WEBINAR: Advances in CT to Enhance Radiation Therapy Planning
This webinar is sponsored by Philips Healthcare
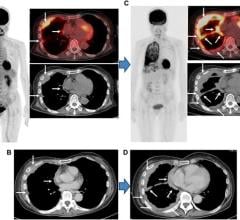
The webinar "Advances in Computed Tomography (CT) to Enhance Radiation Therapy Planning," will offer an overview of the use of CT simulation in radiation therapy and the technologies available to reduce image artifacts that may impact the quality of care.
The webinar took place June 7, 2017, and the archive version is available immediately when you register.
This webinar is sponsored by Philips Healthcare.
Statement of Purpose
CT simulation is the current standard of care for radiation therapy treatment planning due to its excellent geometric fidelity and relationship to material density required for dose calculation. However, image artifacts may be detrimental to treatment planning accuracy. This talk will describe the state of the art of CT artifact reduction, particularly for metal artifacts and potential impacts on radiation therapy planning. Furthermore, as we image more frequently for adaptive planning purposes and adhere to as low as reasonably achievable (ALARA) principles, dose reduction and image optimization without information loss is essential. Concepts such as incorporating advanced CT reconstruction algorithms such as iterative and model-based reconstruction will be discussed. The impact of using these algorithms in the context of radiation therapy will be described. Finally, consideration will be given to emerging CT applications on the horizon.
Learning Objectives
Upon completion of this activity, participants will be able to:
• Review causes of CT image artifacts and potential impacts on treatment planning.
• Explain the state of the art for metal artifact reduction technologies in CT and their potential impact on clinical treatment planning.
• Define typical CT doses in the context of radiation therapy.
• Discuss existing CT technologies to lower dose in image acquisition and examine the potential clinical impact in radiation oncology.
• Describe emerging CT applications under development and use in radiation oncology.
Intended Audience:
This activity is intended for radiation oncologists, medical physicists, dosimetrists, and all staff involved in imaging used for oncology treatment planning and simulation.
Speaker:
 Carri K. Glide-Hurst, Ph.D., DABR
Carri K. Glide-Hurst, Ph.D., DABR
Director of Translational Research
Henry Ford Health System
Glide-Hurst obtained her Ph.D. in medical physics from Wayne State University in 2007, focusing her efforts on breast ultrasound tomography and utilizing acoustic parameters for breast density evaluation. She then spent two years in postdoctoral training in the Department of Radiation Oncology at William Beaumont Hospital, with an emphasis on motion management techniques in lung cancer. She has since been at Henry Ford Health Systems in Detroit, where she currently holds the position of director of translational research. Her primary clinical and research focus includes the implementation of CT and MR simulation (MR-SIM) into radiation oncology and treatment planning. Glide-Hurst is the co-chair of AAPM Task Group 284 - Magnetic Resonance Imaging - Simulation in Radiotherapy: Considerations for Clinical Implementation, Optimization, and Quality Assurance. Glide-Hurst was awarded a five-year NIH R01 grant on the Development of Anatomical Patient Models to Facilitate MR-only Treatment Planning. She has published more than 35 peer-reviewed publications and about 100 abstracts related to imaging in radiation therapy.


 July 24, 2024
July 24, 2024