September 20, 2011 – A national survey found that women overwhelmingly want the option for additional screening tests to find cancer early, even when testing resulted in a false positive – a suspicious area found by biopsy to be non-cancerous. Nine out of 10 women who required a biopsy to determine a false positive indicated that they would still opt for the additional screening the following year.
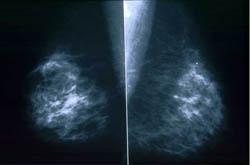
While 55 percent of women surveyed experience anxiety while waiting for the results of their yearly mammogram, 80 percent of those women do not let anxiety deter them from their next scheduled mammogram. Results demonstrate that women have regular screening mammograms for the benefit of the early detection of cancer and would choose additional screening measures to give them the best chance of early detection. This is particularly notable for women for whom a mammogram is compromised due to dense breast tissue; as density increases, the sensitivity of mammography decreases, missing cancer at least 40 percent of the time.
In fact, 93 percent of women, if informed of their dense breast tissue, would elect for an additional screening test. Clinical studies have shown that women with dense breasts may benefit from adjuvant screening modalities such as molecular breast imaging (MBI), magnetic resonance imaging (MRI) and ultrasound, which are more sensitive than mammography and thus may yield more false positives. It has long been maintained that “anxiety” over a false positive is a stressful and possibly emotionally debilitating experience for women. This concern is one of the most frequently cited objections to legislative efforts seeking to standardize the communication of breast density to women.
“This survey clearly shows that women want all the relevant information about their own breast health,” said Wendie Berg, M.D., radiologist and principal investigator and chair of the ACRIN 6666 Study. “In women with dense breasts, mammography is more likely not to show the cancer if present and women with dense breasts are also at increased risk of developing breast cancer. Women should have the information needed to advocate for themselves in this process.”
The national survey of 1,000 women aged 40 to 64 was conducted online in August 2011 by Research Now. Commissioned by Are You Dense Inc., the results indicate a clear preference by women for a false positive over a potentially life threatening missed positive.
“While medical authorities must weigh scientific evidence and recommend to the lay public whether, how often and with what tests women should be screened for breast cancer, there are times when these authorities must take into account women's preferences. These include patient anxiety and the issue of false positive examinations. The issue of false positives is not only patient anxiety but also the cost to society of these examinations,” said Thomas Kolb, M.D., a radiological expert and author of the first published contemporary study detailing the use of screening breast ultrasound to detect cancers. “When evaluating costs one must ask whether a recommendation not to screen is influenced by insurance companies’ profits or government healthcare costs. If so, women may be angered to find that economics, in the guise of science, had any influence in healthcare recommendations. There is a time and place where women should take part in decisions affecting their health and this is one of them.”
“Since my advanced stage cancer diagnosis in 2004, after dutifully having my yearly mammogram, I’ve met women with the same tragic story – a missed positive – that resulted in advanced cancer, aggressive treatment and the likelihood of dying prematurely from breast cancer. These women would exchange their missed positive any day for a false positive,” said Nancy Cappello, M.D., founder of Are You Dense Inc., who was instrumental in the first law in the nation to standardize the communication of breast density in women through the mammography report.
According to JoAnn Pushkin, director of government relations for Are You Dense Advocacy Inc., the communication of breast density to women, through their mammography report, is critical in finding cancers early. “If I had been told that, due to density, the ability of my mammogram to find cancer was little better than a coin toss, of course I would have begun a discussion with my doctor about the possibility of additional screening. Without density notification, the 40 percent of women with dense breasts are effectively being denied equal access to early detection.”
For more information: www.AreYouDense.org, www.AreYouDenseAdvocacy.org


 May 22, 2026
May 22, 2026 









