Image source: Blausen.com staff (2014). "Medical gallery of Blausen Medical 2014". WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436. [CC BY 3.0 (https://creativecommons.org/licenses/by/3.0)]
August 27, 2019 — A new Harvey L. Neiman Health Policy Institute study assesses temporal and patient-level differences in paracentesis and thoracentesis procedures performed on Medicare beneficiaries by radiologists and non-radiologists with respect to overall procedure volume, day of week and patient complexity. The study is published online in Journal of Vascular and Interventional Radiology.1
The researchers used Medicare patient-level claims data from 2004 to 2016 to study differences over time between radiologists and non-radiologists in the performance of paracentesis and thoracentesis procedures. They also investigated whether different specialties were more likely to perform these procedures on patients that are more complex or on weekends.
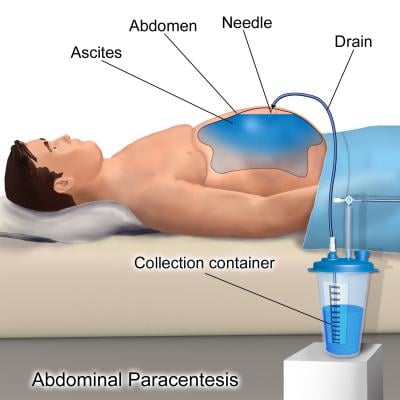
Paracentesis is a procedure used to investigate abdominal swelling where a needle or catheter is inserted into the peritoneal cavity to collect a fluid sample. The most common indication for paracentesis is the suspected presence of ascites, an accumulation of protein-containing fluid commonly caused by liver disease. The procedure can also be therapeutic in nature to help relieve pressure, pain and other symptoms caused by the abdominal swelling. Thoracentesis is a similar procedure used to remove excess air or fluid from the lungs. Ultrasound guidance is frequently used during both procedures.
“For both paracentesis and thoracentesis procedures, we observed an increase over time in the proportion of procedures performed by radiologists compared to non-radiologists,” said Ravi V. Gottumukkala, M.D., a radiology fellow at Massachusetts General Hospital. “Additionally, while for both procedures, radiologists increasingly perform the majority of services on both weekdays and weekends, we found that the proportion of the services provided by radiologists was greater on weekdays compared to weekends.”
Gottumukkala and his colleagues found that between 2004 and 2016, the proportion of all paracentesis procedures performed by radiologists increased from 70 percent to 80 percent, while thoracentesis procedures increased from 47 percent to 66 percent.
The results also showed that currently, both radiologists and non-radiologists perform paracentesis and thoracentesis procedures on similarly complex patients. However, “for a majority of the first nine years, radiologists performed paracentesis on more complex patients than non-radiologists, but patient complexity was similar during recent years. For thoracentesis, patient complexity was similar for both specialty groups across the study period,” noted Anand M. Prabhakar, M.D., MBA, a radiologist at Massachusetts General Hospital.
A separate JVIR study published earlier this year explored the safety of radiologist-performed, ultrasound-guided paracentesis procedures and found minimal risk of procedure-related complications in this setting. The researchers from Banner University Medical Center in Phoenix looked at more than 3,000 paracentesis procedures performed at the hospital over a two-year period, focusing on the number of patients that experienced a hemorrhage requiring blood transfusion or rescue angiogram and/or embolization. Ultimately, significant hemorrhage was found in only six patients (0.19 percent) and an emergency angiogram was only required for one patient.2
For more information: www.jvir.org
Reference
1. Gottumukkala R.V., Prabhakar A.M., Hemingway J., et al. Disparities over Time in Volume, Day of the Week, and Patient Complexity between Paracentesis and Thoracentesis Procedures Performed by Radiologists versus Those Performed by Nonradiologists. Journal of Vascular and Interventional Radiology, published online Aug. 14, 2019. https://doi.org/10.1016/j.jvir.2019.04.015
2. Rowley M.W., Agarwal S., Seetharam A.B., et al. Real-Time Ultrasound-Guided Paracentesis by Radiologists: Near Zero Risk of Hemorrhage without Correction of Coagulopathy. Journal of Vascular and Interventional Radiology, February 2019. https://doi.org/10.1016/j.jvir.2018.11.001


 March 30, 2026
March 30, 2026