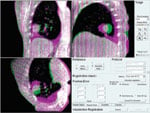
Elektas Symmetry tool quantifies the set-up changes required to accommodate baseline shifts.
(Updated content links are at the bottom of this article)
One of the biggest challenges with tumor control is accelerated repopulation. Surviving tumor cells can repopulate after a few fractions of radiation are delivered or during intervals between treatments. To make matters worse, the rate of tumor repopulation accelerates after each successive treatment.
As the success or failure of a therapy is directly related to the rate of repopulation, radiation oncologists are testing new strategies to better control tumor growth during treatment. These strategies include the use of advanced forms of radiation delivery, such as intensity-modulated radiation therapy (IMRT) and image-guided radiotherapy (IGRT), and shortening the entire course of treatment.
Arc-Based Radiotherapy
Arc-based IMRT is designed to improve dose distribution through intensity modulation. Helical tomotherapy and volumetric modulated arc therapy (VMAT) are two arc-based approaches to delivering of IMRT.
Elekta and Varian Medical Systems developed the first commercially available solutions providing VMAT. With the Elekta VMAT system single or multiple radiation beams sweep in uninterrupted arcs around the patient. Clinicians can use Elekta VMAT with complete or partial arcs to reduce treatment times from the eight to 12 minutes required for conventional radiation therapy to as few as two minutes.
Varian’s RapidArc volumetric modulated arc therapy delivers a complete IMRT treatment in a single rotation of the treatment machine around the patient. The system was engineered to deliver image-guided IMRT two to eight times faster than conventional IMRT or helical tomotherapy. RapidArc’s use of the primary beam is said to reduce secondary stray radiation caused by scatter and leakage by more than 50 percent, compared with fixed field IMRT.
While VMAT offers faster treatment times, many clinicians prefer Tomotherapy’s Hi-Art system for its precision in targeting tumors, despite somewhat longer treatment times. To further hone beam accuracy, the Hi-Art system’s treatment modes now includes a 3-D conformal option.
“From a physicist’s perspective, tomotherapy is a form of VMAT,” indicated Robert Miller, M.S., medical physicist, Meridian Park Radiation Oncology Center, Tualatin, Ore. “It is volumetric therapy, but it is doing it with multiple helical arcs that overlap, and we can actually control that overlap. Whereas VMAT and RapidArc are maybe one, maybe two, maybe three arcs total. [Tomotherapy] is doing that, but it is doing it many times. The treatment times, however, can be significantly longer than RapidArc or VMAT.”
To speed up treatment times, Tomotherapy Inc. recently added TomoDirect, a discrete-angle delivery mode, to the Hi-Art treatment system. This new technology is designed to allow Hi-Art system users to quickly plan and deliver advanced treatments with a series of linear beam paths, rather than the existing helical path. This can provide time savings in both the planning and delivery phases for several clinical scenarios, including whole breast irradiation and palliative treatments.
Conformality
Both helical tomotherapy and VMAT are advanced forms of radiation delivery that use IMRT and IGRT in terms of the way the therapy is delivered. The purpose of helical tomotherapy and volumetric therapy is to produce conformal radiation dose distributions that shape accurately around the target or tumor with as little dose to the surrounding tissue as possible.
“The difference is that tomotherapy delivers the beam in a helical fashion in smaller slice volumes, whereas VMAT delivers this using one, or sometimes two to three larger volumes,” explained Minesh P. Mehta, M.D., University of Wisconsin-Madison, professor of human oncology.
For both techniques, the backbone of radiation delivery is intensity modulation. The more modulation, the more conformal a plan becomes. Depending on the clinical situation, the degree of conformality can vary, explains M. Mehta, from exquisitely to moderately to minimally conformal or not conformal at all.
“You would need exquisite modulation, in which there is a very sharp dose fall off from normal tissue to the tumor, if it’s an extremely complex three-dimensional, unusually shaped target located in proximity to several critical structures,” said M. Mehta.
“You’ll need to conform the dose at multiple levels, when you have targets that are large and irregular in shape. That requires significant intensity modulation across all three dimensions,” indicated M. Mehta. “Using multiple passes through the tumor, through multiple helices, which is what tomotherapy does, tends to produce a more conformal dose distribution in such a context.”
Head-to-Head Comparison
The clinical data in a head-to-head randomized comparison of different technologies for IMRT, such as VMAT and helical tomotherapy, is limited. However, the study, “Evaluation of Arc-based Intensity Modulated Radiotherapy for Head and Neck Cancer,” published in 2009 in the International Journal of Radiation Biology Physics[1], found tomotherapy plans better at sparing surrounding healthy tissue, and VMAT’s treatment delivery time faster.
The objective of this study was to compare treatment plans for head and neck (H&N) cancer using VMAT, helical tomotherapy and fixed field IMRT in terms of plan quality, delivery efficiency and accuracy.
The researchers found, “Both VMAT and tomotherapy are capable of providing highly uniform target doses as compared with fixed field IMRT.”
In terms of accuracy, tomotherapy delivered less toxicity to surrounding tissues.
“Tomotherapy plans achieved slightly better sparing of the parotid glands, spinal cord, brain stem, larynx, and oral cavity with an average mean organ dose that was 2 percent lower than VMAT and 5.1 percent lower than fixed field IMRT,” the researchers stated.
In terms of timing, they found the average delivery time of the VMAT plans was 4.9 minutes as compared with 7.5 minutes for tomotherapy and 12.7 minutes for fixed field IMRT.
“VMAT technique is able to provide 35 percent reduction in delivery time as compared with tomotherapy,” the authors concluded.
The question that this study does not answer is how delivery time affects patient outcome.
“We really don’t know if faster delivery of radiation makes a difference,” said one of the authors of the study, Vivek Mehta, M.D., radiation oncologist, Swedish Cancer Institute, Seattle. “The shorter treatment time might be clinically relevant particularly for some patients with head and neck cancer treatment.”
Need for Speed
While the objective in every treatment plan is to improve patient outcomes, there are two objectives for delivering treatments faster. One is to mitigate tumor repopulation, and the other is to reduce tumor motion during dose delivery.
With the first strategy, initial studies aimed at tumor control tried increasing the number of fractions per session. However, this tactic had limited benefits because the overall treatment course had to be extended, which resulted in tumor repopulation.
Recently, researchers have taken a new approach, accelerated fractionation of radiotherapy. In this scenario, the overall treatment time is reduced, providing less opportunity for repopulation of tumor cells. This procedure allows greater normal tissue recovery to occur during the intervals between treatments. This type of fractionation has been successful in controlling Burkitt’s lymphoma and non-small cell lung cancer.[2]
“You can do hypofractionation with many technologies – tomotherapy and VMAT,” said M. Mehta. “Radiobiologic considerations imply that if you shorten the overall course of treatment, you more effectively treat the tumor, compared to a longer course of treatment. The expectation is that you would get a superior result in controlling the tumor with a hypofractionated, or shorter schedule.”
Accelerated Hypofractionation
Several new studies tested the efficacy of accelerated hypofractionation.
“With advances in technology that incorporate IMRT and IGRT, more trials are being done looking at hypofractionation,” M. Mehta said. “These trials are in their early phases, but are producing initial data that support the hypothesis that shorter schedules could be better for several tumor types. As a consequence, in clinical practice, in certain diseases, clinicians have started using shorter schedules.”
In a trial led by M. Mehta, researchers applied accelerated hypofractionation to overcome tumor repopulation for non-small cell lung cancer. They incorporated the technique into its conformal dose-delivering platform with helical IMRT and IGRT. They were able to reduce the treatment schedule for 25 fractions over five weeks, instead of the traditional six to seven weeks or longer. In essence, the radiation dose was raised and delivered in less time.
Clinical trial cooperative groups, such as the Radiation Therapy Oncology Group (RTOG), are in the process of developing trials that will do head-to-head comparison of a shorter schedule versus longer schedules in prostate cancer, and possibly other diseases.
“Hopefully, this will give us a definitive answer as to whether shorter schedules are better or not,” added M. Mehta.
Moving Target
Another tactic is to shorten fraction times to limit tumor motion during dose delivery. Shorter treatments cause less discomfort and patients tend to move less. In addition, there is less time allotted for tumors to move during dose delivery.
According to M. Mehta, an average patient tomotherapy treatment typically takes four minutes.
“The range is four to seven minutes, but it can be easily reduced down to three minutes by varying the amount of intensity modulation. Many facilities treat 30 to 40 patients a day by changing the amount of intensity modulation,” said M. Mehta.
A retrospective study measured the amount of time it took to treat patients for each fraction. Over a three-year time period, researchers looked at 1,000 patients, with nine different disease types, treated with helical tomotherapy. The average treatment time was four to seven minutes.
“There is not a huge differential in time between the two technologies to deliver radiation. You can shorten the treatment without any substantial or significant change in the plan quality relative to a VMAT plan,” said M. Mehta. “It is very important when comparing the amount of time it takes to deliver a treatment that one is really talking about the same, exact plan.”
Recently, Varian introduced TrueBeam, a platform for image-guided radiotherapy, which also shortens treatment times. It targets moving tumors by dynamically synchronizing imaging, patient positioning, motion management and treatment delivery.
Compared to Varian’s other systems, TrueBeam delivers treatments up to 50 percent faster and with a dose delivery rate of up to 2,400 monitor units per minute, double the maximum output of earlier systems.
Elekta also is targeting treatment times with a new image-guidance tool called Symmetry. This solution allows clinicians to quantify the set-up changes required to accommodate baseline shifts or tumor path changes between treatments. By using anatomically correlated guidance as an alternative to gating, it aims to significantly shorten treatment times with less set-up complexity.
Whether faster treatment times result in greater precision and improved patient outcomes is yet unknown and requires further investigation. But what is certain is the manufacturers of VMAT systems and helical tomotherapy are working hard to shorten these times.
“The shorter treatment time may or may not be relevant to tumor control. It is possible that it will have a greater effect, but I’m not sure it has been studied,” said V. Mehta.
He noted, “The easiest benefit to document is the improved clinical throughput.”
What may be more important to outcome than treatment time, according to V. Mehta, is controlling patient movement. But motion, he added, “can be minimized by a shorter treatment time.”
Read the updated article “Two of a Kind: VMAT Versus Tomotherapy”
Read the related article “The Effect of Planning Speed on VMAT Plan Quality”
Reference:
1. Rao, M., Yang, W., Vivek, M., et al. “Evaluation of Arc-based Intensity Modulated Radiotherapy for Head and Neck Cancer.” International Journal of Radiation Biology Physics Vol. 75, Issue 3, Supplement, Page S419 (Nov. 1 2009).
2. Olle, D., “Repopulation of Cancer Cells.” 2005. www.suite101.com/article.cfm/new_cancer_treatments/117298



 May 06, 2026
May 06, 2026 









