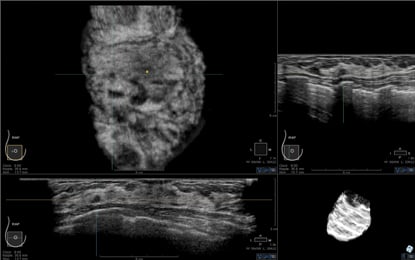
3-D volumetric ABUS
Lately, it seems that breast imagers cannot go a week without reading about new breast imaging research or seeing an article on breast density, the associated risk of breast cancer and the limitations of mammography. In this article, I will summarize today’s current understanding and also provide a look into what I believe the future holds for breast screening.
Breast Density and Breast Cancer
John N. Wolfe in 1976 was one of the first researchers who described an association between increased breast density (breast parenchymal patterns) and the risk of breast cancer. Published literature over the last few decades has repeatedly demonstrated the conclusive evidence of a link between dense breast tissue and breast cancer.
Boyd, Yaffe, Martin and Kerlikowske, among others, have all confirmed Wolfe’s observations. Now we know that the increased cancer risk is four to six times higher for women with extremely dense breast tissue. Increased breast density also has been shown to be an independent risk factor for breast cancer, and it conveys a risk greater than all other risk factors except for age, BRCA mutation, prior history of breast cancer or atypia.
More recently, Tamimi et al. has shown that the risk of breast cancer increases progressively with increasing breast density and that these relationships were stronger with tumors that were larger, higher grade, estrogen receptor negative and associated ductal carcinoma in situ (DCIS). Keller reported a statistically significant correlation with increasing volume of fibroglandular tissue and six single nucleotide polymorphisms.
Mammography Limitations
Breast density on a mammogram is a significant problem for the radiologist. An analogy is often made that describes a radiologist’s difficulty in the detection of breast cancer in dense breasts: “Trying to find a specific snowball in a snowstorm.”
To detect breast cancer, mammography is dependent upon contrast differences between breast cancer and normal breast tissue. In breasts with primarily fatty tissue, the cancer is easiest to detect, with up to 98 percent sensitivity. In breasts with an increased percentage of dense fibroglandular tissue, there may be little to no difference in contrast between cancer and normal epithelial/stromal tissue, with sensitivity falling as low as 48 percent.
The number of women with dense breasts is not insignificant, affecting 74 percent of women between ages 40 to 49, 57 percent for ages 50 to 59, 44 percent for ages 60 to 69, and 36 percent for ages 70 to 79. The risk of developing an interval cancer (cancer presenting between yearly screening examinations) is nearly 18-fold higher in patients with dense breasts, with a concurrent potential for increased medical malpractice risk in this same group of patients.
Radiologists Know, Patients Don’t Know
While the limitations of mammography in women with dense breast tissue have long been known to radiologists, patients have been largely kept “in the dark,” not only about their own degree of breast density, but also about the decreased sensitivity and increased risk of breast cancer. The mammogram results letter sent to the patient does not typically include information on their specific level of dense breast tissue or say that mammograms can have limitations in dense breast tissue. A national survey conducted by Harris Interactive in 2010 of 599 women concluded that 95 percent of women above the age of 40 did not know their breast density, and almost 90 percent were unaware that increased breast density increases their risk of breast cancer.
Over the last few years, an organization, Are You Dense Inc., started by breast cancer patient turned advocate Nancy Capello, Ph.D., has lead a nationwide campaign to create a heightened awareness of breast density on the state and national levels. Capello, who despite having had annual mammograms interpreted as “normal,” was diagnosed with late stage breast cancer. Her efforts resulted in Connecticut becoming the first state to legislatively mandate breast density notification directly to the patient, as well as payor coverage for supplementary screening, such as breast ultrasound.
A companion organization, Are You Dense Advocacy Inc., also was formed to help stimulate and guide legislative efforts across all states and at the national level. There are now breast density notification laws in effect in three states and ongoing legislative efforts in more than 15 states, as well as at the federal level (HR 3102). Social media is helping to drive breast density knowledge to the patient, and there is a growing base of consumers who are demanding breast density notification and supplemental breast cancer screening from the breast imager.
Ultrasound Screening for Dense Breasts
Research has been done using ultrasound to supplement mammography for screening of patients with dense breast tissue. At least nine peer-reviewed publications have shown that adding ultrasound to mammography results in approximately 3.5 additional cancers detected per 1,000 patients in those with dense breasts.
However, the limitations of the current hand-held ultrasound technology used for diagnostic examinations have prevented widespread adoption in the screening population. These include: length of exam in the screening environment, lack of skilled technologists or dedicated breast radiologists to conduct screening breast ultrasounds, the inherent operator dependencies of ultrasound technology and the uncertainty and inconsistencies of scan completeness. All published studies to date, but one, have used experienced breast radiologists to perform the traditional hand-held breast ultrasound scans.
In addition, the average scan times alone — 19 minutes, reported by Berg et al. (ACRIN National Breast Ultrasound Trial) — would be problematic for most radiologists. While sensitivity is acceptable, specificity is less than mammography and is often cited as a significant limitation for widespread adoption.
As an alternative to the limitations of hand-held ultrasound for breast cancer screening, automated breast ultrasound (ABUS) systems have been developed by three companies (Siemens, U-Systems Inc. and SonoCine). Use of the SonoCine device requires placement of a robotic device that holds and guides an existing standard hand-held ultrasound transducer, producing between 2,000 and 5,000 axial images in a cine format.
The Siemens and U-Systems stand-alone devices utilize a large-format transducer that acquires a single volume of the breast automatically in less than 60 seconds. The devices image a much larger portion of the breast as a volume, with 3-D reconstruction for a coronal plane and two standard orthogonal planes for review on a proprietary workstation.
Only one prospective automated breast ultrasound study has been published to date (Kelly et al.) showing a 100 percent increase in breast cancer detection with a positive predictive value (PPV) similar to mammography (38.4 vs. 39 percent). Reported reading times for a bilateral ABUS screening exam differ, with five to seven minutes reported for the SonoCine device and just under three minutes for the U-Systems device.
Standardization of Breast Density —Is It Absolutely Necessary to Perform Ultrasound Screening?
Breast density is defined as the volume of dense tissue divided by the volume of the entire breast, reported as a percentage. Historically, the purpose of BI-RADS reporting of subjective BI-RADS density categories 1-4 (0 to 24 percent, 25 to 50 percent, 51 to 75 percent and 76 to 100 percent) was to convey the sensitivity of mammography to detection of cancer. This subjectivity has been criticized as having less-than-optimal intra-observer and inter-observer agreement, with a call for better standardization and a less qualitative assessment.
Commercial software exists to measure breast density and provide a quantitative value (Volpara, iCAD and Quantra), but this step adds costs to screening examinations that are already under-reimbursed. While software programs such as these should add quantifiable and reproducible reporting of breast density, they may not be absolutely necessary to achieve significant improvements in breast cancer detection using supplementary screening with ultrasound. As breast density is a continuum, it likely makes little difference whether a patient’s breast is computed to be 49 percent or 51 percent by commercial software. Radiologists are typically well calibrated in their subjective interpretation of breast density and typically select appropriate patients in which to perform supplementary ultrasound screening with adequate sensitivity.
Recent Advances for Breast Cancer Screening
In April 2012, the U.S. Food and Drug Administration (FDA) granted pre-market approval (PMA) to U-Systems Inc. (USI) for use of its somo.v automated breast ultrasound device as an adjunct to mammography, explicitly for breast cancer screening for asymptomatic women with dense breast tissue. A research study was conducted by the University of Chicago, and the study data submitted to the FDA showed more than a 100 percent increase (31 percent absolute increase) in breast cancer detection rate in asymptomatic patients with dense breasts and a normal mammogram when a screening mammogram and the USI ABUS were combined, compared to mammography alone. A statistically insignificant decrease in specificity was not associated with this statistically significant gain in sensitivity.
The majority of the cancers detected with USI’s ABUS combined with mammography were small, invasive, node-negative, early stage cancers. If generalized in the real world screening environment, this may indeed provide the necessary improvement in specificity necessary for widespread adoption. Because radiologists are new to ultrasound screening, as well as the presentation of images in a 3-D volumetric format, formalized training in interpretation of automated breast ultrasound may be necessary (and likely may be mandated by the FDA) in order to maintain adequate specificity while keeping sensitivity high.
Unanswered Questions
Where does screening breast ultrasound and, more specifically, ABUS, fit into the current scheme of breast screening, given that breast tomosynthesis was also recently FDA-approved? There is no published research directly comparing digital tomosynthesis and automated breast ultrasound as adjuncts to mammography for breast cancer screening in the same population group. Although digital tomosynthesis (DT) study data has been shown to reduce false positives, the same DT study data does not demonstrate the sensitivity advantage that the USI ABUS study demonstrated. There are discrepancies in cancer detection rates for women with dense breast vs. fatty breast tissue, and there may be a role for both of these complementary technologies across all screening population groups.
Will the increased sensitivity of breast cancer detection using hand-held ultrasound as an adjunct to screening mammography in dense breasts be reproducible using automated breast ultrasound in the “real world?” The results of the SOMO-INSIGHT clinical study will be released soon and may provide an answer. It compares the sensitivity of digital mammography to the combination of digital mammography and ABUS in patients with dense breasts in greater than 16,000 patients at both academic and community facilities.
In Summary
The increased risk of breast cancer in patients with dense breasts is well established, as well as the limitations of 2-D mammography. Patients are becoming more educated about breast density due to the efforts of the advocacy group AreYouDense Inc. and the breast density notification laws that have been introduced at state levels. Hand-held ultrasound has shown clinical value in this group of patients as an adjunct to mammographic screening. However, there are a number of limitations to hand-held ultrasound screening’s widespread adoption.
New technology, such as automated breast ultrasound, has the potential to overcome these limitations. We await the results of future research. itn
Marc Inciardi, M.D., is assistant professor of radiology at the University of Kansas Medical Center, Kansas City, Kan. He is a principle investigator in the SOMO-INSIGHT clinical study and is head of faculty training for U-Systems. He has received compensation for physician training, but owns no stock in U-Systems.
References:
1. American College of Radiology. “Breast Imaging Reporting and Data System,” 4th edn. Reston (VA): American College of Radiology, 2003.
2. Berg WA, Blume JD, Cormack JB, et al. “Combined screening with ultrasound and mammography vs mammography alone in women at elevated risk of breast cancer.” JAMA 299:2151-2163, 2008.
3. Boyd NF, Guo H, Martin LJ, et al. “Mammographic density and the risk and detection of breast cancer.” N Engl J Med. 2007; 356(3):227-36.
4. Byrne C, Schairer C, Wolfe J, et al. “Mammographic features and breast cancer risk: effects with time, age, and menopausal status.” J Natl Cancer Inst 1995;87:1622-9.
5. Checka CM, Chun JE, Schnabel FR, Lee J, Toth H. “The relationship of mammographic density and age: implications for breast cancer screening.” AJR Am J Roentgenol. 2012 Mar;198(3):W292-5.
6. Giger EL, et al. “Clinical Reader Study examining the performance of mammography and automatic breast ultrasound in breast cancer screening.” Submitted for presentation, RSNA 2012.
7. Kelly. “Breast cancer detection using automated whole breast ultrasound and mammography in radiographically dense breasts.” Eur Radiol, DOI 10.1007/s00330-009-1588-y; pub online 9/2/09.
8. Legislative update: AreYouDense.org, July 2, 2012.
9. Singletary SE. “Rating the risk factors for breast cancer.” Ann Surgery 2003;237:474-82.
10. Wolfe JN. “Risk for breast cancer development determined by mammographic parenchymal pattern.” Cancer 1976;37:2486-92.


 May 22, 2026
May 22, 2026 









