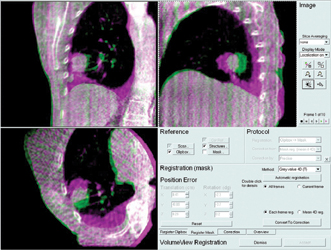
One of the most important recent advances in radiation oncology has been the integration of 4-D treatment planning tools into the clinic. 4-D treatment tools have enabled the radiation oncologist to better plan and account for the tumor motion in a specific patient.
During a 4-D computed tomography (CT) scan, the CT scanner continuously acquires projection data at each couch position for an interval equal to the patient’s respiratory period plus the interval needed for one CT tube rotation. The beam is turned off and the table is advanced. This process is repeated until full longitudinal coverage of the region of interest has been obtained. Typically, a total of 1,000-1,500 images are acquired during a 4-D CT study.
These images are then collected and analyzed so the treating physician can understand what the tumor looks like as it moves, and also better understand the magnitude of motion for a specific tumor. The treating physician can then define a target volume that includes the shape of the tumor and the volume that accounts for motion.
Some physicians treat the volume of space where the tumor spends any amount of time. Others treat a volume that represents where the tumor spends a portion of its time (i.e., 75 percent of its time is spent in this space). Data from ongoing research on the optimum volume that should be treated should be considered.
For decades prior to the development of 4-D treatment planning tools, the incorporation of motion into treatment planning was based on anecdotal information, small series of studies using older technology to understand motion, and always the application of generic or population-based averages to a specific patient. With the advent of 4-D treatment planning tools, the motion for a patient can be specifically accounted for.
In some instances, the motion is greater than anticipated. In this situation, it is possible the conventional approach of arbitrarily assigning a margin to account for motion may have undertreated these tumors, because their motion was significantly greater than anticipated. In other instances, the motion is far less than anticipated. In this situation, the arbitrary expansions used to encompass the expected motion result in significantly more normal tissue exposure than is necessary.
Over the years, radiation oncologists have attempted to find surrogates for 4-D information. Some have tried obtaining inspiration and expiration treatment planning studies and others have used a conventional positron emission tomography (PET)/CT target volume. 4-D CT scans, however, provide more accurate spatial and geometric information than these techniques.
In addition to the obvious advantages of more accurately incorporating motion into the target volume, 4-D CT imaging has some other benefits. These include overcoming the issues of blurred images associated with slow CT scans. The loss of resolution that occurs with these slow CT scans can lead to errors in the target delineation or normal tissue delineation.
There are several advances in 4-D treatment planning and radiation treatment delivery that also have been recently introduced into the clinic. Linear accelerators are now being equipped with 4-D conebeam CT capabilities. This will allow the treating physician to even more accurately prove the tumor is encompassed within the treatment field at the particular instant the patient is treated. (See sidebar for more information.)
Vivek Mehta, M.D., is a radiation oncologist at the Swedish Cancer Institute in Seattle, Wash. He is also the director for the Center for Advanced Targeted Radiotherapies at the Swedish Cancer Institute.
SIDEBAR: 4-D Cone Beam CT
The Netherlands Cancer Institute - Antoni van Leeuwenhoek Hospital (NKI-AvL) in Amsterdam, a clinical partner of Elekta, has been doing studies on 4-D computed tomography (CT) for a number of years. Jan-Jakob Sonke, Ph.D., at NKI-AvL has been part of several presentations on 4-D CT and cone beam CT (CBCT) at meetings of the American Association of Physicists in Medicine (AAPM). In an abstract of a program presented at the 2004 annual meeting, Sonke gives the following overview:
“Advances in image acquisition and reconstruction now permit generation of temporally varying (4-D) models of periodic movement (e.g. breathing) in patients from a single session of scanning. In currently emerging commercial applications the methods of data acquisition are generally through the use of fast slip ring CT scanners with single- or multi-slice detectors or through linear accelerator gantry-mounted CBCT scanners.
“In conventional CT scanners, data are generally oversampled by either acquiring axial cine data over times beyond the expected periodicity of movement (e.g. 4-6 seconds for breathing) at each index of couch position or via helical acquistion with a very tight pitch. For CBCT, the gantry is generally slowed down to increase the number of projections per rotated gantry angle (limited by the data acquisition rate of the imaging system) compared to what is needed for 3-D static CBCT. To generate patient models at various phases of movement, a signal (either external or internal) of movement is used as an index.
“Example external signals for breathing include air volume measured via spirometry, and movement of the chest or abdominal wall assessed from axial CT data or external sensing of reflecting markers. Internal signals have been used especially in the reconstruction of respiratory-correlated cone beam CT (RCCBCT), in these cases based on features present in the projections (e.g. diaphragm position, tracked anatomic region position). Image processing algorithms make the selection of internal signal automatic. Data from conventional CT may be sorted in either image or projection space. RCCBCT involves sorting in projection space exclusively. With current 4-D models, artifacts related to undersampling as well as irregular movement are still present to some extent. Further model-based approaches, such as temporal regularization and iterative optimization, are currently under investigation to improve the quality of 4-D CT.”
In a 2006 AAPM presentation describing NKI-AvL’s continued experiences with cone beam-guided radiotherapy, Sonke’s conclusions were:
• Cone beam CT provides soft tissue contrast, is efficient and does not require moving or touching the patient;
• 4-D CBCT provides a wealth of information (and a huge amount of data);
• Dose needed for CBCT scan is considerably smaller than for standard EPID (electronic portal imaging device) localization fields;
• Imaging quality [is] sufficient for image guidance;
• Several soft-tissue and bony anatomy-based protocols [are] in routine clinical use;
• Substantial investment and support of vendors [is] required to enable advanced image-guided protocols;
• Image guidance is potentially dangerous. Do not underestimate the residual uncertainties.
Sonke and colleagues developed the technology behind Elekta’s Symmetry, which was introduced in 2010. For image-guided radiation therapy (IGRT), Symmetry captures image data during the breathing phase and performs sophisticated computations to provide 4-D data that helps visualize tumor position.
— Helen Kuhl


 May 19, 2026
May 19, 2026 









