Greg Freiherr has reported on developments in radiology since 1983. He runs the consulting service, The Freiherr Group.
Must Radiologists Be Prepared To Delegate ... To Smart Machines?

Last year, our health system ranked dead last among those of 11 developed nations (including France, Germany, Great Britain and Canada) in calculations done by the Commonwealth Fund, a private foundation that specializes in the analysis of healthcare. This despite seven years of expanded access to healthcare through the Affordable Care Act, also known as “Obamacare.”
No big surprise there. Obamacare — like the debate to repeal and replace it — has been more about insurance than care. To see why simply increasing the number of insured patients won’t make healthcare much better, we have to take a deep dive into the stats.
The U.S. ranks last in healthcare outcomes, according to the Fund. It has the highest rate of mortality “amenable to healthcare,” the Fund stated in a report entitled “Mirror, Mirror 2017: International Comparison Reflects Flaws and Opportunities for Better U.S. Health Care.” And the U.S. has achieved “the smallest reduction in that measure during the past decade,” according to the Fund.
So, clearly, we are not getting the job done. And it isn’t because we’re not spending enough. In 2014, the U.S. spent more than 16 percent of gross domestic product on healthcare, according to the Fund. This compares with between 8 and 12 percent for the 10 other nations in the report. And the gap separating the U.S. from other nations has progressively increased over the years and shows signs of continued widening.
Imaging As Catalyst
Rather than debating how to make insurance affordable, we should be looking for ways to make care more effective. A big step in that direction would be the elimination, or at least reduction, of waste. Increased efficiency and making better use of available resources tends to improve performance. Enterprise imaging can do both.
Integrating information sources has the potential to provide diagnosticians and caregivers comprehensive information about patients’ conditions, just as this integration might improve teamwork by those caregivers. Pundits have long promoted such integration.
“We need to move to integrated practice units that encompass all the skills and services,” wrote Harvard business professor Michael E. Porter in the July 9, 2009, issue of the New England Journal of Medicine, a point that Porter reiterated four years later in the Harvard Business Review. Doing so is part of a fundamentally different healthcare strategy to maximize value by delivering the best outcomes at the lowest cost, one that is organized around the needs of patients.
But enterprise imaging will not be enough. It must be part of a culture of change designed and built for efficiency and effectiveness, one that emphasizes meeting the needs of the patient. The technology underpinning this new culture is already bubbling to the surface.
Artificial intelligence (AI) has the potential to help physicians make decisions better and faster. It is already becoming a part of everyday life from smartphones to smart homes.
But before AI can play a serious role in the practice of medicine — and this is the hard part to stomach — some physicians, notably radiologists, may have to be “displaced.”
Displacing — Not Replacing
In a JAMA “Viewpoint” published Dec. 13, 2016, an associate professor of radiology at the Hospital of the University of Pennsylvania (HUP) and the chair of innovative medicine at the Scripps Research Institute speculated that some routine tasks performed by radiologists could be automated.
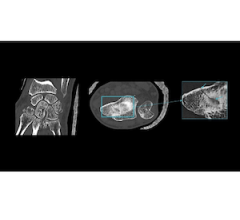
Scripps’ Eric Topol, M.D., and HUP’s Saurabh Jha, MBBS MRCS, MS, urged radiologists to identify “cognitively simple tasks” that smart machines could take over. They cited two such tasks — computed tomography (CT) screening for lung cancer and portable chest radiograms taken in the ICU to confirm the proper positioning of support lines. Delegating simple tasks to machines would allow radiologists to spend more time on challenging cases, where their expertise is most needed. This streamlining of medical practice, if widely applied, holds out the promise for improved efficiency and speedier patient care.
And the use of AI need not be restricted to high-tech imaging. Cameras built into smartphones are already being used to capture everyday events in peoples’ lives.
Might pictures sent via patient portals built into enterprise imaging help in the diagnosis of a skin lesion? Might smart machines review submitted images and select ones that warrant immediate review by physicians, thereby reducing the load placed on diagnosticians and optimizing efficiency?
Similarly, might smartphones be morphed into medical sensors — not only capturing and transmitting vital signs but ultrasound images and video? If so, AI could be leveraged to review these images, spotting cases that deserve careful study by physicians.
There are a lot of “mights” in this. And radiologists will have to go along with it. But the radiology community may soon have little choice. Healthcare costs are mounting. AI might (there’s that word again) make a difference.
It’s important to note, however, that no matter how “artificially smart” medicine becomes, healthcare costs probably will rise. Making medicine more efficient could slow expenditures, but it will probably not decrease them.
The demographics of our population will see to that. Americans are getting older. And older people need more care.
Simply put, enterprise imaging — with or without AI — is not the magic bullet for better or lower cost healthcare any more than fuel-efficient — or electric — cars are the solution to air pollution in a nation with ever more cars. But it can improve efficiency. And healthcare efficiency must be increased.
We can strive to get the most for the money we spend and to deliver the best healthcare in the world.
And those are metrics that really could matter.
Related Content on Artificial Intelligence in Radiology
Artificial Intelligence Could Learn From the Medical Imaging Goldmine of the NHS Archives
VIDEO: Machine Learning and the Future of Radiology
How Artificial Intelligence Will Change Medical Imaging


 May 04, 2026
May 04, 2026