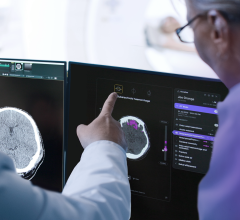
In most medical specialties, the main use of clinical decision support is to quickly determine what is the most appropriate type of imaging exam for a patient with specific symptoms.
In an era of healthcare reform and a push to meet appropriate use guidelines for tests, imaging and therapy amid declining reimbursements, there has been much discussion about implementation of clinical decision support (CDS) software. There is apprehension by some physicians who view CDS as technology telling doctors how to practice medicine. There are others in healthcare who are concerned about adding cost with the implementation of this software and how it will be updated based on the most current clinical data and practice guidelines. However, if implemented in a way where it is integrated with workflow and accepted by the physicians and hospital leadership, CDS has helped some hospitals meet appropriate use criteria and reduce unnecessary tests, which in turn helped reduce healthcare costs.
CDS is supposed to help clinicians do more with less by identifying at-risk patients and eliminating inappropriate procedures, and also help physicians adhere to practice guidelines. It is unreasonable to expect physicians to remember hundreds of pages of ever-changing appropriate use criteria (AUC), which is where CDS can offer an instant resource. In addition, it records data that can be mined for information, such as benchmarking to target education and quality improvement, or to see patterns of use.
Healthcare reform initiatives include payment incentives for hospitals that provide better healthcare. Most of these incentives have been for hospitals leveraging information technology in a meaningful way to better manage patient care. An electronic medical record (EMR) by itself does not mean better care any more than a good road means no accidents. Similar to the adoption of GPS by motorists, CDS can help healthcare providers navigate complex care situations and improve outcomes. CDS does not replace skilled clinicians, but like a GPS, it can help them take the best route to their desired destination.
Stage 2 meaningful use requirements for EMRs, released in August 2012, call for physicians to use some form of clinical decision in their practice. It was left intentionally vague so physicians could find software that best meets their needs. This requirement has brought CDS to the forefront of health IT.
“Healthcare providers are increasingly under pressure to make appropriate clinical decisions, document those decisions and do so efficiently,” said V. Katherine Gray, Ph.D., president, CEO and founder of Sage Health Management Solutions, a provider of CDS software. “With the recent economic pressures, patients, payors and the government are demanding more accountability in managing the costs and value of all healthcare services, especially in the burgeoning diagnostic imaging services.”
CDS for Radiology
In radiology, the main use of clinical decision support is to quickly determine what type of imaging exam or diagnostic testing is needed for a patient with specific symptoms. The software is based on AUC set by various medical societies, including the American College of Radiology (ACR). Some societies are beginning to produce software to help keep clinicians stay up-to-date on the criteria and make it easier for them to implement these standards.
The American College of Cardiology’s Imaging in FOCUS initiative is aimed at reducing inappropriate use of diagnostic imaging through the use of CDS software to track AUC. As a measure of success, participating practices have been able to reduce inappropriate ordering by close to 50 percent in one year (from 12 to 7 percent).[1]
The ACR’s AUC is now available in a digital format that can be incorporated into computerized ordering and EMRs. ACR entered into an agreement with the National Decision Support Company (NDSC) to provide the technical platform, support and licensing of the app under the name ACR Select.
NDSC will provide EMR vendors with a direct method to integrate ACR AUC guidelines. The software offers a CSD support database with more than 130 topics and 614 variant conditions that provide evidence-based guidance for the appropriate use of all imaging procedures. More than 300 volunteer physicians, representing more than 20 radiology and non-radiology specialty organizations, participate on the ACR expert panels to continuously update these guidelines.
“ACR Select will have a substantial impact on the healthcare community by bridging the gap between medical providers and the ACR appropriateness criteria guidelines,” said Paul H. Ellenbogen, M.D., FACR, chair of the ACR Board of Chancellors. “The commitment from major EHR technology providers to integrate these standards is a testament to the importance of promoting appropriate medical imaging use.”
ACR said its software will enable physicians to order the right imaging examination at the right time and can improve quality, reduce unnecessary scans and lower imaging costs.
Choosing Appropriate Imaging Exams
Healthcare IT vendors have developed CDS that integrates with EMRs and includes benefits managers and insurance companies to ensure payment for appropriate procedures. These systems also combine guidelines from multiple sources into one location.
Sage Health Management Solutions (Sage HMS) offers RadWise, which provides evidence-based CDS to guide clinicians to the most appropriate imaging decision based on each patient’s symptoms. It also documents the diagnosis and procedures, and records the current imaging recommendation regardless of what was ordered. RadWise CDS can help organizations improve quality by determining the most appropriate imaging, eliminating unnecessary or redundant tests, monitoring radiation exposure and documenting outcomes.
Epic Imaging, an outpatient diagnostic imaging center in Portland, Ore., recently integrated RadWise radiology reports into the center’s EMR. “Using RadWise will allow our radiologists to document the appropriate imaging for patients, collect data about the outcomes, and test an alternative to the cumbersome prior authorization process to demonstrate that the workflow does not have to be altered for referring physicians,” said John Griffith, CIO and director of operations.
Emerge developed CDS software to check AUC for cardiac nuclear imaging. It evaluates variables in a patient’s EMR to decide if sending them for a perfusion exam meets the guidelines.
“It just shows you if it’s appropriate or not,” said William Daniel, M.D., director of quality control at Mid-America Heart Institute, Kansas City, Mo., and CMO of Emerge. “It’s not for the differential diagnosis, it’s about helping the clinician to meet the appropriate use criteria. It’s not about telling them how to practice medicine.
Tips For What is Needed in CDS Software
Daniel, the physician who developed the company’s signature diagnosis software suite and stayed on with Emerge as chief medical officer, shared several points clinicians should consider when shopping for CDS systems. “For clinical decision support to be used and be effective, it must be integrated into the workflow. It has to make sense and not require all sorts of extra pointing and clicking,” Daniel explained. “It has to work seamlessly. Everyone today is just too busy to deviate from their workflow.”
Along with society guidelines, each hospital has its own set of protocols, so CDS software needs to be customizable. “It needs to be very flexible. It has to be useful,” Daniel said.
CDS software can be hosted on a hospital’s server or on a cloud server. The advantage of a cloud server is it can be easily accessed anywhere through an encrypted connection. It also allows for easier updates of guidelines or reimbursement rules.
In addition to offering decision support, a system should offer feedback reports. It should be customizable to analyze each physician to see if they met AUC. If the system identifies many cases where the criteria were not met, Daniel said it may not be a problem with the doctor, but an issue with the guidelines.
“I think what you are going to see is once people begin to use the software to meet meaningful use, they will want to take it a step further,” he explained.
Daniel said the software can help document everything to remove interim steps to care, such as case review boards or pre-certification of a procedure. It also can better guide physicians to more closely align their care to the guidelines, which may improve patient outcomes.”
CDS as a Second Set of Eyes
MDDX offers Smart Read for real-time guidance while interpreting medical images. It has an integrated report engine that checks each answer put into the system against a database of common pitfalls, acceptable averages (i.e., radiation dose) and clinical correlations. It also checks for inconsistencies between the physician’s interpretation and the patient’s previous medical history. Smart Read aggregates expert wisdom into easy-to-understand points that are displayed during image interpretation.
The system’s cardiac computed tomography (CT) angiography report engine incorporates 160 expert rules derived from the world’s top cardiac CT luminaries. Their advice helps flatten the learning curve and ensures physicians are up-to-date with the latest trends.
“In contrast to most CDS systems, which aim at physicians’ education, this is a CDS that integrates radiology benefits managers and insurance companies,” said James Min, M.D., FSCCT, associate professor of medicine, Cedars-Sinai Medical Center, and director of cardiac imaging research. “The goal of this type of CDS is that it reduces the need for prior authorization by taking guideline-based evidence, expert opinion and peer-based ordering and reducing the need for cardiologists or radiologists from having to interact with RBMs. Given Obamacare, and the trend toward accountable care organizations, this type of CDS will be a huge advance to saving cardiologists and radiologists a lot of headaches with prior authorization, while ensuring that doctors can perform physician-preferred, rather than insurance dictated, medicine.”
CDS Market Impact
KLAS published a report on CDS, “Clinical Decision Support 2011 — Understanding the Impact,” in November 2011, which provides an industry overview of where things are at with adoption and trends.
Healthcare initiatives include payment reform that incentivizes providers to provide better healthcare. Most of these incentives so far have been for hospitals leveraging information technology in a meaningful way to better manage patient care.
KLAS conducted a perception study to find out what CDS solutions providers were using. KLAS interviewed 404 providers about their CDS tools’ performance to understand the impact those tools are having. Providers said using CDS to create order sets was the most impactful software support. Order sets and care plans were rated highest for standardizing care across organizations, though lower for their impact on clinical decisions. KLAS found many providers view order sets and care plans as reflections of decisions already made or known, rather than tools for making on-the-fly clinical decisions.
Standardization is seen as a way to channel management of standard problems through evidence-based guidelines. However, KLAS said some of its respondents expressed concern about standardized care becoming “cookbook medicine,” and emphasized that healthcare still requires trained clinicians doing critical thinking. Providers indicated that changing cultures and gaining consensus was often the most challenging part of getting to a standard, and that the evidence and tools in order sets and care plans made that process easier.
Few provider organizations have measured the impact of their CDS tools on actual outcomes. Most providers are optimistic, but responses on positive outcomes were often anecdotal, so more data needs to be collected.
KLAS reports workflow integration is currently the biggest Achilles’ heel of CDS tools. The report said the software needs to be better integrated into EMRs and seamlessly integrate into workflows. As an example, KLAS points out drug databases are often integrated into EMRs, but they are not connected to the clinician workflow, requiring extra clicks to search something. If something takes additional clicks outside a standard workflow, many people will not use it.
Surveillance CDS scored high in most areas of the KLAS report, but its overall impact is limited by the low adoption rate. As these tools spread, their impact could become a standard-of-care, KLAS predicts.
Reference:
Implementation of Clinical Decision Support in the Real World
Brigham and Women’s Hospital in Boston conducted a pilot study of a Web-enabled computerized physician order entry (CPOE) system (another Stage 2 requirement) with embedded imaging decision support. In an effort to reduce the inappropriate use of medical imaging and improve quality of care, it was phased into clinical use between 2000 and 2010 across outpatient, emergency and inpatient departments. The study, published in the Journal of the American College of Radiology in February 2012, showed significant increases in meaningful use for electronically created studies (from 0.4 percent to 61.9 percent) and for electronically signed studies (from 0.4 percent to 92.2 percent) and the adoption of CPOE (from 0.5 percent to 94.6 percent).
A total of 4.1 million imaging studies were performed during the study period. The use of electronically created studies was greatest in the emergency department and inpatient settings. Meaningful use varied across specialties; surgical subspecialties had the lowest rates of electronically created studies.
“Our study shows that an imaging CPOE system with embedded decision support that is integrated into the healthcare enterprise IT infrastructure and the relevant electronic medical record platform and optimized within the clinicians’ workflow can be successfully and broadly accepted clinically,” said Ivan K. Ip, M.D., MPH, lead author of the study.
CDS was not wholeheartily embraced by everyone at the hospital, said Ramin Khorasani, M.D., radiology, Brigham & Women’s Hospital, Harvard Medical School, when he spoke about the software at SIIM 2012. He said it took time to get people to buy in to decision support and accountability, explaining people did not want to change, or do something new, especially when it is a significant change for a radiology practice. He offered advice to hospitals looking at adopting CDS.
Khorasani said the quality of the evidence used by the CDS matters. He said Brigham & Women’s gives scores to the evidence (it does not matter who published it) to say how valuable it is, before they accept it and put it into the system.
There are instances when there is evidence both for and against something, which can lead to confusion if entered both ways into a CDS system. “When something isn’t clear, we don’t put it in,” Khorasani said. “Then we turn to local best practices. We don’t put something in just because it’s published by one group or another. We leave controversial stuff aside.”
The system uses evidence-based guidelines from the various societies, which are updated continuously to keep the CDS current. The lag time from publication to updates in the system is between four to six weeks.
Effective decision support also must be accompanied by accountability. Brigham & Women’s now requires physicians to sign all orders electronically. “We are going to embarrass you, and make you think twice about ordering an exam,” Khorasani said.
Brigham & Women’s CDS tool is not something on the side, it is part of the medical record, he said. Part of the reason for this is to record everything and make physicians accountable and guarantee they do not ignore clinical evidence.
Khorasani also said a broad collaboration is needed, from those in the front lines using the system, up through to the upper management. “Adoption of evidence-based imaging health information technology needs leadership, too. You must have buy-in and encouragement from the top in order for it to succeed,” he explained.
Finally, he advised using the data collected by the system to measure everything. This will help quantify successes and help identify issues that need to be addressed.
—By Helen Kuhl

 May 22, 2024
May 22, 2024