June 2, 2011 – The U.S. Food and Drug Administration (FDA) this week is warning medical professionals and U.S. medical device vendors to beware of possible safety concerns and radioactive contamination of medical devices and components coming from Japan.
Japan is a critical participant in the global medical device market, and this industry was impacted by the massive March 11, 2011, earthquake and tsunami. The FDA’s Center for Devices and Radiological Health (CDRH) and Center for Biologics Evaluation and Research (CBER) is raising concerns about possible effects these events may have on medical devices, electronic products and device components intended for the U.S. market At this time, neither CDRH nor CBER has been notified of any defective product or serious adverse events associated with the use of a device related to this disaster.
However, given the extent of the devastation, CDRH and CBER have concerns about manufacturing conditions as a result of the earthquake and tsunami that could impact the safety and effectiveness of medical devices exported from Japan, intended for import into the United States. Their concerns include, but are not limited to, the potential for:
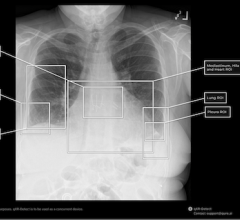
• Radioactive contamination of devices and/or device components, particularly those derived from animals, such as bovine serum albumin. Contamination in products can occur through uptake of radioisotopes from water or soil to animals through feed. Also, there is the potential for radioactively contaminated device implants to act as reservoirs for internal radiation exposure of patients,
• Contaminated water supply that could result in defective products that fail to meet device specifications,
• Loss of electrical power, a source of disruption in the manufacturing process, which directly impacts all components/ devices, specifically those that require refrigeration or temperature controls, such as tissue-based devices,
• Compromise in sterile products during or after production, including stored finished product,
• Compromise in the reliability of product performance (e.g., electrical connectors, microprocessors, alarms, sensors),
• Damaged and/or disrupted medical device manufacturing facilities in the affected and surrounding region may result in a shortage of components and/or finished devices.
CDRH and CBER are reminding manufacturers of finished devices that they must assure that their products comply with FDA regulations. In addition, the FDA requests that all manufacturers of components and unfinished devices do the same. Specifically, it is urging all device manufacturers and initial distributors of medical devices to take increased precautions to provide reasonable assurance of the safety and effectiveness of their devices as described in Title 21, Code of Federal Regulations (CFR), Part 820. Such actions might include increased sampling and enhanced testing of incoming raw materials and components, as well as of finished diagnostic and other medical devices prior to product release. Similarly, 21 CFR 1010.2(c) requires that electronic product certification be based on either a particular performance standard (21 CFR Part 1020) or on good manufacturing practices. Such practices would include the evaluation of raw materials and components as well as the finished product.
CDRH and CBER recommend that electronic product and medical device component manufacturers, finished electronic product and device manufacturers, and initial distributors of electronic product and devices, intended for U.S. market immediately take the following precautions:
• Assess incoming products and supplies to ensure that the product conforms to the vendor’s specifications and quality requirements.
• Closely monitor purchasing and acceptance activities including inspections, sampling, and testing. Carefully check all products for contamination or compromise, including device integrity such as cracks, breech in sterility, filth, defective equipment, or package integrity (dampness, water residue, mold, unpleasant odors, discoloration, or unreadable labels).
• Check all power cords and batteries and electric monitoring devices to make sure that they are not damaged by water.
Some products, components, and other materials used in the manufacture of a medical device require a temperature-controlled environment (e.g. refrigeration). For these items the FDA recommends the following precautions:
• If a vendor is not sure the product is safe, run quality control checks. This applies to all products including disinfectants and sterilants, dental products (e.g., bone filing materials), intra-ocular lenses that require refrigeration, blood grouping reagents, in-vitro diagnostics (e.g. HIV-1/enzyme immuno assay) and other such products.
• Heighten assessment of all animal-derived products (e.g., raw heparin) and other raw materials prior to finished device production.
• When possible, screen and assess the potential risk to safety associated with unfinished and finished products.
If a vendor has a pending purchase order for components, parts or finished electronic products or devices from the affected areas of Japan, the FDA suggest the following steps:
• Ensure that the manufacturer/supplier in Japan is operational.
• Ensure that pending device orders comply with the quality system regulation if you intend to market the device in the United States.
• If the product or device was manufactured or stored in a location that was flooded, check the product for signs of water damage or exposure to water.
• If the product or device was manufactured in a location that was flooded for a short period of time, the location’s water treatment system might have been contaminated. Determine if the municipal water supply was acceptable or that the affected firm used filtration, deionization, reverse osmosis, etc., to treat water during the manufacturing process. If the municipal water supply or the water treatment system was contaminated, it is practically impossible to manufacture acceptable product.
• If the manufacturer indicates that the water supply is acceptable, obtain documented evidence as verification.
• Determine if the manufacturer has an adequate restart procedure addressing one or more power outages during production.
• Determine the disposition of components or devices that were in production during the time of blackouts, especially devices undergoing sterilization.
• If a product or device was reworked, assure that the firm has adequate standard operating procedures for this process.
• If you label a device with a shelf life, determine if the declared shelf life will be compromised.
• If a device is intended to be sterile, validate the effects of re-sterilization on the finished product.
To determine the potential impact of the earthquake and tsunami on the supply of medical devices distributed in the United Stated, CDRH and CBER suggest the following:
• Evaluate the immediate and long term potential for shortages of parts, ingredients, components, and finished devices. Especially, unique products such as tubing, software, circuit boards, etc., that is currently manufactured by a sole supplier. If a shortage is anticipated, will it affect life-sustaining devices, as those used in dialysis or infusion pumps? If so, notify customers immediately.
• If the primary supplier is not operational, or is currently unable to meet your specifications for any reason, you may want to identify, qualify, and validate a secondary source of components or finished devices.
If a vendor determines there is a need for an alternate supplier for its parts, ingredients, components or finished devices, evaluate the need for a premarket approval application supplement, 21 CFR 814.39, or a new premarket notification [510(k)], 21 CFR 807.81.
To determine if the alternate supplier is required to register and list, please review 21 CFR, Part 807, Subpart B, Procedures for Device Establishments, to ensure that the supplier is in conformance with these requirements.
Additionally, the FDA warns vendors to be alert to false or misleading claims by suppliers and advertisements on the Internet, when attempting to locate an acceptable alternate part, accessory or component.
For more information: www.fda.gov/MedicalDevices/ResourcesforYou/Industry/default.htm


 June 02, 2026
June 02, 2026