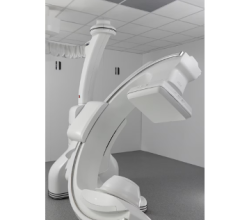
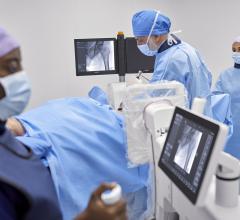
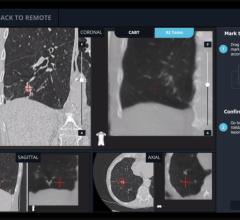
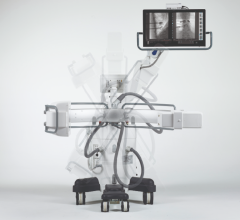
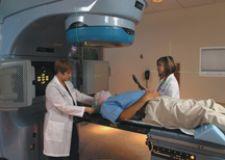
Lisa Bailey, R.T.T, and Angie Daws, R.T.T, set up a patient on a Varian Trilogy with On-Board Imager.
When you hear a name like The Emory Clinic Department of Radiation Oncology you undoubtedly conjure up visions of a top-notch, well-equipped outpatient cancer treatment center funded by generous private, public and collegiate benefactors that offset payer reimbursement woes.
And you’d be half right. Department administrator Diane Cassels, M.S., R.T.T., CMPE, can only wish for half of that to be true – the latter half. Being hitched to a widely respected university and medical school, and a nationally recognized hospital, admittedly affords certain privileges. But fat checks or even blank checks are not one of them.
“Technically, we operate as a freestanding facility so we don’t receive funding by the hospital or the university,” Cassels told Outpatient Care Technology (OPCT). “We have to compete for dollars just like everyone else.”
In fact, The Emory Clinic’s radiation oncology department remains “totally self-sufficient,” supporting its high-tech equipment repertoire and extensive programs through growing patient volume and savvy invoice and reimbursement management. In addition, Emory strives to be an early adopter and implementer of new technology, serving as a clinical evaluation site for new applications offered by vendors.
For these reasons, as well as the facility’s steadfast dedication to quality patient care and high patient satisfaction, OPCT bestowed The Emory Clinic’s Department of Radiation Oncology with its inaugural 2006 Outpatient Excellence Award for Oncology Centers.
Fiscal Fruits
Launched in November 1991, the Clinic’s radiation oncology department consistently has exceeded its net income projections due to growth in gross billings and net patient services revenue each successive year, according to Cassels. And they achieved this without increasing the actual fees billed to patients. How? New CPT codes for both Intensity Modulated Radiation Therapy (IMRT) and Image Guided Radiation Therapy (IGRT), in part fueled the Clinic’s financial growth, helping it to maximize revenue.
“The new reimbursement codes for IMRT and IGRT have helped to increase revenues greatly,” she said.
Approximately 60 percent of its patients undergo IMRT for head and neck cancers, prostate, breast and CNS tumors, a key focus of the department, she noted. Moreover, this past year the department embarked on a targeted marketing campaign with advertisements strategically placed in such publications as Delta Sky Magazine and Southern Living. The purpose of these ads was two-fold, Cassels noted: Increase awareness of radiation therapy as a treatment option and increase market share of those patients selecting radiation therapy.
As a result, the Clinic’s net patient revenue is projected to be $17 million this year, and they’re now billing 10 times what they were when they opened their doors.
While growing the top line billings by approximately 20 percent during the past 12 months, the Clinic also works each invoice and denial from the insurers to optimize revenue, according to Cassels. She admitted that their invoice and denial process is no longer as labor intensive as it was in the past. “We have three certified coders,” she said. “We invested in the right people to do the right thing, and they keep up-to-date on developments. We all do. We don’t always have all the answers but we have to keep abreast of changes.”
The Clinic’s hard-earned financial results has made it easier to continue donating three percent of its net income to “Charity Care” patients that have no means to pay for treatment costs, she said. “We’re a primary provider for pediatrics,” she added, “and there are a lot of uninsured children.”
Tech Effect
Despite the fiscal growth of the Clinic’s radiation oncology department the primary element that typically drains the coffers is technology. Compounding the hurdle for the Clinic is that it’s an early adopter, “led by a strong team of radiation oncologists, physicists and radiation therapists” that are technology-minded, according to Cassels.
“We’re the first to acquire, install and implement new technology,” said Timothy Fox, Ph.D., director of Medical Physics and Computational Research and Informatics. Certain challenges accompany that claim.
“Because we’re an early adopter we don’t generate [a return on investment] right away,” Cassels said. “When we adopted new technology for the first few years we didn’t bill for it. So we had to offset expenses by offering other services and increasing patient volume. New technology has really driven our costs. That’s why we’re so glad that volume has grown because it offsets those expenses.
“We’re learning to be ahead of the curve but we’re not waiting for the curve to catch up to us,” she added.
The radiation oncology department’s tech savvy appears second to none. They were the first to implement Varian’s Trilogy system for intracranial and extracranial radiosurgery and earlier this year they added a second unit. They were the first in the U.S. to clinically use Varian’s On-Board Imaging technology, which relies on KV images to assure reproducibility of the treatment area on a daily basis. In fact, within their network of facilities they employ five OBI systems. Emory’s network includes two owned facilities that are adjacent to hospitals in the Emory Healthcare System and two other facilities where their doctors practice medicine. The main Clifton Road campus resides next to Emory University Hospital and Egleston Children’s Hospital; the second facility is five miles away next to Crawford Long Hospital in midtown Atlanta. The Clinic’s other partners are Veterans Affairs Medical Center and Grady Memorial Hospital.
“We have a [wide-area network] set up with centralized services for treatment planning, IMRT and linac all done out of that server,” Fox said. It’s a cost-effective solution for them because they don’t have to maintain software, and we can do remote-based treatment planning from our own database.” All four facilities are within a few miles of one another.
“It gives us a larger population to do clinical studies,” Cassels said. “We’ve been working together for years and have expanded our networking capabilities.”
The Clinic also implemented the first integrated computed tomography (CT) scanner and 3-D treatment planning system in Georgia and offers such high-tech-driven services as stereotactic radiosurgery and fractionated stereotactic radiotherapy for brain tumors, radioactive seed implants for prostate cancer, high-dose-rate afterloading treatment for lung, gynecologic and other cancers, IMRT, IGRT and respiratory gating for more accurate treatment delivery.
In fact, they’ve been offering IMRT for eight years. Fox recalled how hard it was back then. “We had a handful of patients in 1998, and it was so labor-intensive, in terms of the planning,” he said. “But within two years we became more efficient at it and now it’s easier on the whole team to implement, including the physicists, dosimetrists and doctors. They can localize the tumor and provide a daily dose [of radiation.]”
The Clinic also works with selected vendors by serving as a clinical evaluation site for new applications. With each new development, there is a learning curve for everyone involved, Cassels noted. They hold weekly meetings, while the department evaluates new equipment or software to assure that everything is working smoothly and any “bugs” can be reported back to the engineers.
The staff, particularly the radiation therapists, welcome and embrace new technology with enthusiasm, Cassels said. “Over the past several years the mantra has become ‘what are we doing next?’” she added.
“They’re bored if they’re not doing anything new,” Fox indicated.
Tech Trekkers
With such an extensive repertoire of new and existing equipment something is bound to go wrong but Cassels, Fox and the rest of the radiation oncology team at the Clinic aren’t worried. They rely on the efforts of Russ Olsen, clinical systems manager, as well as another full-time radiation oncology engineer, to minimize, if not prevent, downtime. They’re what Cassels call the Clinic’s “first line of defense,” followed by their primary vendor, Varian.
“Keeping two people well-trained on hand has been a good investment for us,” Cassels admitted.
Olsen, who’s certified and trained on Varian’s hardware and software, not only is in charge of maintaining the department’s equipment but also the computer network of the four integrated facilities, which includes more than 100 users on one database. Given that the department has more than doubled in size to more than 26,000 square feet from 12,500 square feet, and they handled more than 25,000 patient visits in the 12 months (roughly a 10 percent annual increase) Olsen’s job is anything but a walk in the park. He’s responsible for overseeing five linacs, one CT simulator, two acuity simulators and one HDR unit among the two Emory facilities alone, as well as coordinating new equipment installations and software upgrades.
The Clinic hired Olsen as its technology point man from the consulting firm with whom they originally contracted for service.
His mettle was tested during the recent installation of the Clinic’s second Trilogy unit. As with any new installation plans must be developed for redesigning the existing space, installing the equipment and solving problems when something unexpectedly goes wrong.
Under Olsen’s oversight, plans were made well in advance to remove an existing linac, renovate the rooms to make modifications for shielding, and installing the equipment, according to Cassels. “This was all accomplished on time with the first patients treated on this unit within a four-month time span,” she noted.
Contractors literally had to open a hatch, remove an exam room and install a new one simultaneously, Fox said. All the jackhammering was accomplished at night and on weekends. Olsen coordinated and orchestrated the schedules of the contractors and vendors to make sure everyone was ready when needed, he continued. “He’s like a referee,” he added. “We don’t see him a lot because a lot of what he does is after hours. Sometimes we take it for granted but he’s the type of person who takes ownership of things. It’s all about teamwork. If you don’t do your job you feel like you’re letting everyone else down. Our whole staff embraces this philosophy.
“When our computers go down it’s like shutting off the electricity,” Fox noted. “When you invest in such high-tech equipment it only makes sense to invest in a high-tech person to keep it running smoothly.”
The Clinic also relies on Varian, its primary equipment supplier, for tech support as a backup to prevent delays.
“One of the advantages of going with single source is that there’s not a lot of finger pointing [when something goes wrong],” Cassels said. “Another advantage is the integration and maintenance and operations of equipment.”
Fox agreed. “We went to Varian because we felt it was the best out there,” he said. “It’s easier from a service management standpoint, but we do look at quality and efficiency across the board at other vendors and consider them.”
Confirmed Cassels: “We certainly wouldn’t exclude other vendors. We want to work with the best vendor and not just one. Varian has to keep proving themselves to us. We push them, too. We also do site visits for Varian. People come in from around the world.” In fact, the Clinic is assisting Georgia’s minister of health – that’s the nation of Georgia, formerly a Soviet republic – improve healthcare delivery. One of Emory’s doctors hails from the capital city of Tbilisi.
Atop the Pyramid
The Clinic’s extensive investment in people, processes and equipment all support one primary focus: the patient.
“Our team of highly trained professionals — physicians, physicists, nurses, therapists and others — is committed to treating patients with neoplastic diseases in a caring and efficient environment using cutting- edge technology and the most up-to-date information available,” Cassels noted. Even the Clinic’s emphasis on clinical trials, research and teaching, as well as Emory’s interdisciplinary marriage of surgery, medical oncology and radiation oncology, ultimately are geared toward the patient as the end game.
Cassels attributes her department’s strength of focus and achievement on teamwork, from the department chair to the support staff. “Each member of the department has a strong role in achieving quality patient care and excellent patient satisfaction,” she said. “This begins by strong front-end focus on interaction with the patient on the phone and reception areas. No technology will please the patient as much as a smiling face and pleasant staff interaction will.”
Such motivation and philosophy starts at the top, according to Fox. “I try to keep everyone inspired,” he said. “People like to know why we’re doing something and why it’s important.
Cassels, who also is a radiation therapist, strives to build team spirit as much as control the bottom line through a variety of awards and rewards to showcase personal and professional success. And she has a lot to work with. Emory’s radiation oncology services patient satisfaction scores, as tabulated by Press Ganey Associates Inc., consistently reach the low 90th percentile in relation to other services that comprise the Clinic. Among its patient-friendly programs, for example, is lymphadema therapy for post-treatment of breast cancer. Originally, the Susan B. Komen Breast Cancer Foundation supported the program, but the Clinic now supports it through operational funds, “due to evidence from the outcomes of the therapy that have proven to be very advantageous to the patients,” she said.
“Both the staff and the physicians need to be engaged in the patient satisfaction process,” Cassels said. “We hold them accountable with incentives. We’re very team-oriented. The front desk staff is just as important as the doctors. They just picked a different profession.”
Photos courtesy of Jack Kearse, Emory University




 April 15, 2026
April 15, 2026