March 23, 2016 — New research shows that innovative scanning-led surveillance can help identify the need for, and guidance of, neck dissection for head and neck cancer patients. This discovery means patients may no longer have to undergo invasive post-treatment surgery to remove remaining cancer cells.
The study from the Universities of Birmingham and Warwick, published in the New England Journal of Medicine, used advanced imaging to identify cancer cells still present after treatment of head and neck cancer with primary chemoradiotherapy.
Previous guidelines meant that all head and neck cancer patients have to undergo neck dissection surgery, a three-hour operation with considerable morbidity and up to a one-week hospital stay, because there was no reliable way to identify which patients still had remaining cancer cells.
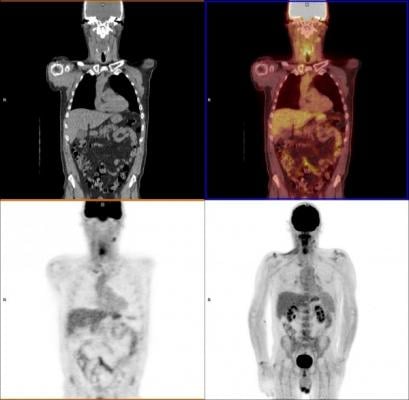
The use of positron emission tomography–computed tomography (PET-CT) scans for image-guided surveillance meant that routine post-treatment operations were no longer necessary, and can now be better targeted to the right areas in those 20 percent of patients who still have persistent cancer.
Prof. Hisham Mehanna, from the Institute of Head and Neck Studies and Education (InHANSE) at the University of Birmingham, explained, “After treatment, remaining cancer cells play something akin to hide and seek. Our study shows that using this PET-CT scan we can hunt them down, find them and remove them effectively.”
The study was conducted across 37 centers in the United Kingdom, overseen by Warwick Clinical Trials Unit, University of Warwick. Five hundred sixty-four patients were recruited between 2007 and 2012, with 282 in the image-guided surveillance group and 282 in the neck dissection control group.
Only 54 (19 percent) of the 282 in the image-guided surveillance group went on to undergo neck dissection surgery, compared with 221(78 percent) of the 282 in the control group.
Survival rates, quality of life and other factors were considered and remained similar across both groups.
Prof. Janet Dunn, from Warwick Clinical Trials Unit said, “This is an important study for the future management of these patients. When we first designed the study in 2007, patients were undergoing routine neck dissection and they did not have access to PET-CT. The results show that the use of PET-CT imaging can prevent unnecessary operations and reduce associated surgical complications.”
Mehanna added, “Patient outcomes, and avoiding unnecessary surgery, are the main goals of this study. But there is a cost saving to be made too. When compared with neck dissection, the PET-CT guided surveillance saved £1,492 (US$2,190) per person for the NHS. Carry that across the tens of thousands of cases each year across the world and you see a significant saving that can be redistributed into other therapies.”
Ninety percent of head and neck cancers are squamous cell carcinomas, known as head and neck squamous cell carcinomas (HNSCC). HSNCC is the sixth leading cancer by incidence across the globe, with an estimated 500,000 new cases reported each year.
The research was funded by the National Institute for Health Research (NIHR) Health Technology Assessment (HTA) Programme.
For more information: www.nejm.org


 May 27, 2026
May 27, 2026 









