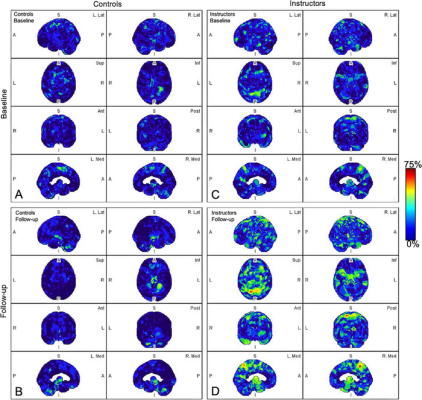
Parametric maps of amyloid deposition in healthy control participants (A and B) and blast-exposed military instructors (C and D) at baseline (A and C) and follow-up (B and D). The blue-to-red scale indicates the frequency of statistically abnormal amyloid uptake in a particular brain voxel. Whereas no abnormal amyloid uptake was identified at baseline or follow-up in healthy control participants (A, B), amyloid deposition occurred most frequently in blast-exposed participants in the superior parietal lobules, precuneus, cingulum, paracentral lobules, and anterior temporal and occipital lobes (D). A = anterior, Ant = anterior, I = inferior, Inf = inferior, L = left, Lat = lateral, Med = medial, P = posterior, Post = posterior, R = right, S = superior, Sup = superior. Image courtesy of RSNA.
May 22, 2023 — New research finds that the brains of otherwise healthy military personnel who are exposed to explosions show an abnormal brain accumulation of amyloid-beta protein—a protein that plays a role in the development of Alzheimer’s disease. The results of the study were published today in Radiology, a journal of the Radiological Society of North America (RSNA).
Research over the last several decades suggests that there might be a relationship between repetitive or severe traumatic brain injury (TBI) and abnormal amyloid-beta accumulation. Certain forms of amyloid-beta can accumulate into tangles and plaques in the brain which can lead to cognitive decline and neurodegenerative diseases such as Alzheimer’s disease.
“Amyloid-beta is a molecule not normally found in the brains of young patients,” said study author Carlos Leiva-Salinas, M.D., Ph.D., M.B.A., associate professor of radiology at the University of Missouri School of Medicine in Columbia, Missouri. “Amyloid-beta accumulation in the brain is proposed to be an early event in the pathogenesis of Alzheimer’s disease, the most common type of dementia worldwide, impacting millions of people.”
TBI can be the result of direct head trauma, such as from a fall or from playing contact sports, but it can also result from indirect forces—such as shockwaves from battlefield explosions—that shake the brain violently in the skull.
Previous autopsy studies have shown the presence of amyloid plaques as early as hours after severe brain injury.
“Non-invasive positron emission tomography, or PET, imaging could be used to identify early-stage amyloid-beta accumulation in individuals or professions exposed to traumatic brain injury such as military personnel, police officers, firefighters, football players, etc.,” Dr. Leiva-Salinas said.
For the study, researchers recruited nine military grenade or breacher instructors at Fort Leonard Wood Military Base in Fort Leonard, Missouri, from January 2020 to December 2021. Grenade and breacher instructors are military officers who train recruits in the use of hand grenades and explosives or other mechanical methods to force open doors.
An additional nine civilians were included in the study as a healthy control group. All participants had no previous history of concussion, and they were all males in their early 30s, an age at which amyloid accumulation is not expected.
The 18 participants were evaluated twice. The first evaluation was to establish a baseline and the second occurred after blast exposure, approximately five months after the baseline examination. The military instructors filled out a digital log with the number of exposures to explosions, including the firing of weapons. The control participants were evaluated at similar time points.
All participants underwent a PET scan of the head to evaluate and quantify amyloid changes. Analysis software was used to segment six brain regions that are usually associated with Alzheimer’s disease and TBI.
Abnormal amyloid accumulation was seen in six of the nine participants who were exposed to explosions. Three of the participants had one region of the brain with increased amyloid accumulation, two participants had two regions, and one participant had three regions with abnormal accumulation.
None of the healthy control participants showed any abnormal amyloid accumulation.
“Further research needs to be done to establish the relationship between the frequency and the severity of traumatic brain injury and the degree of amyloid changes in the brain, the natural course of the observed accumulation, and other potential biologic risk factors for amyloid plaque deposition and the development of cognitive decline,” Dr. Leiva-Salinas said.
For more information: www.rsna.org
Related Alzheimer's Content:
Impaired Glymphatic System May be Linked with Progression of Alzheimer's Disease, Finds New Study
FDA Grants Accelerated Approval for Alzheimer’s Drug Aduhelm
VIDEO: Researchers Use MRI to Predict Alzheimer's Disease
Brain Iron Accumulation Linked to Cognitive Decline in Alzheimer's Patients
Good Results for Alzheimer’s Imaging Agent
NIH Augments Large Scale Study of Alzheimer’s Disease Biomarkers
Alzheimer’s Association Launches New Website for IDEAS Study
PET Tracer Gauges Effectiveness of Promising Alzheimer's Treatment


 May 20, 2026
May 20, 2026 









