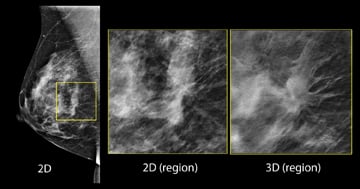
Imaging comparison between 2-D and 3-D. Tomosynthesis allows radiologists to view slices of the breast.
Data from a new study of more than 170,000 examinations using 3-D mammography (breast tomosynthesis) screening technology finds significantly more invasive cancers than a traditional 2-D mammogram. The researchers also found that 3-D mammography reduces the number of women called back for unnecessary testing due to false alarms. The study was published in the June 25, 2014, issue of the Journal of the American Medical Association (JAMA).
Benefits of Tomosynthesis
Traditional 2-D screening mammography has played a key role in reducing breast cancer mortality, although it has drawn criticism for excessive false-positive results, limited sensitivity and the potential of over-diagnosis of clinically insignificant lesions. Tomosynthesis, however, allows for 3-D reconstruction of the breast tissue, giving radiologists a clearer view of the overlapping slices of breast tissue. And though a relatively new technology, it has shown promise at reducing recall rates in all groups of patients, including younger women and those with dense breast tissue, and better detection rates in smaller studies. Single-institution studies have shown that adding tomosynthesis to mammography increases cancer detection and reduces false-positive results, but this is one of the first large-scale multi-center studies showing the benefit of tomosynthesis.
“We believe this study is groundbreaking because of the sheer number of mammograms we reviewed,“ said lead author Sarah Friedewald, M.D., co-medical director of the Caldwell Breast Center at Advocate Lutheran General Hospital, Park Ridge, Ill. “Because it is 10 times larger than other studies to date, and because the data came from both academic and community healthcare settings, we think it tells a compelling story about the effectiveness of 3-D mammography.”
Women will see little difference in the 3-D mammography exam, which takes just a few seconds longer than traditional 2-D mammography. But, what radiologists reading the exams see is different. Like the pages of a book, it allows the physicians to see through the layers of the breast and diagnose potential problems more quickly.
“The Caldwell Breast Center at Lutheran General Hospital was the first in the Midwest to purchase 3-D mammography,” Friedewald said. “All of our patients have the opportunity to receive 3-D exams because we believe the technology is saving lives.”
The Study
Friedewald and colleagues conducted a study using data from 13 centers to determine if mammography combined with tomosynthesis improves performance of breast screening programs. A total of 454,850 examinations (n = 281,187 digital mammography;
n = 173,663 digital mammography plus tomosynthesis) were evaluated.
The primary measured outcomes were recall rate (proportion of patients requiring additional imaging based on a screening examination result), cancer detection rate, positive predictive value for recall (proportion of patients recalled after screening who were diagnosed as having breast cancer) and positive predictive value for biopsy (proportion of patients undergoing biopsies who were diagnosed as having breast cancer).
An analysis of the data indicated that the model-adjusted rates per 1,000 screens were as follows: for recall rate, 107 with digital mammography vs. 91 with digital mammography plus tomosynthesis (an overall decrease in recall rate of 16 per 1,000 screens); for biopsies, 18.1 with digital mammography vs. 19.3 with digital mammography plus tomosynthesis; for cancer detection, 4.2 with digital mammography vs. 5.4 with digital mammography plus tomosynthesis; and for invasive cancer detection, 2.9 with digital mammography vs. 4.1 with digital mammography plus tomosynthesis.
Adding tomosynthesis increased the positive predictive value for recall from 4.3 to 6.4 percent and for biopsy from 24.2 to 29.2 percent.
“It’s the most exciting improvement to mammography that I have seen in my career, even more important for women than the conversion from film-screen mammography to digital mammography,” said senior author Emily F. Conant, M.D., chief of breast imaging at the department of radiology at the Perelman School of Medicine, University of Pennsylvania. “3-D mammography finds more clinically significant breast cancers earlier, which is the key so that women have more treatment options and ultimately better health outcomes.”
Other Significant Findings
The authors wrote that the success of mammography screening in reducing mortality is predicated on the principle of detecting and treating small, asymptomatic cancers before they have metastasized. Accordingly, the preferential increase in invasive cancer detection with addition of tomosynthesis may be of particular value in optimizing patient outcomes from mammography screening. They said the association with fewer unnecessary tests and biopsies, with a simultaneous increase in cancer detection rates, would support the potential benefits of tomosynthesis as a tool for screening. However, assessment for a benefit in clinical outcomes is needed.
Significant findings include:
•A 41 percent increase in the detection of invasive breast cancers (p<.001).
•A 29 percent increase in the detection of all breast cancers (p<.001).
•A 15 percent decrease in women recalled for additional imaging (p<.001).
•A 49 percent increase in positive predictive value (PPV) for a recall (p<.001). PPV for recall is a widely used measure of the proportion of women recalled from screening that are found to have breast cancer. The PPV for a recall increased from 4.3 to 6.4 percent.
•A 21 percent increase in PPV for biopsy (p<.001). PPV for biopsy is a widely used measure of the proportion of women having a breast biopsy that are found to have a breast cancer. The PPV for a breast biopsy increased from 24.2 to 29.2 percent.
•No significant change in the detection of ductal carcinoma in situ (DCIS). DCIS is a non-invasive cancer. It has not spread beyond the milk duct into any normal surrounding breast tissue.
Currently the only U.S. Food and Drug Administration (FDA)-cleared tomosynthesis system is the Selenia Dimensions from Hologic, which was launched in the U.S. market in February 2011. “The JAMA 3-D study validates the findings of previously published studies but on a much larger scale,” said Peter J. Valenti III, Hologic division president, breast health. “The study addresses the two most frequently cited concerns with breast cancer screening — that we are finding too many cancers that don’t need to be treated and that too many women are being called back for unnecessary additional testing. Each of the outcomes measured was statistically significant and reinforced the benefits of Hologic 3-D mammography in addressing these challenges.”
Five leading academic hospitals participated in the study: Massachusetts General Hospital; Yale University School of Medicine in Connecticut; University Hospitals Case Medical Center in Ohio; Albert Einstein Healthcare Network; and the Perelman School of Medicine of the University of Pennsylvania in Pennsylvania. Eight community-based sites participated in the study: Caldwell Breast Center of Advocate Lutheran General Hospital in Illinois; TOPS Comprehensive Breast Center in Texas; Washington Radiology Associates, PC in Washington, D.C.; Radiology Associates of Hollywood and Memorial Healthcare System in Florida; Evergreen Health Breast Center and Radia Inc., PS in the state of Washington; Edith Sanford Breast Health Institute in South Dakota; Invision Sally Jobe Breast Centers and Radiology Imaging Associates in Colorado; and John C. Lincoln Breast Health and Research Center in Arizona.



 May 22, 2026
May 22, 2026 









