November 8, 2017 — CureMetrix, a company developing computer-aided detection (CAD) for mammography to improve clinical outcomes, recently expanded its medical advisory board. Made up of leaders in radiology from the U.S.’s top healthcare institutions, the medical advisory board contributes valuable clinical perspectives to CureMetrix’s investigational image analysis solutions leveraging artificial intelligence and deep machine learning.
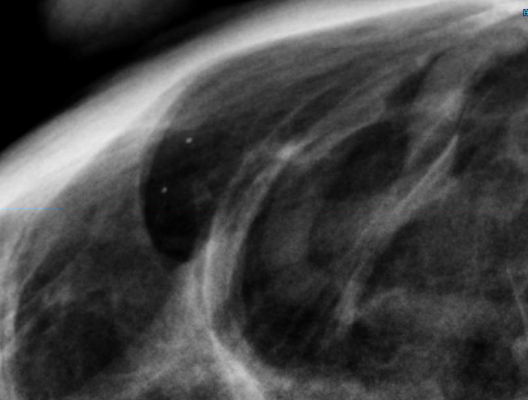
CureMetrix is currently developing a physics-based software algorithm that allows radiologists to get more specific and sensitive readings of breast images from existing imaging systems.
Advisory board members will work with CureMetrix Chief Medical Officer William G. Bradley, M.D., Ph.D., and former chair of the University of California (UC) San Diego Health Department of Radiology.
CureMetrix advisory board members include:
- Jade de Guzman, M.D., is a diagnostic radiologist at Sharp Rees-Stealy Medical Group in San Diego. She is also a voluntary assistant clinical professor at the University of California, San Diego, Department of Radiology. She completed her radiology residency and breast imaging fellowship at University of California, Los Angeles. Her main interests include all aspects of diagnostic and interventional breast radiology;
- Curtis Duffield, M.D., is a breast imager at Sharp Rees-Stealy Medical Group in San Diego. He completed his medical training and radiology residency at University of California, Davis followed by a dedicated breast imaging fellowship at Harvard’s Massachusetts General Hospital. He has a special interest in computational methods to improve decision making and early detection of breast cancer;
- Christopher Comstock, M.D., is the imaging co-chair of the ECOG-ACRIN Breast Committee, chair of the American College of Radiology (ACR) Committee on BI-RADS (Breast Imaging-Reporting and Data System) Breast MRI (magnetic resonance imaging), and member of the NCI Bold task force. Comstock was previously the assistant professor of radiology at the University of Chicago and Northwestern University Hospital’s Lynn Sage Breast Center. He was also chief of breast imaging at the University of California San Diego and was chair on several boards and committees, including the ACR Breast Ultrasound Accreditation program and ACRIN Institutional Participants Committee. He has co-authored a textbook on breast cancer imaging, written several book chapters, been involved in numerous breast imaging publications and has given over 400 invited lectures;
- Vivian Lim, M.D., is a radiologist and head of mammography overseeing the comprehensive breast imaging service she developed at four Scripps Clinical Medical Group locations in San Diego. She is a member of the Alpha Omega Alpha Medical Honor Society, the ACR, the American Roentgen Ray Society, the Radiological Society of North America (RSNA) and the San Diego County Radiologic Society. She graduated from the University of Texas Health Science Center in San Antonio, did an internal medicine internship, followed by diagnostic radiology residency and another year of fellowship in MRI, all at University of California, San Diego;
- Jenna Liu, M.D., is a radiologist at Sharp Grossmont Hospital in San Diego. She is the vice president of X-Ray Medical Group and was previously the chair and vice chair of the Department of Radiology at Sharp Grossmont Hospital as well as president of the San Diego Radiological Society. She has a special interest in all aspects of MRI, mammography and developing tools for early detection of breast cancer;
- Allen Nalbandian, M.D., is a radiologist at Palomar Medical Center in Escondido, Calif. He is the president of Valley Radiology Consultants and is an active member of the ACR, RSNA, the American Roentgen Ray Society and the Society of Breast Imaging. Nalbandian previously served as the president of the San Diego Radiological Society. He has a special interest in all phases of women’s imaging including mammography, breast ultrasound, breast MRI and the entire spectrum of breast interventional procedures including stereotactic, ultrasound and MRI guided breast biopsy procedures;
- Michele Rochelle, M.D., is board certified in diagnostic radiology with the American Board of Radiology. She received her Bachelor of Science degree from the University of California, San Diego and her medical degree from the University of California, Davis. Rochelle completed her diagnostic radiology residency at the University of California, San Diego. She then completed her Breast Imaging Fellowship at the University of Washington. She has been practicing in the San Diego area for several years and specializes in breast imaging, with a focus on early breast cancer detection through screening mammography; and
- Alyssa Watanabe, M.D., is a clinical associate professor of radiology at the University of Southern California Keck School of Medicine. She is a nationally recognized expert in radiology with over 20 years of practice and has lectured on the topic of continuing medical education meetings. Her articles have been published in numerous leading journals like the American Journal of Radiology and she is past president of the American Society of Spine Radiology. Watanabe was previously director of breast imaging at Patricia L. Scheifly Breast Health Center in Whittier, Calif., and director of breast MRI at MemorialCare Imaging Center at Long Beach Memorial.
CureMetrix was founded in 2014 on the belief that better medical image analysis technology could lead to better outcomes for breast cancer patients. The company is developing investigational physics-based artificial intelligence and deep machine learning solutions to help radiologists get more accurate readings of breast images. Through its research partnerships with leading hospital radiology departments, CureMetrix has evaluated more than 500,000 mammogram images to identify potential false negatives, which are undiagnosed cancers, and false positives, which are unnecessary recalls of patients to review anomalies that turn out to be normal. False negatives can occur at a rate of about one in five breast cancers.1 False positives affect 7-12 percent of all women after an initial mammogram.2 Reducing false positives could save a significant portion of the $4 billion per year spent on unneeded and sometimes invasive procedures such as biopsies.3 More importantly, reducing false negatives could save lives as well as reduce the cost and difficulty of cancer treatment through early detection.
For more information: www.curemetrix.com
References
2. http://ww5.komen.org/BreastCancer/AccuracyofMammograms.html
3. http://content.healthaffairs.org/content/34/4/576.abstract


 May 12, 2026
May 12, 2026