February 26, 2015 — Approximately 8 to 12 million people in the United States alone are suffering from peripheral arterial disease (PAD), a common vascular problem that is also one of the most serious complications of diabetes. Andreas Hielscher, professor of biomedical engineering, electrical engineering and radiology (physics) at Columbia Engineering, is developing a novel technology that could improve diagnosis of this crippling disease and make it easier to monitor patients.
Hielscher and his team received a $2.5 million, five-year grant from the National Heart, Lung and Blood Institute (NHLBI) to build and test a noninvasive, external. dynamic optical tomographic imaging system. This system uses near-infrared light to map the concentration of hemoglobin in the body’s tissue and reveal how well blood is perfusing patients’ hands and feet.
“We believe our new vascular optical tomographic imaging (VOTI) system will revolutionize the way we diagnose and monitor peripheral artery disease,” said Hielscher, who leads an interdisciplinary team of Columbia engineers, radiologists and vascular surgeons. He and his colleagues have been working on this research for the last three years, testing a prototype system in clinical pilot studies.
Because most patients are asymptomatic and there is no single reliable screening method, PAD is considerably under-diagnosed. Most of the undiagnosed and untreated patients are diabetics who commonly suffer from peripheral neuropathy and therefore do not sense and report symptoms that are early signs of the disease.
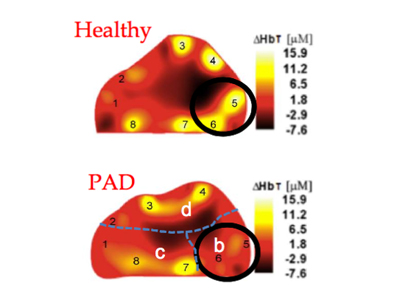
Hielscher hopes to remedy that with his VOTI system, which relies on near-infrared light that is shone onto different locations on a patient’s foot. Transmitted light intensities are then used to generate spatially resolved maps of oxy- and deoxy-hemoglobin, the two main components of blood.
“We’ve successfully used the VOTI to detect PAD in the lower extremities,” said Michael Khalil, a Ph.D. student working in Hielscher’s Biophotonics & Optical Radiology Laboratory. “Unlike other methods, our VOTI technology can provide maps of oxy-, deoxy-, and total hemoglobin concentration throughout the patient’s foot and identify problematic regions that require intervention.”
The results of the team’s latest study, involving 20 patients and 20 healthy volunteers, were recently published in the European Journal of Vascular and Endovascular Surgery.
Hielscher plans to use the NIH funding to build upon research previously funded by a Translational Research Grant from the Wallace H. Coulter Foundation and develop a new prototype and test the technology in a larger clinical study.
Hielscher also is working with the New York City Partnership (NYCP) fund to commercialize certain aspects of this technology. He has received funding through NYCP’s Bioaccelerate program to develop a commercially viable device that can be used intra-operatively and guide interventions by vascular surgeons. Monitoring wound healing is another promising applications of this technology. His team has already filed a broad patent application and believes that a commercial device could be available within two years.
For more information: www.bme.columbia.edu


 May 27, 2026
May 27, 2026