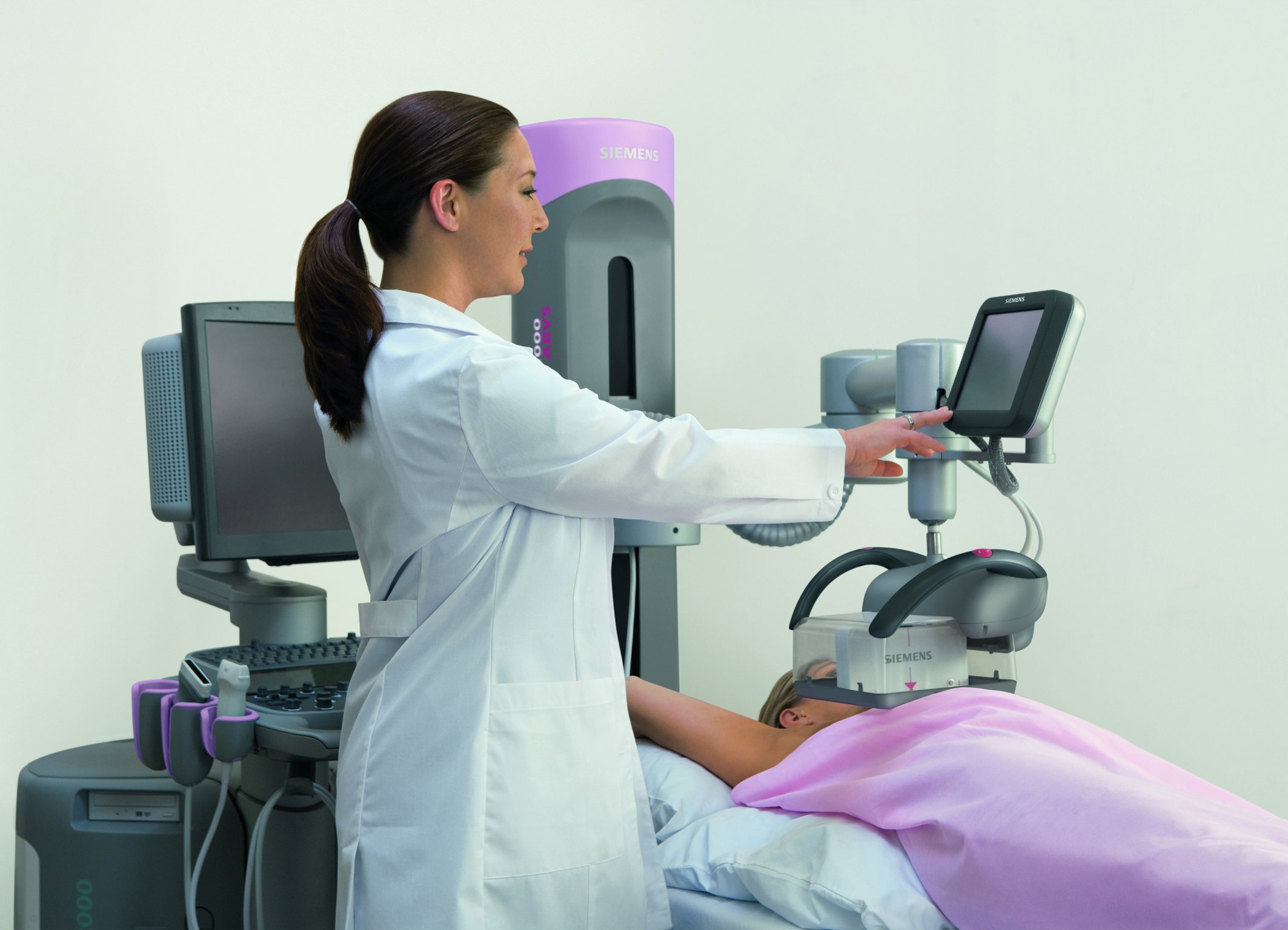
The multi-use ultrasound breast system Acuson S2000 Automated Breast Volume Scanner (ABVS) from Siemens Healthineers automatically acquires volume images of the breast. Photo courtesy of Siemens.
Research shows that automated breast ultrasound (ABUS) is a strong companion to traditional mammography, particularly for patients with dense breast tissue. The comprehensive scan provides a better interpretation than traditional mammography, enabling radiologists to catch cancers that might not otherwise be visible.
What is ABUS?
Automated breast ultrasound (ABUS) is a comprehensive breast scanning system that uses high-frequency sound waves to produce a 3-D volumetric image of the entire breast. The 3-D image allows radiologists to check the breast from multiple angles, which may reveal tumors that were invisible or difficult to find in 2-D mammography.
Using traditional ultrasound, exams can take up to 30 minutes and are highly impacted by the operator’s skill level due to the device’s handheld transducer. ABUS solves both of these problems by automatically scanning the breast in as little as seven minutes with some systems.
The U.S. Food and Drug Administration (FDA) first approved an ABUS system as an adjunct to mammography for asymptomatic patients with dense breast tissue in 2012. The somo•v ABUS system from GE Healthcare was soon followed by others, and today ABUS is a leader in the movement toward personalized breast screening and patient-first care.
How Does ABUS Work?
Traditional ultrasound uses a handheld transducer to both emit ultrasound waves and detect the ultrasound waves that are reflected back. Radiologists apply gel to the skin to prevent air pockets from forming between the skin and the transducer, which block ultrasound waves from passing through the body. The sound waves bounce off of tissues, and the differences between the reflections are analyzed by software and used to create a 2-D image.
ABUS systems work similarly, but eliminate user error by automating the scan. GE Healthcare’s Invenia ABUS system, for example, uses a transducer that is lowered onto the patient’s breast by the radiologist, who properly positions the patient and applies an ultrasound lotion to the breast. Hitachi’s Sofia system has the patient lie prone on a large, table-like transducer. The jelly or lotion is applied directly to the transducer’s screen rather than to the breast itself.
When an ABUS system is done scanning, it produces a 3-D volumetric image of the entire breast. This image includes the coronal view, which is not traditionally used in breast imaging, and other angles that may reveal tumors not visible in mammographic images of dense breasts.
While mammography is still the standard of care when it comes to breast cancer screenings and is proven to reduce deaths due to breast cancer, it may not be enough for patients with dense breast tissue. The FDA began approving ABUS devices in 2012 because they enabled radiologists to find 30 percent more cancers in these patients than with mammography alone. One study, published in the New England Journal of Medicine, showed 35 percent of breast cancer goes undetected by mammography in women with dense breasts, as density masks the appearance of tumors.1 In addition to making breast cancer more difficult to find, dense breast tissue increases the risk of breast cancer by four to six times.
But for all its benefits, ABUS systems still come with some drawbacks, particularly for radiologists. The 3-D view that makes ABUS so different is also what makes it so challenging — radiologists are forced to approach reading time in a whole new way. Additionally, using ABUS systems requires radiologists to learn new ways to position the patient, as well as make workflow adaptations.
Though the adjustments can initially lead to increased recall rates and reading times, both can be potentially reduced by half after being trained on ABUS systems and getting used to them.
How Does ABUS Help Patients?
A recent study presented at the 2017 annual meeting of the Radiological Society of North America (RSNA) showed that women prefer to get mammograms annually rather than biennially because the scans reduce anxiety about cancer development. However, the 40 percent of women age 40 and older who have dense breast tissue do not receive this same anxiety-reducing benefit, since mammograms miss about
35 percent of these patients’ cancers.2
ABUS not only contributes to higher numbers of correct diagnoses, but also reduces women’s anxiety about breast cancer and their own healthcare. “It gives women a peace of mind that they’re doing something additional for themselves if they have dense breast tissue,” said Silaja Yitta, M.D., director of breast imaging and intervention at El Camino Hospital Breast Health Center in San Jose, Calif.
Breast tissue density, the ratio between fibrous or glandular tissue and fat in the breast, is determined by the appearance of breast tissue on a mammogram. Having dense breast tissue is defined as falling into either category 3 (heterogeneously dense) or 4 (extremely dense) of the American College of Radiology’s Breast Imaging-Reporting and Data System (ACR BI-RADS). The fibrous tissue appears white on mammograms — just like tumors. This is where ABUS systems help distinguish what is abnormal tissue.
Because dense tissue increases a patient’s cancer risk and makes cancer more difficult to spot, some states have laws or education programs in place regarding breast density. Thirty-one states require notifying patients about breast density; five states have efforts for breast density reporting and education without notification; and six states provide insurance coverage for dense breasts.
Newest Clinical ABUS Research
Clinical studies have shown just how much ABUS systems aid in cancer diagnosis.
An April 2015 study acknowledged the difficulty radiologists can have reading ABUS scans. It found that despite “considerable inter-observer variability,” all radiologists had improved diagnostic performance when examining both ABUS and mammography scans. Additionally, they found that shadowing from the dense tissue was the most common cause of false positive ABUS interpretations. The study concluded that combined reading of ABUS and mammography scans should be standard if ABUS is implemented in screening of patients with dense breasts.3
Another 2015 study found several critical advances in knowledge and implications for patient care. Twenty-eight of the 30 cancers detected with ABUS (93.3 percent) were invasive, compared to 51 of 82 (62.2 percent) detected with mammography alone. The study concluded that “Clinically important cancers are detected with the addition of ABUS compared with screening mammography alone,” and that “improved detection through the use of ABUS supplemented to screening mammography alone has the potential to lead to earlier treatment and better prognosis in patients with dense breasts.”4
A study analyzing false-negative reading of ABUS images found that several things may make reading the images difficult.5 According to the 2017 study “Analysis of false-negative readings of automated breast ultrasound studies,” the image resolution can be diminished by “imperfect transducer-breast contact.” It also found, as did the 2015 study, that fibrous breast tissue can cause shadowing artifacts in images. Lastly, blind spots in ABUS imaging may cause lesions to be missed. The study concludes, however, that reader training and experience may be critical to managing these issues.
Research on ABUS systems is ongoing as well. The “Diagnostic Performance of an Automated Breast Ultrasound System (ABUS): a Single Centre Study,” first posted in January 2016 and currently in recruitment status, intends to evaluate the diagnostic performance of a new ABUS system in four different population groups:
- Population A: Women undergoing screening for familial or genetic predisposition for breast cancer.
- Population B: Women with newly diagnosed breast cancer. ABUS performance will be compared to breast magnetic resonance imaging (MRI) in the pre-operative assessment of breast cancer extent.
- Population C: Women with BI-RADS 3 or 4 lesions in a routine breast imaging examination. ABUS will be evaluated as a problem-solving tool.
- Population D: Women undergoing breast MRI for the assessment of breast implant integrity. ABUS performance will be compared to breast MRI.
This observational study has an estimated primary completion date of January 2021.
Delphinus announced in September 2017 the launch of its SoftVue Discover Breast Ultrasound Prospective Case Collection project. The project will enroll 10,000 asymptomatic patients with dense breast tissue who will undergo screening digital mammography in addition to SoftVue 3-D whole breast ultrasound exams. The study seeks to determine the effectiveness of detecting additional cancers with SoftVue that are not seen with mammography alone.
More information on ABUS systems currently on the market can be found at http://bit.ly/2GoRfKR.
Emily Clemons is a Florida State University alumna and current master’s candidate at Northwestern University’s Medill School of Journalism.
References
1. “Mammographic Density and the Risk and Detection of Breast Cancer.” NEJM. http://www.quantason.com/pdf/Mammographic_Density_and_the_risk_of_Breas…, Jan. 18, 2007.
2. “Women Prefer Getting Mammograms Every Year.” www.itnonline.com, Jan. 9, 2018.
3. Skaane P., Gullien R., Eben E.B., et al.“Interpretation of automated breast ultrasound (ABUS) with and without knowledge of mammography: a reader performance study.” Acta Radiologica, April 1, 2015. https://doi.org/10.1177/0284185114528835
4. Brem R.F., Tabar L., Duffy S.W., et al. “Assessing Improvement in Detection of Breast Cancer with Three-dimensional Automated Breast US in Women with Dense Breast Tissue: The SomoInsight Study.” Radiology, March 2015.https://doi.org/10.1148/radiol.14132832
5. Grubstein A., Rapson Y., Gadiel I., Cohen M. “Analysis of false-negative readings of automated breast ultrasound studies.” Journal of Clinical Ultrasound, March 13, 2017. DOI: 10.1002/jcu.22474


 May 07, 2026
May 07, 2026 









