Greg Freiherr has reported on developments in radiology since 1983. He runs the consulting service, The Freiherr Group.
Legislating Women’s Health: A Chance for Radiologists to Step In
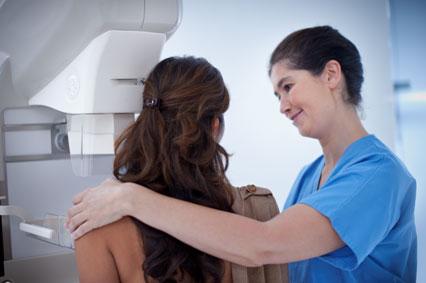
States increasingly are mandating that physicians inform patients with dense breasts that mammography may miss some signs of cancer. This trend provides radiologists with a chance to take a more direct role in patient care.
Five states now mandate physicians to inform women with dense breasts that mammography may be of limited value to them. These states — Connecticut, Virginia, Texas, California and New York — require physicians to advise patients that complementary imaging studies, such as ultrasound or MRI, may be needed, if dense fibroglandular tissues are likely to obscure the mammographic signs of cancer. Their laws, however, do not say specifically who should inform patients — the physician who interprets the mammogram or the physician who regularly attends the patient.
This quandary is ready-made for radiologists. Because mammography is a screening exam, patients are seldom referred to radiologists for such studies. Instead the patients themselves typically make the appointments and are then informed by the radiologist of the results.
Only a month ago, radiologists were encouraged by the RSNA president to consider imaging patients on their own and to take a more active role in their care. The recognition of breast density as a complicating factor in women’s health presents the opportunity to act on this advice.
Radiologists can play a pivotal role in the care of women with dense breasts, according to Stamatia Destounis, M.D., an attending radiologist at Elizabeth Wende Breast Clinic in Rochester, New York.
“We want to do this right — we want to educate and inform patients without causing a lot of undue stress and anxiety and fear and we have to try to do (additional testing) that is appropriate in a cost-effective manner,” she told me.
Ultrasound and MRI are the two options. Ultrasound is low cost and widely available. But it is very sensitive and can produce false negatives demonstrated on biopsy. MRI might be indicated, if patients are high-risk due to family history or the presence of the BRC1 or BRC2 gene. This modality is also very sensitive and can lead to biopsies that are negative.
Clearly, to provide optimal care, several challenges must be met. One is to identify patients with dense breasts, identification that is heavily dependent on the skills of the interpreter. The second challenge is to choose the best method for additional testing. The third is correctly interpreting follow-on tests to minimize the number of biopsies. The fourth is to maintain communication with the patient throughout the diagnostic process — to keep patients informed and not unduly alarmed.
Rhetorically, you might ask, who better to meet these challenges than radiologists? And what better time to act than now, when organized radiology is pushing its members to take a higher profile in the care of patients?
The question without an obvious answer is whether radiologists, who for so long have taken a back seat in the practice of medicine, will act on this opportunity.


 May 22, 2026
May 22, 2026