March 13, 2018 – HeartFlow, Inc. today announced that it has entered into a licensing and technology transfer agreement with Cedars-Sinai in Los Angeles for AutoPlaque technology, a software tool used to detect and characterize coronary artery plaque based on coronary computed tomography angiography (CCTA) images. HeartFlow plans to use the AutoPlaque technology in its efforts to provide plaque assessment in future products, providing physicians with more information to help diagnose patients with coronary artery disease (CAD) and determine optimal treatment pathways.
The assessment of vulnerable plaque – lesions in coronary arteries that have the potential to rupture and cause acute coronary syndrome (ACS) – is an important area of clinical research. Results of the EMERALD (Exploring the MEchanism of the plaque Rupture in Acute coronary syndrome using coronary CT angiography and computationaL fluidDynamics) study, which were presented at EuroPCR 2016, demonstrated that the HeartFlow® FFRct Analysis, together with an assessment of coronary plaque, may help predict which coronary plaques are most likely to rupture. The HeartFlow FFRct Analysis is a first-of-its-kind non-invasive technology that provides a personalized 3D model of the heart to help clinicians diagnose and treat patients with suspected coronary artery disease (CAD).
“In addition to assessing lesion-specific physiology, understanding and characterizing coronary artery plaque is important in determining the most appropriate treatment path for patients with suspected CAD. The power of utilizing the AutoPlaque tool in the HeartFlow Analysis may accelerate our ability to analyze and characterize plaque in coronary arteries,” said John H. Stevens, M.D., president and chief executive officer, HeartFlow.
CAD, which today affects 16.8 million Americans, develops when the coronary arteries narrow, reducing blood flow to the heart and causing angina (chest pain), myocardial infarction (heart attack) and death. Acute Coronary Syndrome (ACS) is a life-threatening condition that occurs due to decreased blood flow to the heart, often because of a sudden rupture of plaque inside a coronary artery. ACS encompasses both unstable angina and myocardial infarction. In the United States, an ACS occurs every 25 seconds and someone dies from an ACS-related event every minute. Each year, approximately 1.4 million Americans are hospitalized with ACS, of whom 810,000 are hospitalized for myocardial infarction. Studies have shown that plaque rupture causes approximately 75 percent of fatal myocardial infarctions.
About the HeartFlow FFRct Analysis
Clinicians diagnostics someone with suspected CAD want to know as definitively as possible if the individual has a significant blockage in their coronary arteries. They also want to know the impact of that blockage on blood flow so they can best determine which treatment pathway is appropriate (e.g., medical management, stenting or coronary artery bypass grafting).
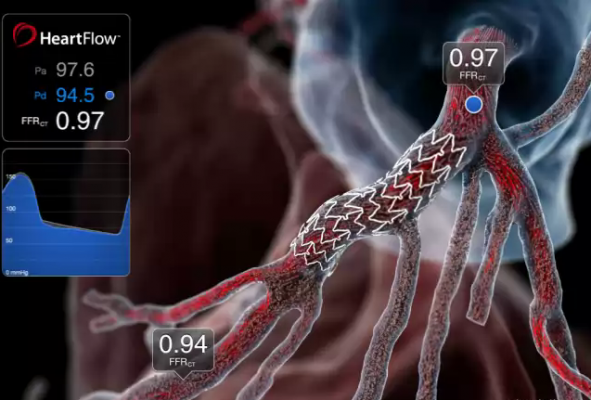
Data from a patient’s non-invasive CCTA are securely uploaded from the hospital’s system to the cloud. HeartFlow leverages deep learning to create a personalized, digital 3D model of the patient’s coronary arteries. The HeartFlow Analysis then uses powerful computer algorithms to solve millions of complex equations to simulate blood flow and assess the impact of blockages on coronary blood flow. The HeartFlow FFRct Analysis is provided via a secure online interface to offer actionable information to enable clinicians to determine the optimal course of treatment. To date, clinicians around the world have used the HeartFlow Analysis for more than 15,000 patients to aid in the diagnosis of heart disease.
This technology has been demonstrated to reduce unnecessary and invasive diagnostic coronary angiography procedures, which can be associated with bleeding, stroke, major blood vessel damage and other serious complications. It also significantly reduces healthcare costs for hospitals.
For more information: www.heartflow.com


 May 19, 2026
May 19, 2026 









