ...
March 28, 2023 — A new article in The Journal of Nuclear Medicine explores the potential for using ChatGPT, an ...
March 27, 2023 — On Target Laboratories, Inc., a privately held biotechnology company developing intraoperative ...
March 22, 2023 — A novel imaging modality that can visualize the distribution of medical radiopharmaceuticals with very ...
March 21, 2023 — Positron Corporation, a molecular imaging device company that offers PET imaging systems and clinical ...
March 20, 2023 — RayzeBio, Inc., a targeted radiopharmaceutical company developing an innovative pipeline against ...


 June 21, 2023
June 21, 2023