January 4, 2010 - Patients demonstrated significant improvements in motor skills and brain function in a large-scale study conducted to measure the effectiveness of dopamine cell transplantation in Parkinson’s disease patients shows, according to research reported in the January issue of The Journal of Nuclear Medicine (JNM).
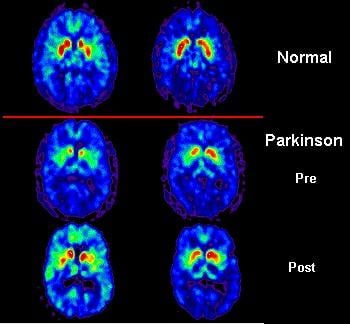
In the study, positron emission tomography (PET) played a critical role in assessing graft survival. The results of this study demonstrate that transplanted cells were viable and integrated well with the host brain tissue. Furthermore, these cells produced dopamine that helped support the brain and led to an improvement in motor symptoms. These improvements were sustained over a four-year study period.
"This study provided new insights into the time course of transplantation outcome," said David Eidelberg, M.D., study co-author and director of the Neuroscience Center at the Feinstein Institute for Medical Research in Manhasset, N.Y. "Comprehensive long-term clinical follow-up, together with molecular imaging, allows for a more realistic appraisal of this kind of intervention for Parkinson’s disease."
Researchers reported long-term clinical and imaging outcomes after transplantation from 33 patients who originally participated in a one-year, double-blind, placebo-controlled trial of embryonic dopaminergic cell implantation for Parkinson’s disease. Clinical improvement in motor ratings, as well as increased brain uptake of 18F-fluorodopa (18F-FDOPA), the radiotracer that is widely used to investigate the function of dopamine grafts, was evident at one, two and four years after the transplantation surgery.
According to the researchers, the findings in the study demonstrate the critical roles played by PET in screening patients for transplantation procedures and in objectively assessing graft survival over the long term.
"This work provides a valuable template for conducting imaging-based trials of cell transplantation for Parkinson’s disease and perhaps other neurodegenerative disorders," said Yilong Ma, Ph.D., lead author of the JNM study and associate investigator at the Feinstein Institute for Medical Research. "It offers guidance in the design of this type of trial, particularly with respect to the use of quantitative imaging as an adjunct to clinical assessments."
While there is presently no cure for Parkinson’s disease, a variety of medications provide dramatic relief from the symptoms. Novel surgical interventions such as cell transplantation and gene therapy are currently being investigated for patients with medically refractory symptoms.
Co-authors of "Dopamine Cell Implantation in Parkinson’s Disease: Long-Term Clinical and 18F-FDOPA PET Outcomes" include Yilong Ma, Chengke Tang, David Eidelberg, Vijay Dhawan, Thomas Chaly, Center for Neurosciences, The Feinstein Institute for Medical Research, Manhasset, N.Y.; Yilong Ma, Thomas Chaly, David Eidelberg, Vijay Dhawan, Departments of Neurology and Medicine, North Shore University Hospital and New York University School of Medicine, Manhasset, N.Y.; Paul Greene, Stanley Fahn, Department of Neurology, Columbia College of Physicians and Surgeons, New York, N.Y.; Robert Breeze, Department of Neurosurgery, University of Colorado School of Medicine, Denver, Col.; and Curt Freed, Neuroscience Center and Division of Clinical Pharmacology and Toxicology, University of Colorado School of Medicine, Denver, Col.
For more information: jnm.snmjournals.org.


 May 08, 2026
May 08, 2026 









