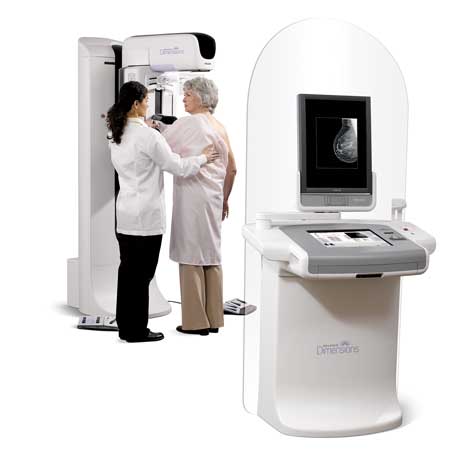
Tomosynthesis is a 3D imaging technology that involves acquiring as many as 15 different images of a stationary and mildly compressed breast at multiple angles during a short scan.
In the ongoing battle to improve breast cancer detection and diagnosis, full-field digital mammography has held steady as the first line of defense. But recent developments have given rise to technologies that are revolutionizing breast imaging, and have the potential to one day replace mammography as the gold standard.
ABUS Advances on FFDM
The 2005 ACRIN Digital Mammographic Imaging Screening Trial established full-field digital mammography’s (FFDM) superiority over film mammography in detecting significantly more cancers in women with dense breasts (who are at a higher risk for developing breast cancer) and women 50 and younger. This study has since driven the growing adoption of FFDM.
When a mammogram is inconclusive, ultrasound is often the follow-up test. In a newly launched clinical study, researchers are comparing mammography alone to 3D Automated Breast Ultrasound (ABUS) combined with routine screening mammography. The somo·InSIGHT multi-center clinical study is led by Marc F. Inciardi, M.D., radiologist at the University of Kansas Breast Imaging Center. Dr. Inciardi will use the somo-v Automated Breast Ultrasound technology, which is currently FDA approved for use as an adjunct to mammography, to examine whether digital mammography along with ABUS is more sensitive to detecting breast lesions compared to mammography alone in women with dense breasts. U-Systems, the study’s sponsor and manufacturer of somo-v, hopes to show that ultrasound is capable of finding cancer not visible with mammography in women who have dense breasts.
According to the Kansas Cancer Center, one of 12 national sites participating in the study, ABUS is a breast imaging technology that is less affected by a woman’s breast density. Unlike mammography, which uses radiation, ABUS uses sound waves at a safe frequency to create images of the internal breast tissue. This technology has been shown to find cancer not visible in women who have dense breasts.
While mammography remains to be the gold standard, “[a]utomated whole breast ultrasound may facilitate implementation and profitability of screening ultrasound.”1 U-Systems states on its Web site, “It is anticipated that the somo-InSIGHT study will prove that the somo-v is an essential tool and will make a positive difference in women’s health-care.”2
Although ultrasound for breast is fast gaining credibility in the medical community, it is not without its own shortcomings. Although it provides excellent contrast, it does lack the spatial resolution provided by mammography. Another drawback is the requirement for a qualified sonologist to handle the transducer to obtain the quality images. Evolving 3D and even 4D technology that lessen the need for a sonologist, coupled with increased demand for low to no radiation diagnostic tools, are setting the stage for a day when breast ultrasound could hold its own as the diagnostic tool of choice for breast cancer imaging.
Tomosynthesis: The Next Frontier
The promise of 3D mammography has been discussed in academic circles and detailed in medical imaging conferences and peer-review journals for almost a decade, but only recently has the technology caught up with the theory. The modality also known as tomosynthesis is now awaiting pre-market approval in the United States — it’s already being used in Europe with great reviews — and is currently being evaluated in a handful of U.S. trials.
Joseph Lo, M.D., associate professor of radiology, biomedical engineering and medical physics at Duke University, is leading a trial investigating breast tomosynthesis in partnership with Siemens Healthcare. However, new modalities, while promising, are still mostly viewed as adjuncts to mammography.
“[Mammography] has been the Holy Grail all along even though we know it is not perfect. So how do we improve upon that? Finally, the pay off is breast tomosynthesis,” he said. “Tomosynthesis is really the most exciting thing to come along in decades when it comes to breast cancer imaging. Really, nothing else out there has the potential to replace mammography in all its roles except for tomosynthesis. I’m talking about for screening, for diagnosing, for biopsies. It’s amazing how this one technique can cover the full spectrum of breast cancer imaging needs.”
Down the road, researchers are also exploring tomosynthesis’ more far-reaching potential, such as its ability to characterize the extent of cancer and monitor response to treatment, added Lo.
In simple terms, tomosynthesis is a 3D imaging technology that involves acquiring as many as 15 different images of a stationary and mildly compressed breast at multiple angles during a short scan. The images are captured by moving an X-ray tube in an arc over the breast, and mathematically synthesizing the tomogram into a volumetric view to show tissue as layers. A tomosynthesis exam typically takes only a few seconds longer than a conventional mammogram and dramatically increases accuracy by eliminating the problems of tissue overlap — and with less radiation exposure than more advanced modalities such as CT scans.
Tomosynthesis claims to be exactly the missing prescription for diagnosing cancer in the sizable fraction of women with dense breast tissue. “Cancer is very often hidden away underneath dense tissue — that’s one of mammograms biggest disadvantages. With a 3D scan, it really doesn’t matter, because even if it’s hiding behind dense tissue, you can still see it from a different angle,” Lo said.
He draws an analogy between tomosynthesis and searching for an ace of spades in the middle of a deck of cards: “If you hold the deck up to the light, you’re not going to see a darn thing. If you ruffle through and pull out the one card you need, there you go — that’s the card you want,” he said. “Same thing when dialing through these slices. If there’s something like a cancer, it jumps out at you. It literally just pops.”
“If and when approved, tomosynthesis will hold the honor as the only modality to meet a short but crucial checklist: Ability to image entire breast and detect both masses and micro-calcifications; relatively inexpensive; short exam time; and doesn’t require a radiologist to the conduct exam,” explained Andy Smith, M.D., Ph.D., senior director of Holigic Inc.’s Image Science Group, the first and only imaging vendor thus far to submit the technology for pre-market approval. “3D X-ray imaging meets all those requirements. It addresses the fundamental limitations of regular mammography.”
As a two-dimensional modality, conventional mammography is simply missing too many hidden cancers. “You can think of imaging as trying to find a certain tree in a forest of trees and the cancer can be thought of as being one of those trees inside the forest. When looking at a photo of a forest, it’s very difficult to see an individual tree,” Smith said. “3D is a way of walking into a forest and being able to look very clearly at the trees.”
The transition from conventional mammograms to 3D mammograms should be a pretty smooth one for radiologist, said Lo. “They don’t need to be trained from scratch. In their eyes, it already instinctively makes sense,” he says. “When they see cancer on a tomosynthesis study, it just looks bigger, more obvious, easier to see compared to a regular mammogram, or you just see it where you don’t see it before.”
As tomosynthesis awaits the rigorous pre-market approval, which experts agree is forthcoming although they’re not sure exactly when, the medical community is waiting for its promise to be delivered. “In general, the medical community has been overwhelmingly positive about this. We usually have to sell new techniques to doctors. In this case, it’s the other way around,” Lo said. “Even back 5 or 10 years ago, when we were just beginning to work out the initial details of this technology, doctors were already knocking on our doors saying, ‘Hey, I want that and I want it now.’”
In the future, vendors will probably offer retrofitted mammograms systems that have the option to upgrade to 3D, not necessarily entirely new systems, for an incremental price hike. “Sometime in the relatively new future, our vision is that this will be the new way of doing both screening and diagnosing,” Lo said. “I think that this is really going to change how radiologist work and how patients perceive breast cancer screening. I think we will be catching breast cancer earlier and be able to treat them much earlier.”
Breast MRI: Top of the Sensitivity Food Chain
One of the primary imaging tools used for high-risk patients with dense breasts – not for general screening – is magnetic resonance imaging (MRI). “We want to detect [cancer] before it presents clinically,” Smith said.
Unlike X-ray based modalities, MRI for the breast offers a completely new path to diagnosing breast cancer. Instead of using ionizing radiation, breast MRI uses a powerful magnetic field, radio frequency pulses and a computer to produce detailed pictures of organs, soft tissue, bone and virtually all other internal body structures. It is traditionally seen as a supplemental tool for detecting and staging breast cancer and other breast abnormalities. In recent years, it has gained a reputation for cutting-edge sensitivity across all patient groups.
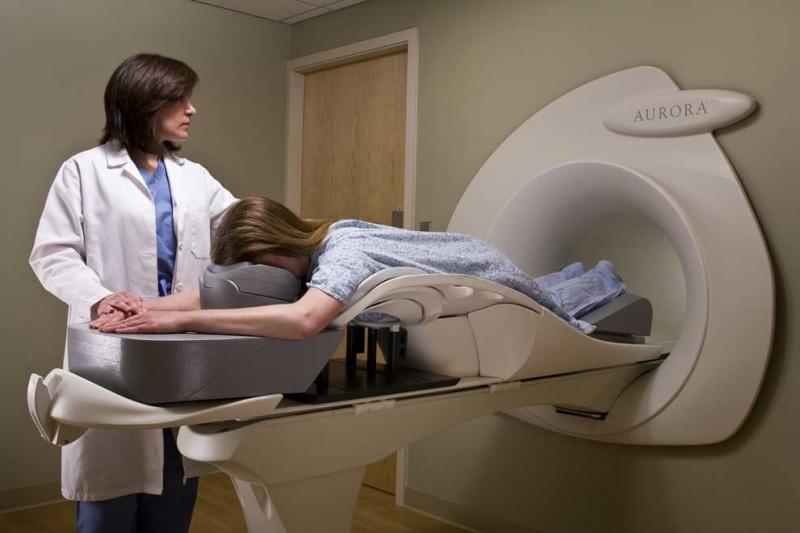
Compared to ultrasound and MBI, “breast MRI is at the top of the food chain,” said Steven E. Harms, M.D., FACR, radiologist at The Breast Center of Northwest Arkansas, which uses a dedicated breast MRI system from Aurora. “The sensitivity of breast MRI is high regardless of which group you segment out: women with dense breasts, young women, old women, any way you want to cut the pie.”
Harms said he is one of the early developers of MRI for breast imaging, and has been using this technique since 1990. The early days of MRI completely changed the game, he recalls.
“When we first came out, we were seeing cancers that we couldn’t see any other way,” he said. “The advantage of MRI is that its so highly flexible and there are so many different things that you can do. It’s like turning people loose to their own creativity, whereas a lot of other imaging methods are locked in to whatever manufacturers decide to do. With MRI there are many different ways of doing things, and there will be even more in the future.”
The major drawback of breast MRI is the hefty price tag it carries, admits Harms. “The biggest problem with MRI is its cost. If an MRI was the same cost as a mammogram, I don’t think we would be having this discussion.”
There’s a potential to make MRI more affordable down the road, especially if it is to remain competitive with emerging technologies, Harms adds. Regardless of the cost factor, he doesn’t see it being eclipsed by any other diagnosing tool – even the much buzzed about Molecular Breast Imaging (MBI) technique. “The reason is that it’s so incredibly good. Something of that nature just comes along once every 50 years,” Harms said. “We’ve got resonating hydrogen nuclei telling a story about their environment that you can’t get from X-rays or ultrasounds. It’s not something easily replaced.”
Molecular-based Breast Imaging: New Contender
If MRI is at the top of the food chain when it comes to diagnosing breast cancer, the re-emergence of molecular-based imaging (MBI), also known as breast specific gamma imaging (BSGI), is providing some healthy competition.
With MBI, the patient receives technetium 99 sestamibi, which cancerous cells absorb more of and appear as “hot spots.” MBI overcomes many of the limitations of MRI, such as the inability to image patients with pacemakers, claustrophobic or obese patients, and problems with insurance/expense restrictions. Perhaps most importantly for the patient, MBI eliminates the trauma over false positive readings more common with MRI, therefore preventing unnecessary biopsies.
“MBI is an excellent and effective alternative for patients who don’t meet the criteria for MRI,” said Leora Lanzkowsky, MD, director of Women’s Imaging at Nevada Imaging Center. This includes patients who cannot tolerate breast MRI because they can’t stay in the machine or can’t tolerate the contrast injection, or simply can’t afford it. Patients with very dense breasts, as well as women over the age of 69 who are at an increased risk of developing breast cancer and often can’t tolerate MRI screenings for a variety of reasons, including patients with a cardiovascular implant device, are particularly great candidates for MBI. “As you get older, everything that is relatively harmless can cause harm,” Lanzkowsky said.
And in patients of any age who have multiple complex findings on their other imaging studies and radiologists need to rule in or rule out an area to biopsy, MBI is also an excellent alternative. “There is every indication for BSGI and no contra-indications (i.e. pregnancy, allergy to pharmaceutical). It’s an extremely well tolerated test, it’s less expensive, easier for the radiologist to read. It’s got tremendous advantages, she said.”
The proof is in the pudding, asserts Lanzkowsky, who herself has undergone two MBI procedures. “I’m no cowboy,” she said. “I won’t go and use a new technology without considering all the existing technology and studies that have been done. I have to see scientific evidence.”
Still, Lanzkowsky sees the most promise in a technology that marries methodology and function.
“That might be our great solution. A conjoined technology that can tell you, a scar area might on tomosynthesis like cancer, but it reacts like a scar,” she said. After all, each patient is different and might demand a different approach – or a combination of studies — to best diagnose breast cancer. “You can’t really lump women into groups. It’s becoming much more individualized now, as is the therapy.”
References:
1. JAMA 2008;299(18):2151-63
2. U-Systems, Inc. SOMO-INSIGHT Clinical Study. http://www.u-systems.com/Healthcare_Professionals/index.cfm/15.


 May 27, 2026
May 27, 2026 









