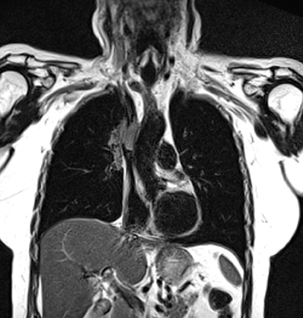
At least a few Europeans think ventilation MRI should be commonplace.
MR sequences are faster than ever before, they say; basic protocols as easy to perform as those for the knee or spine. Combined with contrast, lung MR can produce results as accurate as those seen in the liver, according to said Prof. Hans-Ulrich Kauczor, M.D., medical director and
chairman of radiology at the University Hospital of Heidelberg, Germany.
Kauczor evangelized the benefits of lung MRI in a special focus session at the European Congress of Radiology in early March. Speaking for himself and other advocates, he said “our job is to show on a case-by-case basis — depending on the primary tumor and quality of the lung protocol — that whole-torso staging analysis of the lung by MRI is at least as good as CT or even PET/CT.”
Kauczor and his colleague, Prof. Edwin van Beek, M.D., chair of clinical radiology at the University of Edinburgh, UK, put together a strong argument, at least for some applications. Lung MR can be used to downstage cancer, clearing the way for surgery on patients previously thought to be inoperable, Kauczor said. It is the only way to visualize the superior sulcus tumors and surrounding vascular and brachial plexus structures. Chest wall invasion can be better studied using MRI, according to fellow evangelist van Beek, who expects positron emission tomography/computed tomography (PET/CT) and CT to remain the primaries for lung imaging, but asserts that MR should be used more often.
All this came as something of a surprise to me, who for the past 30 years had heard much more about MRI of the head, spine, abdomen, peripherals — in fact, every part of the body — other than the lungs. Ventilation MR simply wasn’t on the radar — except during one anomalous time.
Back 15 years ago, I remember that a dedicated group of believers were promoting lung MR with hyperpolarized gases. The idea took root at a small company called Magnetic Imaging Technologies Inc., MITI for short. It then shriveled on the vine when MITI was acquired by Nycomed Amersham, which was then acquired by GE Healthcare. The proselytizing over lung MR using protons then made me wonder, what became of hyperpolarized helium and xenon? Not much, I found out. But that could change.
A little digging on my part found that hyperpolarized MR re-emerged last year with the launch of Polarean, which had secured the assets and intellectual property for the modality from GE Healthcare. Its own evangelical, John P. Mugler, III, Ph.D., professor of radiology and medical imaging, and biomedical engineering, at the University of Virginia, had been stumping for the broader use of this technology since making the first hyperpolarized xenon images of the human lung in 1996.
Mugler was at it again at SPIE Biomedical Optics and Medical Imaging last year, where during the keynote presentation (http://spie.org/x86304.xml) he described the disadvantages of conventional lung MR — low proton density and the millions of air-tissue interfaces that disturb magnetic fields — then extolled the virtues of hyperpolarized MR. Mugler illustrated those virtues with hyperpolarized MR images of cystic fibrosis, chronic obstructive pulmonary disease, bronchopulmonary dysplasia, and the signs of damage from smoking and those of lung transplant rejection. With the formation of Polarean with its singular focus being on building and selling the technology for hyperpolarized MR, the way is clear for the broad use of noble gasses to assess lung health, he said.
It turns out there are a whole lot of possibilities. At the recent European Congress of Radiology (ECR), Kauczor and van Beek pointed to quantitative biomarkers that might help MR assess blood flow in the lung and motion of the diaphragm. In some quarters, noncontrast proton-based MR angiography is already challenging echocardiography for diagnosing pulmonary embolism in pregnancy, they said. In the future, lung perfusion without contrast could add information about pulmonary artery obstruction and hypoxic vasoconstriction, as well as confirm pulmonary hypertension, embolism and chronic obstructive pulmonary disease.
With a two-pronged effort — one using conventional proton sequences, the other hyperpolarized gas protocols — the lungs may become just another area for MRI. The proponents are out there.
Greg Freiherr has reported on developments in radiology since 1983. He runs the consulting service, The Freiherr Group. Read more of this views on his blog at www.itnonline.com.


 April 28, 2026
April 28, 2026