June 1, 2015 — Four World Health Organization (WHO) member states and nine non-governmental organizations (NGOs) co-organized a side event during the 68th session of the World Health Assembly (WHA) entitled “Imaging for Saving Kids - the Inside Story about Patient Safety in Pediatric Radiology." The International Society of Radiology (ISR) was one of the initiators of the side event.
The WHA is the supreme decision-making body of the WHO; the annual meeting in Geneva, Switzerland, is attended by delegations from the 194 WHO member states, the NGOs in official relations with the WHO and representatives from other United Nations (UN) agencies.
This event conducted at the United Nations Office at Geneva (UNOG), brought policymakers, healthcare providers, equipment manufacturers, and patients together to jointly discuss what could be done to improve health and service delivery by maximizing the benefits and minimizing the risks when using medical imaging in children and how this could be achieved.
Universal health coverage aims to ensure that all people obtain the health services they need without suffering from financial hardship. This outcome requires efficient health systems, suitable health financing approaches, access to essential medicines and technologies, and sufficient capacity of well-trained and motivated health professionals.
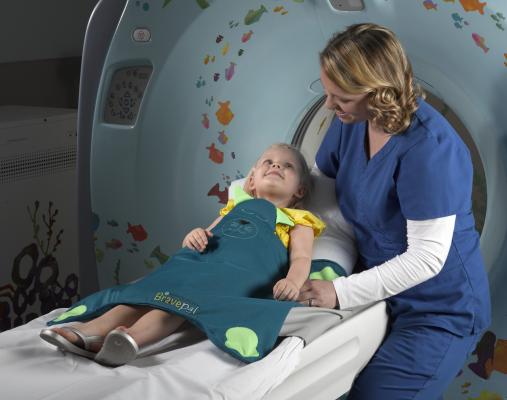
Medical imaging enables earlier diagnosis and offers less invasive treatment for sick children. Timely access to basic life-saving procedures, e.g. ultrasound and computed tomography (CT), is important. While resources vary between regions and settings, the stakeholders are improving access to these imaging procedures.
Children are more vulnerable to ionizing radiation-related health risks, e.g. X-ray exposure during CT scans. Whenever appropriate, medical imaging without ionizing radiation has to be used, e.g. ultrasound or magnetic resonance imaging (MRI). Good communication with the patient and carers facilitates informed decision-making and minimizes procedure delay or refusal due to unfounded concerns. Every procedure should be justified, tailored and optimised.
During the session, the participating stakeholders provided the perspectives of health professionals, patients, families and health authorities. The current situation in different regions, priorities and improvement opportunities were discussed.
Improvement in patient safety in pediatric radiology requires multidisciplinary teamwork, collaboration and an integrated framework for actions covering research, advocacy, education, infrastructure and evidence-informed policy. These actions will help to improve the performance of practitioners, facilities and healthcare systems. Some examples include: implementing the Radiation Basic Safety Standards (BSS) through national regulations; putting into practice the ten priorities identified in the Bonn call-for-action; taking into account the ICRP recommendations on radiation protection in medicine; increasing access to imaging procedures; improving appropriate use of pediatric imaging by policies, providing guidance and tools, and ensuring practitioner education and training; and promoting awareness of stakeholders’ roles and responsibilities.
It is important to foster an effective dialogue and build partnerships between health authorities, radiation protection regulatory bodies, practitioner organizations, equipment manufacturers, patients and families. Facility-based and system-wide actions are complementary for the establishment and maintenance of a radiation safety culture in pediatric imaging. Integration avoids duplication and promotes synergy.
For more information: www.isradiology.org

 May 28, 2026
May 28, 2026 









