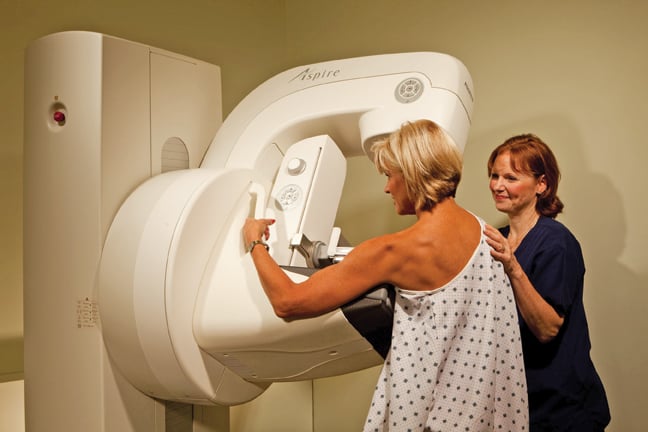
The Fuji Aspire FFDM system
Digital mammography (DM) is a field in which advances are constantly being made and new trends evolve. During a scientific session at RSNA 2011, John M. Lewin, M.D., discussed recent trends and how they have changed during the past year.
One trend, Lewin said, was that mammography screening in general is still under attack. Myriad studies have argued for and against mammography, citing false positives, mortality rates, number of life-years gained, bang for the buck (and bang versus buck) and other factors, such as at what age women should be screened, how often they should be screened — and whether they should be screened at all. Lewin has a positive view of mammography screening, referring to “our side” when citing a study indicating that 80 percent of women feel mammograms are vital to their health.
A second trend is about breast density reporting legislation. The facts, Lewin says, are these: Breast density is a risk factor for breast cancer, and mammography is less sensitive in dense breasts. It is still conjecture that adding more tests to mammography will decrease breast cancer mortality rates, but a number of groups (including areyoudense.org) advocate women knowing their breast density.
There is federal legislation in the works requiring radiologists to report breast density. If passed, it would require mammography reporting packages to accommodate breast density in their patient letters about test results. Breast density analysis software would be amped up. Automated whole-breast ultrasound screening would become the norm, with devices that would screen without the radiologist’s involvement, eliminating user variability; the radiologist would simply read a video loop.
Trend No. 3 is having more choices in approved devices, both pre-market approval (PMA) and 510(k), as well as increased concern about radiation. Lewin said not much changed with this over the past year, with radiation concerns focused on computed tomography (CT) and imaging children (where he believes the focus should lie), except for a paper published in 2010 noting the high whole-body radiation dose from sestamibi breast scanning or breast positron emission mammography (PEM). However, dose has since been lowered by improved technology and dual-head units.
Another trend in which not much has changed is new detectors; Lewin said that except for in labs, there really have not been advances here in the past year. One change — Philips purchased Sectra’s mammography system, which uses photon counting or multiple-slit scanning.
Last year, a fifth trend was that mammography moved from 2-D to 3-D in the realms of tomosynthesis and breast CT. Hologic received U.S. Food and Drug Administration (FDA) approval after five years of waiting; the approval is for using tomosynthesis in combination with 2-D mammography. However, using both of these in conjunction almost doubles the dose of a 2-D mammogram, so there is a cost to getting more images and fewer artifacts.
Lewin speculated about eliminating the 2-D view to reduce dose by using something he called a “2-D synthetic view,” in which the tomosynthesis data is used to create a view that simulates a 2-D mammogram and allows one to see calcification distributions that might be difficult to see on tomo slices. He stated that a method like this might allow the FDA’s requirement to be dropped.
Adding contrast is yet another DM trend. The hypothesis behind contrast-enhanced digital mammography (CEDM) is that by using intravenous iodinated contrast with digital mammography, occult cancers can be made visible and breast cancers can appear enhanced on magnetic resonance imaging (MRI) and CT.
However, there are a few stumbling blocks: The contrast resolution of DM is far lower than CT and MRI, and breast compression limits the image to a single view and inhibits blood flow, thus occluding the flow of contrast. As an alternative to CEDM, Lewin named dual-energy subtraction, in which one takes two mammograms of different energies — both of them after the contrast is already in — and uses an algorithm to perform a weighted subtraction. The breast does not need to be immobilized during contrast, only while imaging, and images can be taken one after another until the contrast dissipates.
Another 2011 trend that has not made many new advances is combining exams — for example, mammography plus ultrasound, or mammography plus nuclear imaging, such as positron emission tomography (PET). Lewin said nothing much happened over the last year; automated screening ultrasound continues to proliferate (not necessarily with mammography in direct combination, although that is in the works). But this may not really take off until screening becomes a paid indication under Medicare.
The eighth and final trend Lewin discussed was tailored screening, which ties into the breast density legislation mentioned above. Breast density legislation will open the floor for even more tailored screening in terms of population — for instance, if there is a way to determine who is more likely to have cancer. However, tailored screening has never been studied in randomized controlled trials, so there is no evidence for or against it.
Lewin named several events to watch for in the coming year. He expects that tomosynethsis will come out with a synthetic 2-D view, so 2-D imaging could be scrapped altogether; that other tomosynthesis units will be approved; that more states will approve breast density legislation; and that contrast mammography will replace MRI in some cases.


 May 22, 2026
May 22, 2026 









