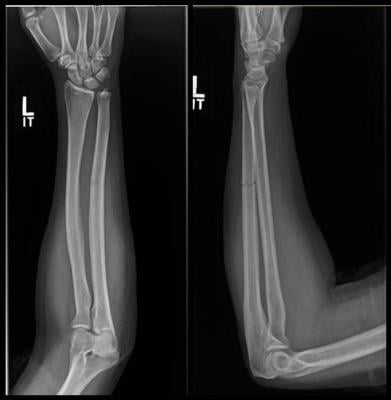
X-ray shows fracture to the ulna bone of the forearm. Image courtesy of RSNA
November 30, 2020 — Up to one-third of adult women who sustain a non-displaced fracture to the ulna bone of the forearm may be victims of intimate partner violence, according to a study being presented at the annual meeting of the Radiological Society of North America (RSNA). The findings underscore the need to screen for intimate partner violence in women with these types of injuries, researchers said.
Fractures to the ulna, the bone on the pinkie side of the forearm, often occur when people hold up their hands to protect their faces from being struck with an object. These breaks are referred to as “nightstick fractures,” because they are frequently seen in people who try to block blows from nightsticks wielded by police officers.
Bharti Khurana, M.D., a radiologist at Brigham and Women’s Hospital in Boston and senior author of the study, had observed these fractures in her practice for years, mostly in men. But it was the occasional woman she saw that raised questions.
“I would see these types of injuries in men, but once in a while I would see them in women,” Khurana said. “I never correlated it with intimate partner violence until recently. I shared my thoughts with our orthopedic surgeons and, with their interest and support, decided to pursue the study.”
For the study, Khurana and colleagues searched electronic medical records from six hospitals for isolated ulnar fractures in women ages 18 to 50. They identified 62 patients, average age 31. Of those, 12 were confirmed for intimate partner violence and another eight were suspected of intimate partner violence.
Analysis of the radiographs demonstrated that intimate partner violence was strongly associated with minimally displaced fractures.
“The radiological characteristics we were looking at were the location of the fracture, the pattern of the fracture in terms of how it broke, and the displacement of the fracture,” said study lead author David Sing, M.D., an orthopedic surgery resident at Boston Medical Center. “Out of all those things, what we usually saw was a minimally displaced fracture, meaning the bone is broken all the way through but has not shifted significantly.”
Confirmed cases were also linked with homelessness and previous visits to the emergency department with musculoskeletal injuries.
Women with ulnar fractures from intimate partner violence who are reluctant to report the crime will often attribute their injuries to a fall, Khurana said. However, she noted, falls are much more likely to result in a fracture of the radius, the other bone of the forearm.
This observation was supported by the study, as all the patients who were not victims of intimate partner violence had ulnar fractures from motor vehicle accidents or accidental striking, such as from crashing into a tree while skiing. Of the eight patients where intimate partner violence was suspected, four reported a fall.
“It’s actually rare to break your ulna in a fall,” Khurana said. “If a radiologist is seeing an ulnar fracture that is non-displaced, and the woman says she had a fall, it’s actually quite concerning for intimate partner violence.”
The study results suggest that intimate partner violence screening may be underutilized. Formal documentation of intimate partner violence evaluation or screening was completed in only 40% of confirmed/suspected intimate partner violence cases in the study. According to the researchers, radiologists who observe non-displaced ulnar fractures can help close that shortfall by letting the emergency department physician or orthopedic surgeon know that the fracture is often seen in intimate partner violence. The ordering physician can then look at the patient’s clinical history to see if there is anything suspicious.
“Careful analysis of previous imaging exams may also help radiologists confirm their suspicion of intimate partner violence,” said study co-author Rahul Gujrathi, M.D., a radiology fellow at Brigham and Women’s Hospital.
In the study, for instance, historical imaging analysis alone was able to raise suspicion in 75% of clinically confirmed intimate partner violence patients.
“We have resources that we can provide to the patients who are stuck in that situation,” Sing said. “It’s especially important during COVID-19, where we’ve seen the rate of intimate partner violence go up with people trapped at home with their abusers.”
Dr. Khurana, who devotes much of her research to identifying radiological signs of intimate partner violence, believes that a more widespread awareness of the association between ulnar fractures and intimate partner violence will help provide earlier detection and intervention.
“The sooner we can address and change the behavior, the better,” she said. “Just like radiologists want to diagnose cancer as early as possible, it’s the same thing with this. If we diagnose early, we have a better chance to break the cycle of violence.”
This research was partially funded by a Gillian Reny Stepping Strong Innovator Award, Brigham Health. Co-authors are George Dyer, M.D., Mitchel B. Harris, M.D., Camden Bay, Ph.D., Irene Chen, Steven E. Seltzer, M.D., Giles W. Boland M.D., and Paul Tornetta, III, M.D.
For more information: www.rsna.org


 May 26, 2026
May 26, 2026 









