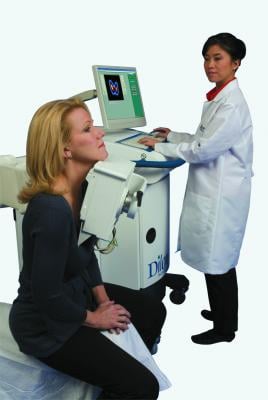
May 15, 2013 — ECRI Institute released a report listing three key questions and the answers concerning breast-specific gamma imaging (BSGI; sometimes referred to as molecular breast imaging or MBI). The technology uses a specially designed gamma camera system to image the uptake of a tracer that emits gamma radiation (most commonly 99mtechnetium-sestamibi [MIBI]). MIBI is preferentially taken up by cancer tissue, and thus BSGI can be used to image breast cancer for a variety of clinical indications. Unlike X-ray mammography, BSGI is not affected by the density of breast tissue, and therefore it may be particularly useful for screening and diagnosis of breast cancer in women with dense breast tissue.
Indications for BSGI may include patients with dense breast tissue, difficult-to-interpret mammograms, implants, palpable lesions not detected by mammography, multiple suspicious or indeterminate lesions, pre-biopsy evaluation of suspect areas, disease staging for breast conservation surgery, and evaluation of post-surgical or post-therapeutic breasts. Contraindications are pregnancy and hypersensitivity to the tracer.
Regulatory Status
All three of the BSGI devices manufactured by Dilon Technologies (Newport News, Va.), Gamma Medica (Northridge, Calif.) and GE Healthcare (Wauwatosa, Wis.) have been cleared by the U.S. Food and Drug Administration (FDA) for marketing under the 510(k) process for diagnostic imaging of the breast as an adjunct to mammography.
State of the Evidence Base
ECRI searched 17 external and internal databases, including PubMed and Embase, through Nov. 7, 2012, for clinical trials on the use of BSGI for breast cancer.
Key Question 1: For what indications and patient populations has BSGI been clinically studied?
ECRI identified published studies of BSGI for screening asymptomatic women, for diagnostic workup, for pretreatment evaluation and for monitoring response to neoadjuvant therapy. They did not identify any published studies of BSGI for monitoring response to post-surgical treatment or for detecting recurrences of cancer.
Key Question 2: What is the accuracy of low-dose BSGI for screening the general population? For screening women with dense breast tissue?
Searches did not identify any studies of low-dose BSGI for screening that met our study inclusion criteria.
Key Question 3: What is the accuracy and utility of BSGI for pre-treatment workup? In comparison to other imaging technologies (such as MRI) for this indication?
Four studies of a total of 445 patients met inclusion criteria for analysis for this question. The crude mean diagnostic yields of occult lesions could be computed from the reported data. They rated the evidence as moderate in quality, but no robust analysis could be performed, and therefore they rated the evidence as insufficient to answer this question. Only one study reported on a direct comparison to MRI. Two studies reported information on the impact of BSGI on medical decision making; the most common impact was triggering additional imaging and biopsies, followed by changes to additional treatment plans or leading to more extensive surgical treatment.
ECRI Institute Conclusions
For diagnostic workup, the sensitivity of BSGI for distinguishing between malignant and benign lesions is approximately 92 percent. BSGI may be a valid option for a diagnostic workup in some women, particularly for women with dense breast tissue. However, the evidence available as of November 2012 was insufficient to evaluate the accuracy and utility of BSGI for any other breast screening, diagnostic, or monitoring applications.
For more information: www.ecri.org

 June 02, 2026
June 02, 2026 









