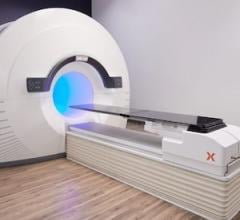
GE Healthcare combined its CT with the motion management capabilities of its Discovery PET system to create the Discovery PET/CT 600.
The number of new clinical applications for positron emission tomography (PET) and PET/CT are constantly unfolding in new disease areas, and, subsequently, PET procedure volumes are increasing at unprecedented rates.
The growing body of clinical evidence demonstrating that PET has greater sensitivity and is more accurate in detecting cancer compared to other imaging tools has weighed in heavily amongst healthcare decision-makers in government, prompting the recent proposal by Centers for Medicare & Medicaid Services (CMS) to expand reimbursement for PET.
Expanded Coverage
The recently proposed national coverage determination (NCD) will consider extending coverage for initial diagnostic testing with PET for many Medicare beneficiaries who are being treated for cancer.
Under the Coverage with Evidence Development (CED) program, CMS had issued a national coverage determination in 2005 that tied Medicare coverage of PET scans to the collection of clinical information about the effect of the test on the beneficiary’s cancer care. This information was obtained through the National Oncologic PET Registry (NOPR) observational study. Without CED, these tests would not have been covered by Medicare.
The purpose of CED is to develop evidence on the utilization and impact of the item or service evaluated in an NCD, so that Medicare can document the appropriateness of use of that item or service in Medicare beneficiaries under current coverage; consider future changes in coverage for the item or service; and generate clinical information that will improve the evidence base, which providers use to support their recommendations to Medicare beneficiaries regarding the item or service.
The sponsors of NOPR submitted a formal written request to reconsider the 2005 coverage determination to CMS, based on the evidence they had collected and published. This proposed expansion in coverage marks the first time that CMS has reviewed medical evidence arising from its CED program.
The proposed decision addresses coverage for cancer staging and restaging, in addition to initial diagnosis. Two important items in the CMS draft include a proposal to replace coverage for “diagnosis, staging and restaging and treatment” with “initial treatment” and “subsequent treatment.” CED will still be required for PET scans for subsequent treatment strategies, as CMS believes that the current evidence is not adequate to provide coverage for PET scans in guiding subsequent treatment. After a public comment period, a final decision is expected in April 2009.
The Burden of Proof
Despite the fact that many PET procedures have not been reimbursed, PET adoption has proliferated, leaving many to wonder: “How long will PET continue to go uncovered and what will it take for it to become the standard of care?”
IMV Medical Information Division, a market research firm, estimated that 1.13 million clinical PET and PET/CT patient studies were performed in 2005, which represented an annual growth rate of 26.5 percent since 2003. Another leader in market research, Bio-Tech Systems Inc., expects that by 2010, PET procedures should rise to 2.1 million.
In anticipation of growing utilization, the NOPR was created in 2006, and since its inception, several bodies of data have been released by various authors demonstrating the superiority of PET over other imaging tools in the management of cancer.
One such study led by Bruce Hillner, M.D., found that clinicians changed their treatment plan 36.5 percent of the time based on PET scan results. Specifically, biopsies were avoided in 75 percent of patients who had planned to undergo one. This study also revealed that PET identifies more areas of active cancer than other imaging tools, a finding that appears to be consistent across a wide range of cancers.
Another NOPR-backed study indicated that the course of treatment changed 43.1 percent. The most common changes involved switching to another chemotherapy agent 26.5 percent of the time or changing the current dose or duration of therapy 16.5 percent of the time.
There are also several groundbreaking trials on PET imaging independent of NOPR. In a study led by Fritz Eilber, M.D., assistant professor of surgery, assistant professor in molecular and medical pharmacology and director of the Sarcoma Program at UCLA’s Jonsson Cancer Center, researchers directly compared PET to CT scanning in evaluating response to treatment in sarcoma patients. According to Dr. Eilber, the study demonstrates that the change in activity by FDG-PET was much more sensitive and accurate at detecting people who responded to treatment than Response Evaluation Criteria in Solid Tumors (RECIST) using CT, which is the current standard of care.
In this study, eight sarcoma patients were scanned using PET/CT, treated, scanned again and lastly underwent surgery. “We compared the change in the PET to the change in the size [of the tumor] with how much of the tumor was dead. We had eight people who had what we considered a pathologic response, in which 95 percent of the tumor was killed. All eight were picked up by PET; only two of them were picked up by CT. So if those [two] patients were on a drug where you couldn’t take out the tumor, they could have been pulled off the drug, which could have been working,” Dr. Eilber explained.
A tool to assess whether a patient is responding to treatment, Dr. Eilber stressed, is critical in cases of advanced disease in which case surgery may not be an option. “Basically it keeps you from interpreting somebody who has responded to treatment but has not had a decrease in size as a non-responder. And currently, a lot of studies [indicate] that type of patient would get pulled off the study because the tumor didn’t meet the size criteria changes.” Dr. Eilber suspects that more of these types of studies will be conducted, which will look at PET in the management and treatment of other types of cancer. “They just haven’t been done to a certain degree because the PET/CT scanner is relatively new,” he noted.
High-Definition Hybrids
In line with growing utilization and demand for PET imaging, manufacturers continue to drive advancements in hybrid technology, particularly for PET/CT.
One of the buzzwords today in imaging is high-definition (HD). But beyond the hype, there are significant benefits that HD lends image quality; enough for Siemens Healthcare to introduce its latest PET/CT system, Biograph mCT, which includes advanced HD to create a new system that is capable of scanning the whole body in five minutes and allows for low dose scans.
“High-definition PET enables improved delineation of small and early lesions, especially lesions without very high tracer uptake due to the improved resolution and higher lesion contrast obtained by HD and ultraHD technology,” said Partha Ghosh, M.D., clinical marketing manager, molecular imaging, Siemens Healthcare. “Thus patients with small metastases, early tumor recurrence especially in regions with distorted anatomy following surgery or radiotherapy and metastases with lower tumor burden causing it to have low FDG uptake are better visualized with HD and ultraHD technology.” UltraHD technology combines time-of-flight (TOF) and point-spread-function (PSF) reconstruction and offers 2-mm uniform resolution throughout the entire field of view (FOV) and 4 times enhanced lesion contrast compared to standard PET scans.
He added, “This should help early diagnosis of metastases and tumor recurrence and evaluation of treatment follow up since visualization of small residual disease would otherwise be missed and would have a major impact on further treatment decision.”
According to Siemens, with Biograph mCT, a facility may only need to purchase one imager instead of two, representing a huge cost-savings potential in a time when healthcare budgets are tight.
With oncology applications representing more than 90 percent of clinical PET/CT exams, GE Healthcare integrated its BrightSpeed CT with the motion management capabilities of its Discovery PET system to create the Discovery PET/CT 600. The system is optimized for use in oncology and is capable of managing and correcting for motion during a scan. As a key component of the image chain, the Discovery PET/CT 600 includes a scintillator with high sensitivity level available, and GE BGO technology said to allow for improved lesion detectability, potentially reducing the dose requirement and allowing for faster scans and increased throughput.
As new technology continues to enhance the image quality of PET/CT, and studies demonstrate the clinical efficacy of the system, the medical community is building its case for why Medicare should expand reimbursement for PET, and so far, it is a convincing one.
Reference:
NOPR is sponsored by the Academy of Molecular Imaging (AMI), and managed by the American College of Radiology (ACR) and ACR Imaging Network (ACRIN). The registry received input from—and is endorsed by—ACR, the American Society for Clinical Oncology (ASCO) and the Society of Nuclear Medicine (SNM). The NOPR Working Group was chaired by Bruce Hillner, M.D., of Virginia Commonwealth University and co-chaired by Barry Siegel, M.D., Washington University; R. Edward Coleman, M.D., Duke University; and Anthony Shields, M.D., Wayne State University.


 May 27, 2026
May 27, 2026