October 31, 2023 — Prostate cancer has a significant impact globally. For example, approximately one in eight men in the ...
RSNA
This channel contains news about the Radiological Society of North America (RSNA), including coverage of its annual meeting. RSNA is a leading resource for the radiology and all its subspecialties. This includes all areas of medical imaging, angiography, computed tomography (CT), digital X-ray, magnetic resonance imaging (MRI), nuclear imaging, ultrasound, PACS and advanced visualization. For coverage of RSNA specific to cardiovascular medicine and interventional radiology, visit our sister publication Diagnostic and Interventional Cardiology (DAIC) and its RSNA channel.
October 30, 2023 — Fujifilm Healthcare Americas Corporation, a leading provider of diagnostic and enterprise imaging ...
October 26, 2023 — The Radiological Society of North American (RSNA) made a major announcement this morning regarding ...
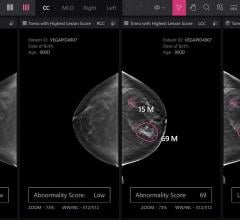
Despite decades of progress in breast imaging, one challenge continues to test even the most skilled radiologists ...
October 24, 2023 — Reseller partners, IMAGE Information Systems (iQ IMAGE), headquartered in Rostock, Germany, and aycan ...
October 18, 2023 — DeepTek.ai, a leading medical imaging AI company in India has announced that it has received ...
October 16, 2023 — The Radiological Society of North America (RSNA) has announced highlights of the Technical Exhibits ...
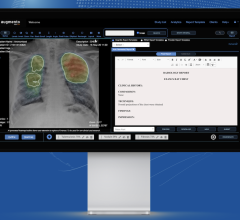
Clinicians and referring physicians need fast, secure access to both patient data and their diagnostic or viewing tool ...
October 13, 2023 — Hospital TV leader LG Business Solutions and healthcare technology innovator Aceso Interactive are ...
October 13, 2023 — Locally run large language models (LLMs) may be a feasible option for extracting data from text-based ...
Registration is now open for The Radiological Society of North America’s (RSNA) 2023 Conference: Leading Through Change ...
Agfa Radiology Solutions is committed to enhancing clinical outcomes and operational efficiency, underscoring its ...
October 4, 2023 — A new artificial intelligence (AI) model combines imaging information with clinical patient data to ...
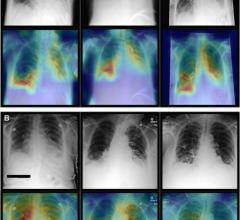
October 4, 2023 — An AI chest X-ray foundation model for disease detection demonstrated racial and sex-related bias ...
September 28, 2023 — Siemens Healthineers has announced the Food and Drug Administration (FDA) clearance of the Magnetom ...
Agfa Radiology Solutions delivers diagnostic imaging solutions that set the standard in productivity, safety, clinical ...
September 26, 2023 — In a study of more than 2,000 chest X-rays, radiologists outperformed AI in accurately identifying ...
September 21, 2023 — Declines in cardiovascular procedure volumes observed early in the COVID-19 pandemic greatly ...
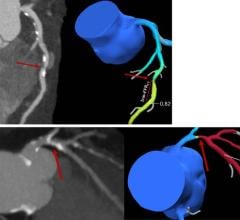
September 19, 2023 — An advanced CT test can identify individuals with stable angina at a reduced risk of three-year ...
September 14, 2023 — Royal Philips, a global leader in health technology, today announced the launch of Philips Image ...
September 12, 2023 — The Radiological Society of North America (RSNA) launched “RSNA Market Insights,” a series of ...
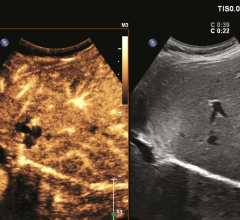
September 8, 2023 — When diagnosing and treating cancer patients, the dynamics of blood flow to and from a suspected ...
September 5, 2023 — Using a standardized assessment, researchers in the UK compared the performance of a commercially ...
August 31, 2023 — A new article published in RadioGraphics, a journal of the Radiological Society of North America (RSNA ...


 October 31, 2023
October 31, 2023