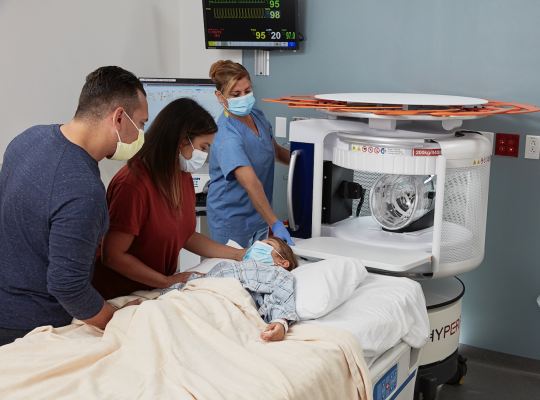
Photo courtesy of Business Wire
August 9, 2023 — Hyperfine, Inc., a groundbreaking medical device company that created the Swoop system, the world’s first FDA-cleared portable magnetic resonance brain imaging system, today announced completed enrollment for the multi-site observational study, HOPE PMR (Portable MRI for Children with Neurological Injury—A Pilot Study using Hydrocephalus as an Index Condition).
Children living with hydrocephalus typically undergo at least two brain scans per year to monitor pressure in their enlarged brain ventricles and identify potential shunt malfunctions. With the aim of exploring a safer, more accessible solution for hydrocephalus patients, the HOPE PMR study is assessing the feasibility of integrating the Swoop system, a brain imaging solution with zero ionizing radiation that is accessible at a child's bedside, into routine inpatient, outpatient, and emergency pediatric care settings. The study used pediatric hydrocephalus as an index condition to assess if Swoop system images can be used to accurately detect shunt malfunctions and assess ventricular size.
"The Swoop system represents a promising shift in brain imaging. We believe it has the potential to improve pediatric hydrocephalus management significantly," said Dr. Khan Siddiqui, chief medical officer and chief strategy officer at Hyperfine, Inc. "The insights gathered from this study will inform the viability of the Swoop system in pediatric healthcare settings and patient care.”
Dr. Jeffrey Leonard, chief of Pediatric Neurosurgery at Nationwide Children’s Hospital, added, "With the completion of the enrollment phase of the study, we are now embarking on the critical task of data analysis and academic publication preparation. Our collaboration with Hyperfine, Inc. paves the way for improvements in brain imaging, benefiting this vulnerable patient population."
About Hydrocephalus
Hydrocephalus, marked by an abnormal buildup of cerebrospinal fluid in the brain, affects more than one million Americans. It particularly poses substantial challenges in pediatric care. Current treatments, such as the surgical placement of a shunt, experience an alarming failure rate of around 50% within two years of placement1, highlighting a significant unmet need for improved solutions.
Although magnetic resonance imaging (MRI) is the preferred scanning modality due to its absence of ionizing radiation, practical constraints often limit its use. When MRI is unavailable, care providers must resort to computerized tomography (CT) scans, which carry notable risks. Published research indicates a single pediatric head CT scan could double the risk of radiation-associated malignancy2.
For more information: hyperfine.io
References:
1 https://www.hydroassoc.org/powerful-hydrocephalus-facts/
2 https://link.springer.com/content/pdf/10.1007/s00381-019-04345-3

 May 28, 2026
May 28, 2026 









